热门视频

► Sign up here and try our FREE content: http://lectur.io/freecontentyt
► If you’re an medical educator or faculty member, visit: http://lectur.io/medytb2u
This video “Respiratory Histology” is part of the Lecturio course “Histology” ► WATCH the complete course on http://lectur.io/respiratoryhistology
► LEARN ABOUT:
- The cellular components of epithelium
- Structure and function of the conchae
- The cellular components of olfactory epithelium
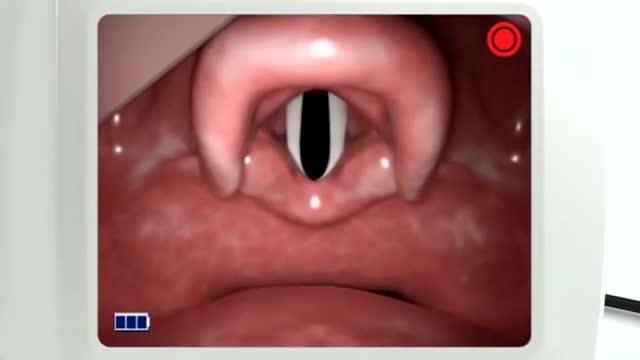
- Components of the true vocal cord
- Function of the epiglottis
- The difference between bronchus, bronchiole, respiratory bronchiole
- Alveolar duct and Alveolar sac
- Components that make up the interalveolar septum
- Type I and Type II of alveolar cells, macrophages and endothelium
- Two separate blood supplies to the lungs and their functions
- Summary of the functions and the system of the respiratory system
► THE PROF: Your lecturer is Professor Geoff Meyer. He is currently teaching at the School of Anatomy, Physiology and Human Biology at the University of Western Australia (UWA). As a leading anatomy and histology expert he is also coordinating the Federative International Program for Anatomical Terminologies (FIPAT) of the International Federation of Associations of Anatomists (IFAA). Besides medical research on the ovarian function, steroidogenesis, corpus luteum, angiogenesis, and microcirculation, Geoff Meyer’s research activities also focus on developing innovative, computer-aided learning and teaching tools. For his inventiveness, Geoff Meyer has received a number of awards, including the Australian University Teaching Award.
► LECTURIO is your single-point resource for medical school:
Study for your classes, USMLE Step 1, USMLE Step 2, MCAT or MBBS with video lectures by world-class professors, recall & USMLE-style questions and textbook articles. Create your free account now: http://lectur.io/respiratoryhistology
► INSTALL our free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► READ TEXTBOOK ARTICLES related to this video:
Histology of the Airways
http://lectur.io/respiratoryhistoloyarticle
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribe
► WATCH MORE ON YOUTUBE: http://lectur.io/playlists
► LET’S CONNECT:
• Facebook: https://www.facebook.com/lectu....rio.medical.educatio
• Instagram: https://www.instagram.com/lecturio_medical_videos
• Twitter: https://twitter.com/LecturioMed
• Pinterest: https://www.pinterest.de/lecturiomedical
• LinkedIn: https://www.linkedin.com/company/lecturio-medical/
0:00 Introduction
2:00 Respiratory system Summary of structure and function
3:32 Conducting portion
7:49 The Nasal cavities
11:27 The nasal cavity
13:06 Respiratory mucosa
15:26 Olfactory mucosa
17:13 Olfactory receptor
21:16 The larynx (and the epiglottis)
25:44 The trachea
29:16 The bronchi
31:35 Bronchiole
38:50 Alveolus
40:45 Air blood barrier
43:36 Alveolar macrophages
45:35 Blood supply and lymphatic drainage of the pulmonary lobule

Shane Shapiro, M.D., orthopedic physician at Mayo Clinic in Florida, performs a bone marrow aspiration and concentration for BMAC/stem cell injection into arthritic knees. This procedure is part of a Mayo Clinic IRB approved, FDA monitored clinical research trial which can be searched on at http://ClinicalTrials.gov.
Mayo Clinic and the Mayo Center for Regenerative Biotherapeutics is studying biologically based non-surgical treatments for osteoarthritis. One such treatment is the harvesting of the patient's own stem cells from their bone marrow.
"In our procedure we draw cellular rich bone marrow from both sides of the pelvis. We then filter the resulting product and concentrate the stem cells and their corresponding growth factors. Using an ultrasound to image the knee joint, we are then able to precisely inject the cells into the arthritic knee. We are currently demonstrating that this procedure is safe and can relieve pain. We also hope to be able to slow the progression of the degenerative joint disease and perhaps one day regrow cartilage in the arthritic joint."
------
Hear Dr. Shapiro discus this procedure in detail here: http://youtu.be/8Djpsc66hKI
Learn more about the Mayo Clinic Center for Regenerative Biotherapeutics here: http://goo.gl/rnRdtU
------
Mayo Clinic...
On Facebook: http://Facebook.com/MayoClinic
On Twitter: http://twitter.com/MayoClinic
On Google+: http://google.com/+MayoClinic
On Instagram: http://instagram.com/MayoClinic
On Pinterest: http://Pinterest.com/MayoClinic
On YouTube: http://YouTube.com/MayoClinic
On the blogs: http://connect.MayoClinic.org
Most C-sections are done under regional anesthesia, which numbs only the lower part of your body — allowing you to remain awake during the procedure. A common choice is a spinal block, in which pain medication is injected directly into the sac surrounding your spinal cord
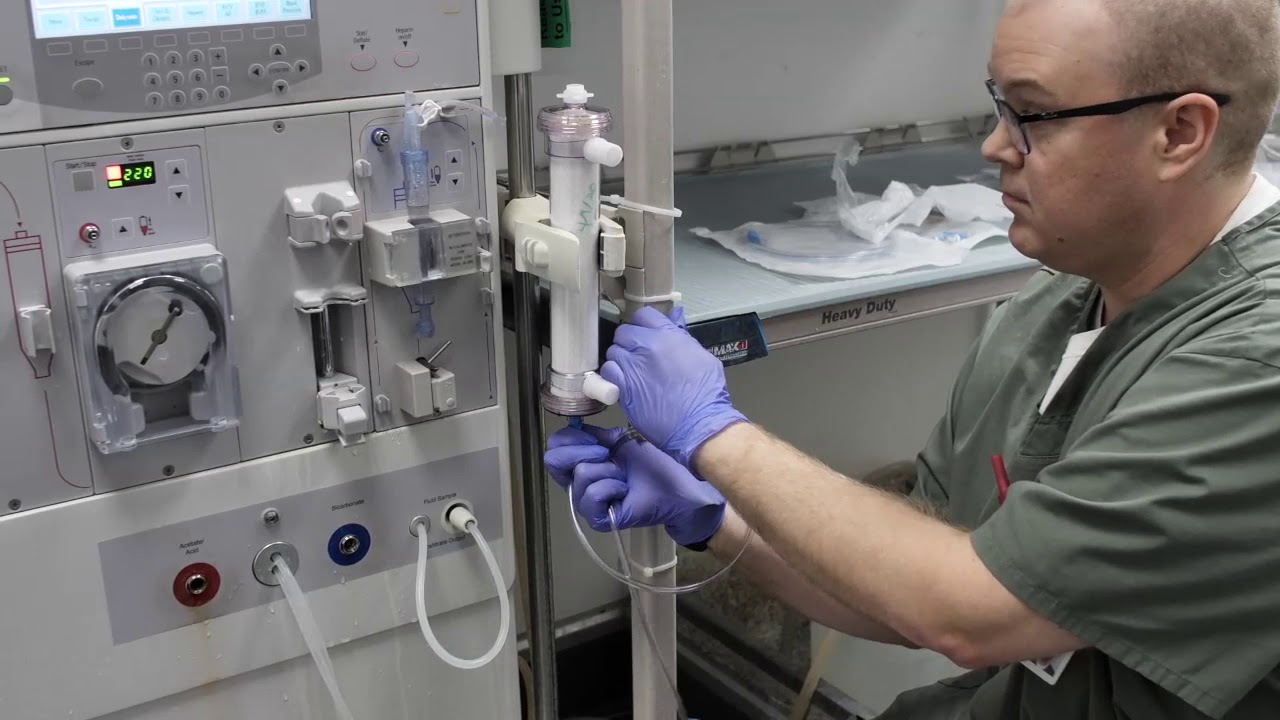
In this instructional video, Director of Critical Care Nephrology, Sevag Demirjian, MD goes over the steps for in-hospital production of ultra-pure continuous hemodialysis fluid.
By using the information in this video and/or any other materials made available by Cleveland Clinic related to the dialysate solution, you agree to comply with and be bound by the terms of the Permissive Use Agreement, a copy of which is available at https://bit.ly/3f9lN4j
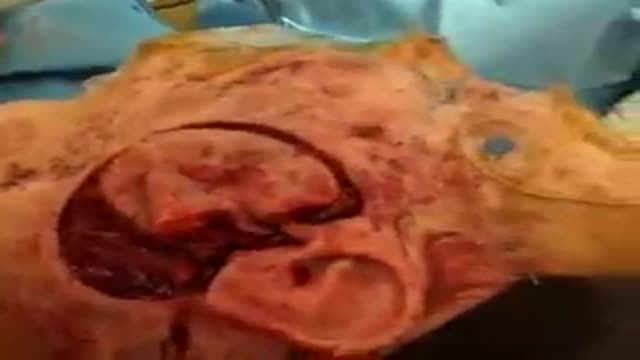
Not every woman undergoes a traditional vaginal delivery with the birth of her child. Under conditions of fetal or maternal distress, or in the case of breech presentation (when a baby is turned feet first at the time of delivery), or if the woman’s first baby was born by cesarean delivery, a procedure called a cesarean section may be required. During a cesarean, a doctor will make either a lateral incision in the skin just above the pubic hair line, or a vertical incision below the navel. As the incision is made, blood vessels are cauterized to slow bleeding. After cutting through the skin, fat, and muscle of the abdomen, the membrane that covers the internal organs is opened, exposing the bladder and uterus. At this time the physician will generally insert his or her hands into the pelvis in order to determine the position of the baby and the placenta. Next, an incision is made into the uterus and any remaining fluids are suctioned from the uterus. The doctor then enlarges the incision with his or her fingers. The baby’s head is then grasped and gently pulled with the rest of its body from the mother’s uterus. Finally, the abdominal layers are sewn together in the reverse order that they were cut. The mother is allowed to recover for approximately three to five days in the hospital. She will also be quite sore and restricted from activity for the following several weeks. There are several potential complications associated with this procedure that should be discussed with a doctor prior to surgery.

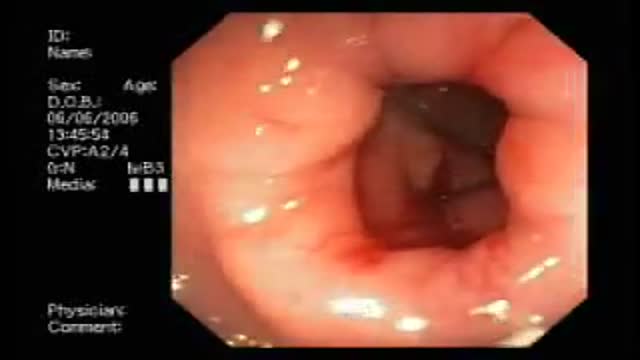
This video demonstrates Laparoscopic Cholecystectomy Fully Explained Skin-to-Skin Video with Near Infrared Cholangiography performed by Dr R K Mishra at World Laparoscopy Hospital. A laparoscopic cholecystectomy is a minimally invasive surgical procedure that involves removing the gallbladder. It is typically performed using small incisions in the abdomen, through which a laparoscope (a thin tube with a camera and light) and surgical instruments are inserted. The surgeon uses the laparoscope to visualize the inside of the abdomen and to guide the instruments in removing the gallbladder.
Near-infrared cholangiography is a technique that uses a special camera and fluorescent dye to visualize the bile ducts during surgery. The dye is injected into the cystic duct (the tube that connects the gallbladder to the bile ducts) and the camera detects the fluorescence emitted by the dye, allowing the surgeon to see the bile ducts more clearly.
The combination of laparoscopic cholecystectomy and near-infrared cholangiography has become a standard of care in many hospitals and surgical centers. It allows for a more precise and efficient surgery, reducing the risk of complications such as bile duct injury.
The use of indocyanine green (ICG) with near-infrared imaging during laparoscopic cholecystectomy has several advantages. Here are some of them:
Better visualization of the biliary anatomy: ICG with near-infrared imaging allows for better visualization of the biliary anatomy during surgery. This helps the surgeon identify important structures, such as the cystic duct and the common bile duct, and avoid injuring them.
Reduced risk of bile duct injury: With better visualization of the biliary anatomy, the risk of bile duct injury during surgery is reduced. Bile duct injury is a serious complication that can occur during laparoscopic cholecystectomy and can lead to long-term health problems.
Improved surgical precision: ICG with near-infrared imaging also improves surgical precision. The surgeon can better see the tissues and structures being operated on, which can help reduce the risk of bleeding and other complications.
Shorter operating time: The use of ICG with near-infrared imaging can shorten the operating time for laparoscopic cholecystectomy. This is because the surgeon can more quickly and accurately identify the biliary anatomy, which can help streamline the surgery.
Overall, the use of ICG with near-infrared imaging is a valuable tool in laparoscopic cholecystectomy that can improve surgical outcomes and reduce the risk of complications.
Like any surgical procedure, laparoscopic cholecystectomy (gallbladder removal) has potential complications. Here are some of the most common ones:
Bleeding: Bleeding during or after the surgery is a possible complication of laparoscopic cholecystectomy. Most cases are minor and can be easily controlled, but in rare cases, significant bleeding may require a blood transfusion or even additional surgery.
Infection: Any surgical procedure carries a risk of infection. After laparoscopic cholecystectomy, there is a risk of infection at the site of the incisions or within the abdomen. Symptoms may include fever, pain, redness, or drainage from the incision sites.
Bile leakage: In some cases, a small amount of bile may leak from the bile ducts into the abdominal cavity after gallbladder removal. This can cause abdominal pain, fever, and sometimes requires further surgery or treatment.
Injury to nearby organs: During the surgery, there is a small risk of unintentional injury to nearby organs such as the liver, intestines, or bile ducts. This can cause additional complications and may require further treatment.
Adverse reactions to anesthesia: As with any surgery requiring general anesthesia, there is a small risk of adverse reactions to the anesthesia, such as an allergic reaction, respiratory problems, or heart complications.
Most patients recover without complications following a laparoscopic cholecystectomy, but it is important to discuss any concerns or questions with your surgeon beforehand.
Contact us
World Laparoscopy Hospital
Cyber City, Gurugram, NCR Delhi
INDIA : +919811416838
World Laparoscopy Training Institute
Bld.No: 27, DHCC, Dubai
UAE : +971525857874
World Laparoscopy Training Institute
8320 Inv Dr, Tallahassee, Florida
USA : +1 321 250 7653
Regenerate response
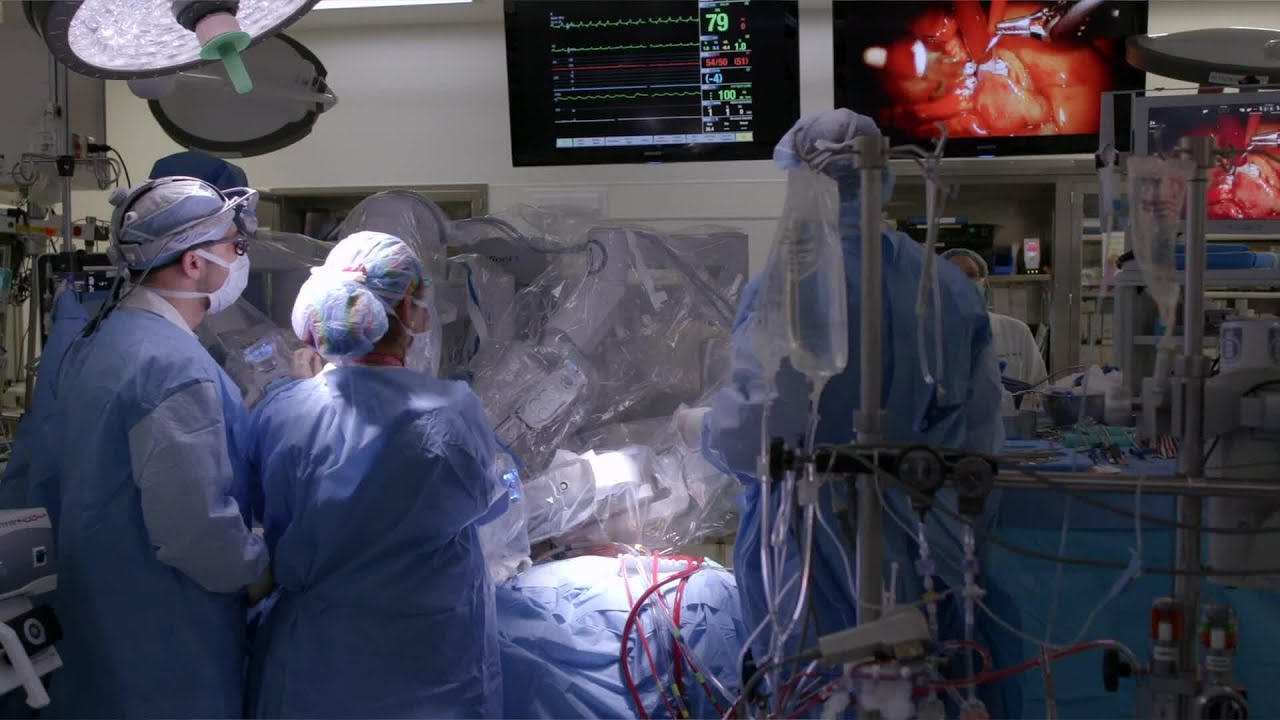
To learn more about robotically assisted heart surgery, please visit https://cle.clinic/2Y6aHXH
Robotically assisted heart surgery is a minimally invasive option most often used for mitral valve repair. Cleveland Clinic cardiothoracic surgeons explain how it works and what to expect.
To learn more about our cardiothoracic experts, please visit
Marc Gillinov, MD - https://cle.clinic/2ZtNM7b
Daniel Burns, MD - https://cle.clinic/2W1MdxI
If you liked the video hit like and subscribe for more!
#clevelandclinic #heartsurgery #roboticsurgery #heartcare #cardiothoracic

In this video, Professor Dan Reinstein performs a bilateral LASIK procedure filmed in real-time to demonstrate the full 8 and-a-half minute procedure from multiple angles. The superior design and experience of the Carl Zeiss Meditec Visumax femtosecond Laser for flap creation is seen, where the patient is only in contact with the device for about 30 seconds with extremely low contract force such that the patient feels effectively nothing, there are no red splodges (subconjunctival haemorages) left behind. From the surgeons' standpoint there is no device that is easier to use or faster for LASIK flap creation. The Carl Zeiss Meditec MEL80 excimer laser portion of the procedure is seamlessly integrated and incorporates all the features that make clinical outcomes so reproducible including the unique cone-for-controlled-atmosphere (CCA) and high efficiency, high sensitivity calibration test which can be performed for each individual patient to compensate for minor changes in energy that occur with excimer laser devices during the course of a day.
For reference to the clinical outcomes for LASIK with the MEL80 in presbyopia using PRESBYOND Laser Blended Vision see:
Reading glasses presbyopia (ageing eyes) only:
LASIK for presbyopia correction in emmetropic patients using aspheric ablation profiles and a micro-monovision protocol with the Carl Zeiss Meditec MEL 80 and VisuMax.
J Refract Surg. 2012 Aug;28(8):531-41. Reinstein DZ, Carp GI, Archer TJ, Gobbe M.
http://www.ncbi.nlm.nih.gov/pubmed/22869232
Short sighted, astigmatism and presbyopia (ageing eyes)
LASIK for Myopic Astigmatism and Presbyopia Using Non-Linear Aspheric Micro-Monovision with the Carl Zeiss Meditec MEL 80 Platform.
J Refract Surg. 2011 Jan;27(1):23-37. Epub 2010 Mar 1.
Reinstein DZ, Archer TJ, Gobbe M.
http://www.ncbi.nlm.nih.gov/pubmed/20205360
Long-sighted, astigmatism and presbyopia (ageing eyes)
LASIK for hyperopic astigmatism and presbyopia using micro-monovision with the Carl Zeiss Meditec MEL80 platform.
J Refract Surg. 2009 Jan;25(1):37-58. Reinstein DZ, Couch DG, Archer TJ.
http://www.ncbi.nlm.nih.gov/pubmed/19244952
For more information about laser eye surgery and PRESBYOND Laser Blended Vision, please contact the London Vision Clinic on 020 7224 1005.
http://www.bodysculptor.com. Dr. Otto Placik, Board Certified Chicago based plastic surgeon demonstrates the results of a muscle separation(rectus diastasis) repair using 3 dimesional CAT scan and photographic images