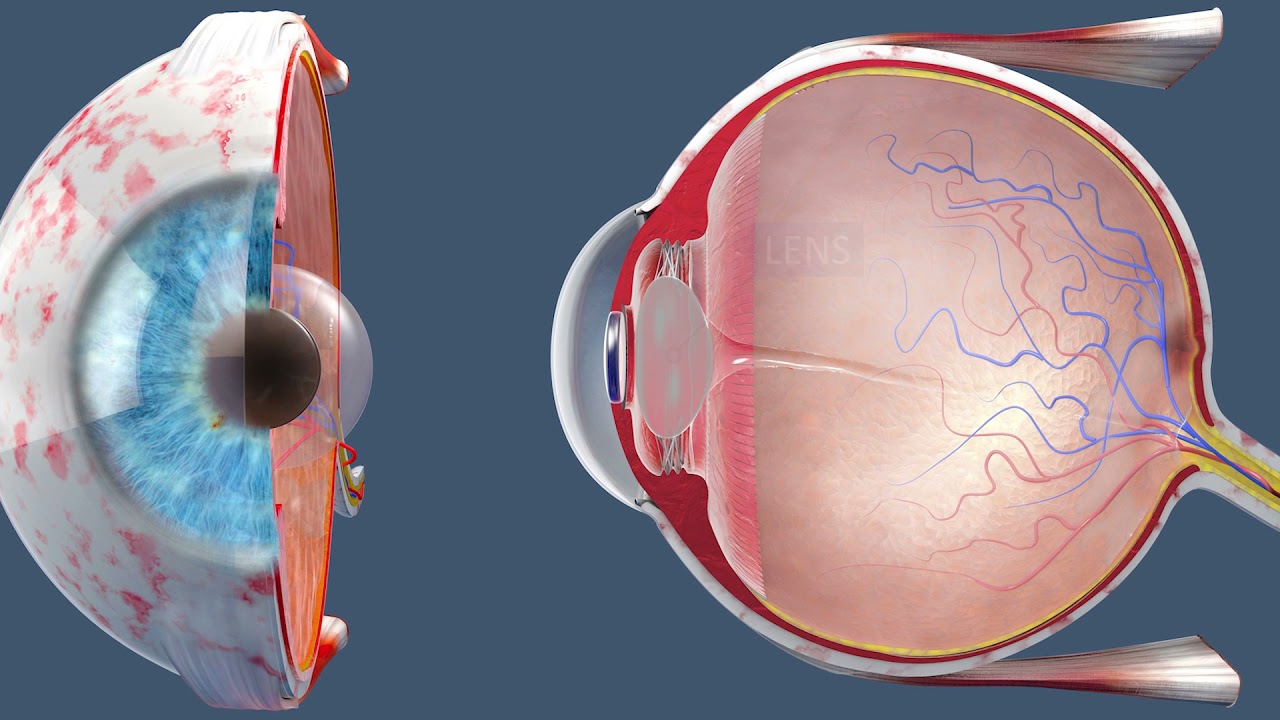
Surgery Videos
Ettore Vulcano, MD, Foot and Ankle Orthopedic Surgeon at Mount Sinai West, discusses a new minimally invasive bunion surgery that has patients walking immediately after surgery, and getting back to an active lifestyle much quicker than with the traditional surgery.

For more information about Mohs surgery, please visit https://cle.clinic/3x7CRTy
Mohs surgery is a highly effective skin cancer removal procedure that takes just a few hours. It is most often used to treat basal cell and squamous cell carcinomas, the two most common skin cancers.
Chapters:
0:00 How effective is Mohs Surgery?
0:23 When is Mohs Surgery used?
0:50 How does Mohs Surgery work?
1:55 Does Mohs Surgery cure skin cancer?
2:06 How long is the recovery period after Mohs Surgery?
Resources:
Skins Cancer: https://cle.clinic/3G2MMM8
How Skin Cancer Is Found and Removed — At the Same Appointment: https://cle.clinic/3r9Wzu6
The Best Strategies To Reduce Your Risk of Skin Cancer: https://cle.clinic/38Bazqn
The information in this video was accurate as of 4.8.2022 and is for information purposes only. Consult your local medical authority or your healthcare practitioner for advice.
▶Share this video with others: https://youtu.be/aCV1UZ0Yj-o
▶Subscribe to learn more about Cleveland Clinic:
https://www.youtube.com/user/C....levelandClinic?sub_c
#ClevelandClinic #MohsSurgery #SkinCancer

Dr. Debbie Song at Gillette Children's describes in detail selective rhizotomy surgery.
A selective dorsal rhizotomy is an operation performed to treat spasticity. It is thought that high tone and spasticity arise from abnormal signals that are transmitted through sensory or dorsal nerve roots to the spinal cord. In a selective dorsal rhizotomy we identify and cut portions of the dorsal nerve roots that carry abnormal signals thereby disrupting the mechanisms that lead to spasticity. Potential patients go through a rigorous assessment that includes an in-depth gait and motion analysis as well as a physical therapy evaluation.
They are evaluated by a multidisciplinary team that includes a pediatric rehabilitation doctor, a neurosurgeon, and an orthopedist, Appropriate patient selection is vital. Ideal candidates for selective dorsal rhizotomy are children who are between four and ten years of age, have a history of being born prematurely, and have a diagnosis of diplegia cerebral palsy. These patients usually walk independently or with the assistance of crutches or a walker. They typically function at a level one, two, or three in the gross motor function classification system or gmfcs. A selective dorsal rhizotomy involves the coordinated efforts of the neurosurgery, physiatry, anesthesia and nursing teams. The operation entails making an incision in the lower back that is approximately six to eight inches long. We perform what we call a laminoplasty in which we remove the back part of the spinal elements from the lumbar one or l1 to l5 levels. At the end of the procedure the bone is put back on. We identify and open up the Dural sac that contain the spinal fluid spinal cord and nerve roots. Once the Dural sac is opened ,we expose the lumbar and upper sacral nerve roots that transmit information to and from the muscles of the lower extremities.
At each level we isolate the dorsal nerve root, which in turn is separated into as many as 30 smaller thread light fruitlets.
Each rootlet is then electrically stimulated. Specialized members of the physiatry team look for abnormal responses in the muscles of the legs as each rootless is being stimulated. If an abnormal response is observed then the rootlet is cut.
If a normal response is observed, then the rootlet is not cut. We usually end up cutting approximately 20 to 40 percent of the rootlets. The Dural sac is sutured closed and the l1 through l5 spinal elements are put back into anatomic position, thus restoring normal spinal alignment. The overlying tissues and skin are then closed and the patient is awoken from surgery. The entire operation takes between four and five hours. A crucial component to the success of our rhizotomy program is the extensive rehabilitation course following surgery. With their tone significantly reduced after a rhizotomy, patients relearn how to use their muscles to walk more efficiently through stretching, strengthening, and gait training. Approximately one to two years after a rhizotomy patients undergo repeat gait and motion analysis. The orthopedic surgeons assess the need for interventions to correct bone deformities, muscle contractures, poor motor control, impaired balance, or other problems related to cerebral palsy.
At Gillette we work closely with patients and families to ensure that our selective dorsal rhizotomy program meets their goals for enhancing their function and improving their quality of life.
VISIT https://www.gillettechildrens.org/ to learn more
0:00 Why choose selective dorsal rhizotomy?
0:56 Who is a good candidate for selective dorsal rhizotomy?
1:31 What does a selective dorsal rhizotomy entail?
3:26 What is recovery from selective dorsal rhizotomy like?

This video demonstrates a manual small incision cataract surgery using a Blumenthal technique, in a white cataract.
Surgeon: Dr. Rishi Swarup, FRCS, Medical Director & Senior Consultant, Swarup Eye Centre, India
For Employees of Hospitals, Schools, Universities and Libraries: Download 8 FREE medical animations from Nucleus by signing up for a free trial: http://nmal.nucleusmedicalmedi....a.com/free-trial-mem
Biology students: Subscribe to the Nucleus Biology channel to see new animations on biology and other science topics, plus short quizzes to ace your next exam: https://bit.ly/3lH1CzV
This medical animation depicts Laser Eye Surgery, a procedure that permanently changes the shape of the cornea, the clear covering over the front of the eye.
#lasik #eye #cornea
ANCE00185

Learn Basic Laparoscopic Surgery, the components of a laparoscopic surgical setup, optimal positioning and ergonomics in laparoscopic surgery, and much more. Check out the full course for free here: https://www.incision.care/free-trial
What is Laparoscopic Surgery:
Laparoscopic surgery describes procedures performed using one or multiple small incisions in the abdominal wall in contrast to the larger, normally singular incision of laparotomy. The technique is based around principles of minimally invasive surgery (or minimal access surgery): a large group of modern surgical procedures carried out by entering the body with the smallest possible damage to tissues. In abdominopelvic surgery, minimally invasive surgery is generally treated as synonymous with laparoscopic surgery as are procedures not technically within the peritoneal cavity, such as totally extraperitoneal hernia repair, or extending beyond the abdomen, such as thoraco-laparoscopic esophagectomy. The term laparoscopy is sometimes used interchangeably, although this is often reserved to describe a visual examination of the peritoneal cavity or the purely scopic component of a laparoscopic procedure. The colloquial keyhole surgery is common in non-medical usage.
Surgical Objective of Laparoscopic Surgery:
The objective of a laparoscopic approach is to minimize surgical trauma when operating on abdominal or pelvic structures. When correctly indicated and performed, this can result in smaller scars, reduced postoperative morbidity, shorter inpatient durations, and a faster return to normal activity. For a number of abdominopelvic procedures, a laparoscopic approach is now generally considered to be the gold-standard treatment option.
Definitions
Developments of Laparoscopic Surgery:
Following a number of smaller-scale applications of minimally invasive techniques to abdominopelvic surgery, laparoscopic surgery became a major part of general surgical practice with the introduction of laparoscopic cholecystectomy in the 1980s and the subsequent pioneering of endoscopic camera technology. This led to the widespread adoption of the technique by the early- to mid-1990s. The portfolio of procedures that can be performed laparoscopically has rapidly expanded with improvements in instruments, imaging, techniques and training — forming a central component of modern surgical practice and cross-specialty curricula [2]. Techniques such as laparoscopically assisted surgery and hand-assisted laparoscopic surgery have allowed the application of laparoscopic techniques to a greater variety of pathology. Single-incision laparoscopic surgery, natural orifice transluminal endoscopic surgery, and minilaparoscopy-assisted natural orifice surgery continue to push forward the applications of minimally invasive abdominopelvic techniques; however, the widespread practice and specific indications for these remain to be fully established. More recently, robotic surgery has been able to build on laparoscopic principles through developments in visualization, ergonomics, and instrumentation.
This Basic Laparoscopic Surgery Course Will Teach You:
- Abdominal access techniques and the different ways of establishing a pneumoperitoneum
- Principles of port placement and organization of the operative field
- Key elements of laparoscopic suturing, basic knotting and clip application
Specific attention is paid to the following hazards you may encounter:
- Fire hazard and thermal injury
- Lens fogging
- Contamination of insufflation system
- Complications from trocar introduction
- Limitations of Veress needle technique
- Limitations of open introduction technique
- Complications of the pneumoperitoneum
- Gas embolism
- Mirroring and scaling of instrument movements
- Firing clip applier without a loaded clip
The following tips are designed to improve your understanding and performance:
- Anatomy of a laparoscope
- Checking for optic fiber damage
- "White balance" of camera
- Checking integrity of electrosurgical insulation
- Access at Palmer's point
- Lifting abdominal wall before introduction
- Confirming position of Veress needle
- Umbilical anatomy
- Identification of inferior epigastric vessels under direct vision
- Translumination of superficial epigastric vessels
- Selection of trocar size
- Aiming of trocar
- Working angles in laparoscopic surgery
- Choice of suture material
- Instruments for suturing
- Optimal ergonomics for suturing
- Extracorporeal needle positioning
- Optimal suture lengths
- "Backloading" needle
- Intracorporeal needle positioning
- Hand movements when suturing
- Optimal positioning of scissors
- Extracorporeal knot tying
- Visualization of clip applier around target structure
- Common clip configurations
Thousands of Canadians undergo surgery every year, so how can you best prepare? The first step is having a dialogue, says Sunnybrook anesthesiologist Dr. Colin McCartney. Read the blog for more: http://sunnyview.sunnybrook.ca
Cleft palate is among the most common birth defects affecting children in North America. The incomplete formation of the roof of the mouth can occur individually, or in addition to cleft lip. Cleft palate repair is a type of plastic surgery to correct this abnormal development both to restore function and a more normal appearance. This video explains what to expect for families scheduled for cleft palate surgery at the Craniofacial Anomalies Program at University of Michigan C.S. Mott Children's Hospital.
Learn more about our program at http://www.mottchildren.org/craniofacial

Our mission: Empower you with the tools and support you need for weight loss and live a healthier life. Get started on your weight loss journey today: https://bit.ly/2Ms4JaX
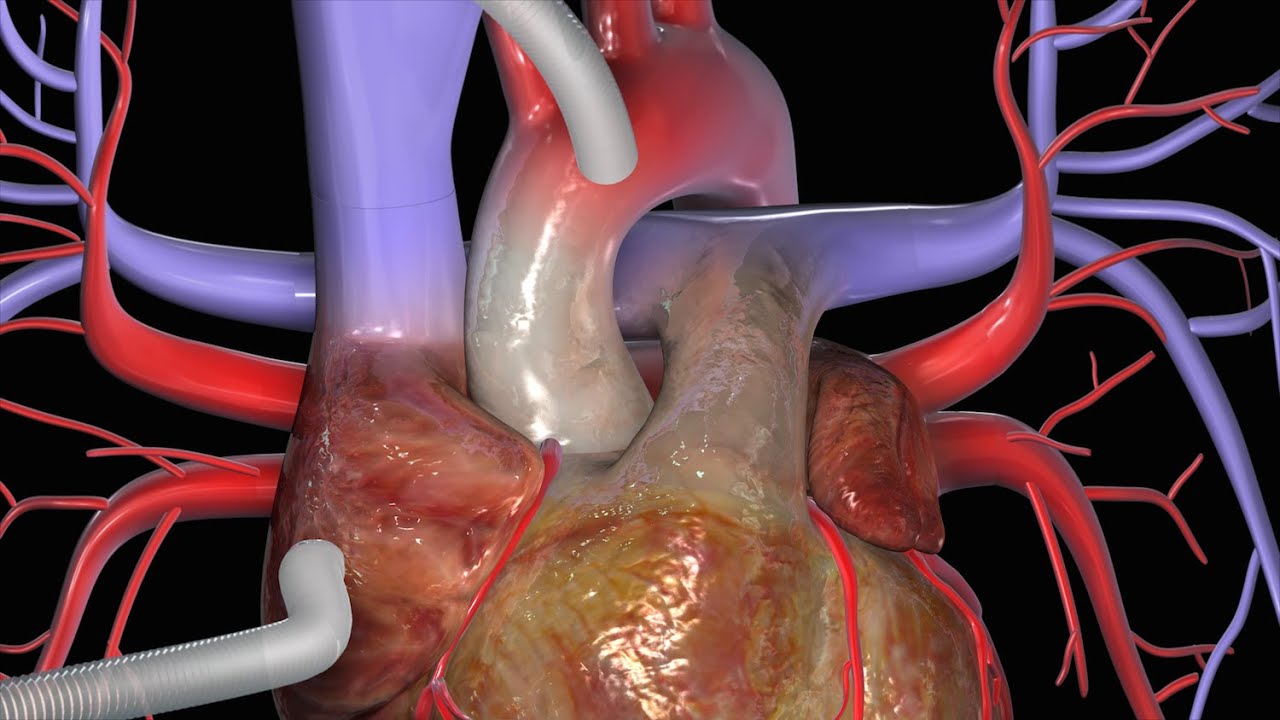
This video has been updated to include an alternate name for the internal thoracic arteries. View the updated video here: https://youtu.be/kxc22Fjd1NQ
For Employees of Hospitals, Schools, Universities and Libraries: Download 8 FREE medical animations from Nucleus by signing up for a free trial: http://nmal.nucleusmedicalmedi....a.com/free-trial-mem
Biology students: Subscribe to the Nucleus Biology channel to see new animations on biology and other science topics, plus short quizzes to ace your next exam: https://bit.ly/3lH1CzV
This video, created by Nucleus Medical Media, shows a coronary artery bypass graft (CABG) procedure used to combat coronary artery disease. Beginning with a midline sternal incision, the heart is connected to a perfusion machine which will take over the duties of the heart while the surgery takes place. Two different grafts are used to bypass the blocked coronary arteries: the internal thoracic artery from inside the chest wall, and the saphenous vein from the leg. After the procedure, the heart is shocked to restart its beating. A drainage tube is left at the incision site to drain away excess fluid. The animation continues to show two other types of approaches to a coronary artery bypass graft, off-pump bypass surgery and minimally invasive bypass surgery.
This is similar to the procedure performed on former president Bill Clinton and former California governor Arnold Schwarzenegger.
#HeartBypassSurgery #CABG #heart
ANCE00199

If a fetal lung lesion is causing heart failure, fetal surgery may be performed to remove the CCAM before birth. http://fetalsurgery.chop.edu
N. Scott Adzick, MD, Mark Johnson, MD, and Holly Hedrick, MD, experts from the Center for Fetal Diagnosis and Treatment at Children’s Hospital of Philadelphia, explain when fetal intervention for CCAM is recommended, the various approaches that may be used to treat the most complex fetal lung lesions before birth, and how these procedures are performed.
One concern with fetal lung lesions is that they take up space in the chest. If the lung mass grows and pushes the heart and other organs out of place, it can lead to complications such as fetal hydrops (heart failure in the fetus). If this happens, a fetal surgery procedure may be performed to remove the CCAM before birth.
In other cases, an EXIT procedure may be performed to partially deliver the baby, so the team can remove the mass before the baby is fully delivered.
In this video series, parents, nurses and doctors from Children’s Hospital of Philadelphia’s Center for Fetal Diagnosis and Treatment talk about the different types of fetal lung lesions like congenital cystic adenomatoid malformation (CCAM) and bronchopulmonary sequestration (BPS), the importance of accurate diagnosis and monitoring, and the most advanced treatment options currently available. They also discuss follow-up care and long-term outcomes for babies diagnosed with fetal lung lesions.
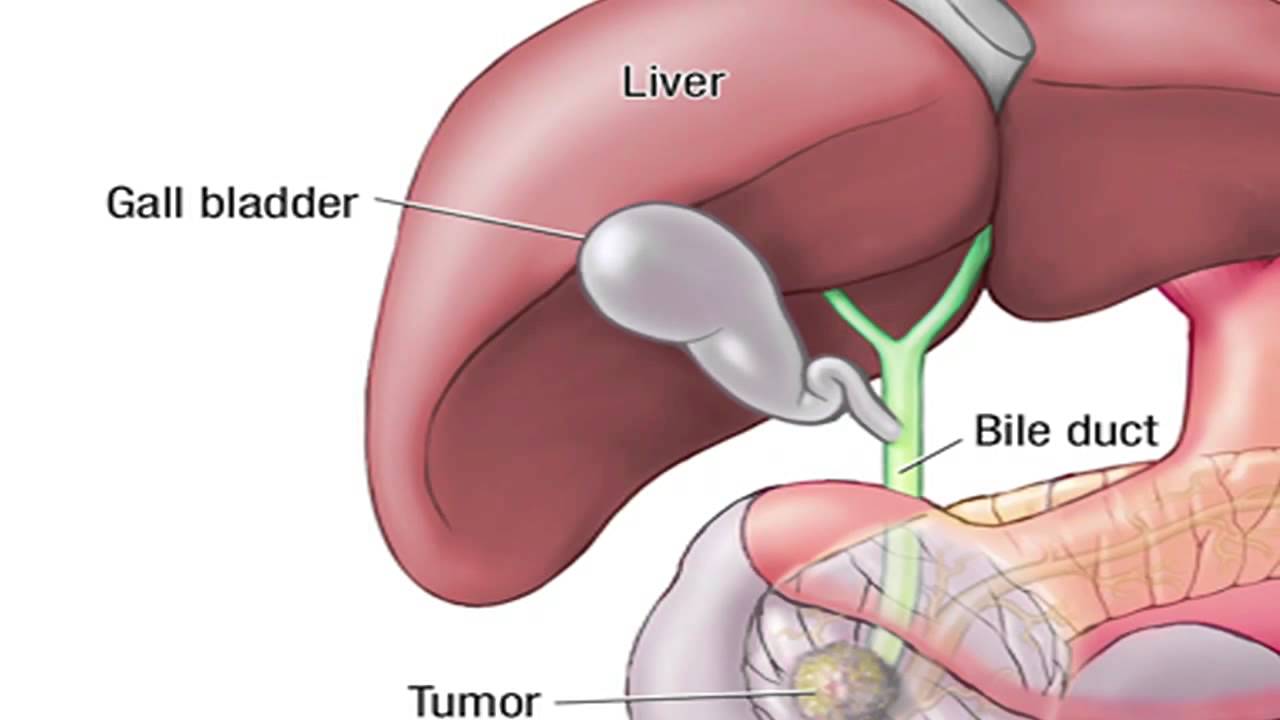
Dr. Horacio Asbun, Mayo Clinic in Florida, explains the Whipple procedure using this animated graphic of a pancreas. Cancer of the pancreas affects 45,000 people every year in the U.S., and it is the fourth leading cause of cancer-related deaths. The five-year overall survival rate if a tumor is detected early and surgically removed is 22 percent, versus 6 percent without early detection and surgery. To learn more, visit http://mayocl.in/2zk7FDi.
This video in Spanish/español: https://www.youtube.com/watch?v=N_zWboNMKWk

A brain surgery called a craniectomy is performed to remove a part of your skull in order to relieve pressure in an area when your brain swells from a traumatic brain injury. It is also performed to treat medical conditions that cause your brain to swell or bleed that can be caused by an aneurysm, brain tumor or other cancer.
This 3d animation shows how the surgical procedure decreases intracranial pressure (ICP), intracranial hypertension (ICHT), or heavy bleeding (also called hemorrhaging) inside your skull. If left untreated, pressure or bleeding can compress your brain and push it down onto the brain stem. This can be fatal or cause permanent brain damage.
Brain surgery is a very serious procedure under any circumstances, but a craniectomy is done when there is an immediate risk to the brain and neurological function due to severe brain injury or stroke.
For more information about custom 3D animation depicting surgery, please visit https://www.amerra.com/.
Watch additional medical animations:
Accessing an implantable port training - 3D animation: https://youtu.be/xSTpxjyv4O4
Open Suctioning with a Tracheostomy Tube - 3D animation: https://youtu.be/wamB7jpWCiQ
Ventriculostomy Brain Surgery - 3d animation: https://youtu.be/pUy0YDzVNzs
Suctioning the endotracheal tube - medical animation: https://youtu.be/pN6-EYoeh3g
Functional endoscopic sinus surgery (FESS) - 3D animation: https://youtu.be/qKTRyowwaLA
How to insert a nasogastric tube for NG intubation - 3d animation: https://youtu.be/Abf3Gd6AaZQ
Oral airway insertion - oropharyngeal airway technique - 3D animation: https://youtu.be/caxUdNwjt34
Nasotracheal suctioning (NTS) - 3D animation: https://youtu.be/979jWMsF62c
Learn about hemorrhoids with #3d #animation: https://youtu.be/R6NqlMpsiiY
LASIK eye surgery - 3D animation: https://youtu.be/Bb8bnjnEM00
CPR cardiopulmonary resuscitation - 3D animation: https://youtu.be/G87knTZnhks
What are warts (HPV)? - 3D animation: https://youtu.be/guJ1J7rRs1w
How Macular Degeneration Affects Your Vision - 3D animation: https://youtu.be/ozZQIZ_52YY
NeoGraft hair transplant procedure – animation: https://youtu.be/C-eTdH2UPXI

Orthopedic spine surgeons and vascular surgeons at UW Health in Madison, WI work together to perform minimally invasive anterior lumbar interbody fusion (Mini-ALIF). With this type of spinal fusion surgery, patients have smaller incisions, usually spend less time in the hospital and typically return to daily activities more quickly. Learn more https://www.uwhealth.org/ALIF

In this video, Dr. Robert Rozbruch, chief of Limb Lengthening and Complex Reconstruction at Hospital for Special Surgery performs an osseointegration after a primary amputation. The patient, a 40 year old woman, had chronic nerve pain and compromised function of her residual limb.
For more information, visit: https://www.limblengthening.com/
https://www.hss.edu/limblengthening
https://www.hss.edu/LSARC
https://www.facebook.com/limblengtheningNYC
https://www.instagram.com/limblengthening
https://www.twitter.com/limblengthen
https://www.youtube.com/channe....l/UC-JL_X6ALjZXiXtcP
key words: Osseointegration, Amputee, Amputation, Limb Replacement, Tibia, Osseointegration

Watch to learn more about what happens during a stent procedure.
More information about this procedure and other heart care at BJC: https://www.bjc.org/Services/M....edical-Services/angi