Top videos

Head to SimpleNursing’s OFFICIAL website here: https://bit.ly/3TzGwF0
SimpleNursing memberships have 1,200+ animated videos, 900+ colorful study guides, 3,000+ practice questions, and more! See why SimpleNursing is trusted by over 1,000,000 nursing students.
Today’s video is all about peritoneal dialysis vs hemodialysis for Nursing Students and NCLEX Review.
Two common treatments for kidney failure are hemodialysis and peritoneal dialysis. With the right nursing assessments and interventions, your kidney failure patient can have a better chance at recovery.
We’re going over the roles that potassium plays in each of these two types of dialysis, as well as how stenosis monitoring can be used to prevent complications.
00:00 Introduction
01:10 Hyperkalemia in Hemodialysis
02:27 Assessing Fluid Status
03:35 Medications to Hold Before Hemodialysis
04:50 Medications Removed During Hemodialysis
05:45 Dialysis Disequilibrium Syndrome
07:20 Caring for a Fistula
09:12 Avoiding Fistula Complications
10:35 Peritoneal Dialysis
11:23 Peritonitis Risk
12:31 Respiratory Distress With Peritoneal Dialysis
13:39 Repositioning With Outflow Problems
#KidneyFailure #Dialysis #Hemodialysis #Peritonealdialysis

Warren Pettaway of Detroit knew he needed to have his left knee checked out when he could no longer keep up while officiating basketball. The pain got so bad that running up and down the court or quickly changing directions was too much for him to continue doing what he loved.Only three weeks post-surgery, Warren is ready to get back in the game. He is able to move without issue and is getting things done around the house. He makes sure to do his therapy as directed and is exercising on his own in the gym. To learn more visit https://www.henryford.com/serv....ices/joint-replaceme
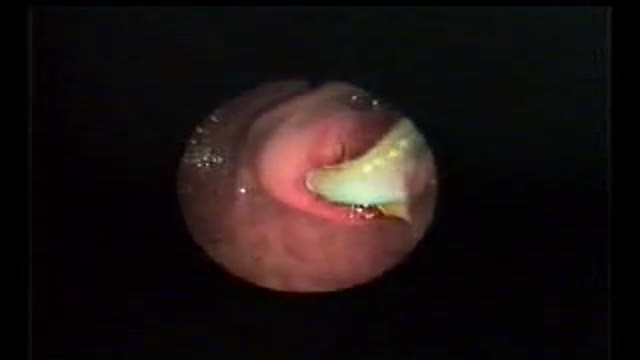
A 30 YEAR WOMEN WITH INTRACTABLE BILIARY COLIC
CASE REPORT: This 30 year women developed severe pain right upper quadrant for last 10 days. She sought many consultations and was given intravenous analgesics both (nonnarcortic and narcotic). Pain did not subside and she sought my consultation. Examination revealed her to be in agony with severe upper abdominal pain. General physical examination was otherwise unremarkable. Abdominal examination revealed mild tenderness in right hypochondrium with doubtful Murphy's sign. Urgent abdominal ultrasound showed a linear structure in bile ducts making slow writhing movements. The structure had an anechoic tube (alimentary canal) inside suggestive of a large Ascarid. Urgent ERCP was performed and bile duct and pancreatic duct cannulated selectively. Pancreatic duct was normal. Bile ducts contained a long linear filling defect extending from lower end of common bile duct to right intrahepatic duct (see image gallery for ERCP plate). A basket was introduced in the duct (see video clip) and the linear structure was engaged with soft closure and extracted out of the bile duct. Accompanying the basket was a 25 cm thick highly motile Ascarid. To recover the worm, endoscope was withdrawn along with the basket and the friendly catch. While the endoscope was being withdrawn and the basket was in the duodenum with the worm out of bile duct, patient indicated of relief of abdominal pain. A relook cholangiogram showed no more structures in the duct. She was given antihelmintic therapy and passed hundreds of worms with the feces. The worms recovered form stools were both male and female population and varied in length and size. However the lone worm recovered form bile ducts was the longest and the thickest male worm. The phenomenal behavior of this ubiquitous infection remains unexplained.