Top videos
A detailed description of the Hepato-pulmonary syndrome including its definition, pathophysiology, diagnosis and treatment. The pathophysiology includes nitric oxide in the pulmonary vasculature which results in intrapulmonary vasodilatation. This causes the classical and unique symptom of platypnea and orthodeoxia.

How to approach histology for Human Anatomy students. Using a key will help get you through it! Add some penguin fairy dust will help too!
Please note: I mis-spoke and said "striated" instead of "stratified epithelium" a couple of times... apologies!
There are lots of histology keys out there, but the one I showed in the video is here: http://www.penguinprof.com/upl....oads/8/4/3/1/8431323
Want more?
Subscribe: http://www.youtube.com/user/ThePenguinProf
FB Page: https://www.facebook.com/ThePenguinProf
Twitter: https://twitter.com/penguinprof
Web: http://www.penguinprof.com/
---------------------------------------------------------------------------------------------------
Details:
Tissue in the human body:
Epithelial: Is made of cells arranged in a continuous sheet with one or more layers, has apical & basal surfaces.
A basement membrane is the attachment between the basal surface of the cell & the underlying connective tissue.
Two types of epithelial tissues: (1) Covering & lining epithelia and (2) Glandular Epithelium.
The number of cell layers & the shape of the cells in the top layer can classify epithelium.
Simple Epithelium - one cell layer
Stratified epithelium - two or more cell layers
Pseudostratified Columnar Epithelium - When cells of an epithelial tissue are all anchored to the basement Membrane but not all cells reach the apical surface.
Glandular Epithelium -- (1) Endocrine: Release hormones directly into the blood stream and (2) Exocrine - Secrete into ducts.
Connective: contains many different cell types including: fibroblasts, macrophages, mast cells, and adipocytes. Connective Tissue Matrix is made of two materials: ground substance - proteins and polysaccharides, fiber -- reticular, collagen and elastic.
Classification of Connective Tissue:
Loose Connective - fibers & many cell types in gelatinous matrix, found in skin, & surrounding blood vessels, nerves, and organs.
Dense Connective - Bundles of parallel collagen fibers& fibroblasts, found in tendons& ligaments.
Cartilage - Cartilage is made of collagen & elastin fibers embedded in a matrix glycoprotein & cells called chondrocytes, which was found in small spaces.
Cartilage has three subtypes:
Hyaline cartilage -- Weakest, most abundant type, Found at end of long bones, & structures like the ear and nose,
Elastic cartilage- maintains shape, branching elastic fibers distinguish it from hyaline and
Fibrous Cartilage - Strongest type, has dense collagen & little matrix, found in pelvis, skull & vertebral discs.
Muscle: is divided into 3 categories, skeletal, cardiac and smooth.
Skeletal Muscle -- voluntary, striated, striations perpendicular to the muscle fibers and it is mainly found attached to bones.
Cardiac Muscle -- involuntary, striated, branched and has intercalated discs
Smooth Muscle -- involuntary, nonstriated, spindle shaped and is found in blood vessels & the GI tract.
Nervous: Consists of only two cell types in the central nervous system (CNS) & peripheral nervous system (PNS):
Neurons - Cells that convert stimuli into electrical impulses to the brain, and Neuroglia -- supportive cells.
Neurons -- are made up of cell body, axon and dendrites. There are 3 types of neurons:
Motor Neuron -- carry impulses from CNS to muscles and glands,
Interneuron - interpret input from sensory neurons and end responses to motor neurons
Sensory Neuron -- receive information from environment and transmit to CNS.
Neuroglia -- is made up of astrocytes, oligodendrocytes, ependymal cells and microglia in the CNS, and schwann cells and satellite cells in the PNS.
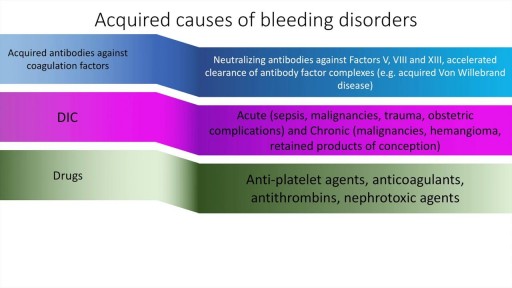
A detailed description of the approach to a use of bleeding disorders. This presentation includes the causes, history, clinical features and diagnosis of specific bleeding disorders. These include Haemophilia, DIC, Von Willebrand Disease and others. The final differentiation is often made on the basis of the Prothrombin Time, activated Partial thromboplastin time and platelet count.

Buy your new Medical Marijuana Card for $59 & renewals for $45. Chat with our licensed doctors from your place and obtain your card by email in less than 10 minutes. Visit https://www.onlinemmjlosangeles.com/
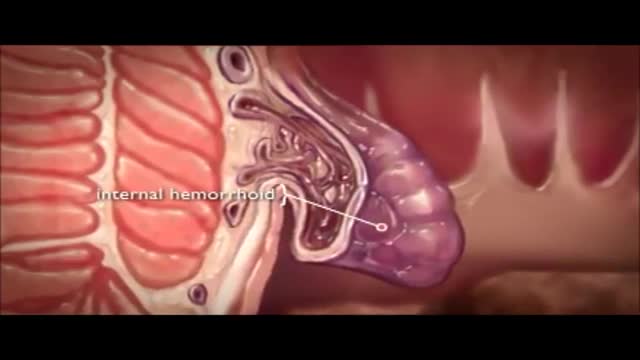
The veins around your anus tend to stretch under pressure and may bulge or swell. Swollen veins (hemorrhoids) can develop from an increase in pressure in the lower rectum. Factors that might cause increased pressure include: Straining during bowel movements.

Invasive intracranial pressure monitoring. The most common surgically placed monitors for ICP measurement are intraventricular catheters (external ventricular drain [EVD] or a ventriculostomy drain) and fiberoptic ICP monitors implanted into the parenchyma of the brain.

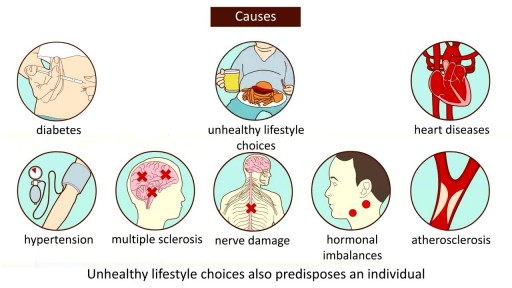
The discussion begins with a basic explanation of Bone biology taking into consideration the osteoblast and osteoclast balance. Concepts of RANK, RANK ligand and Osteoprotegerin are included. Risk factors for Osteoporosis such as Age, alcohol, smoking, sedentary lifestyle are also discussed.

The cause for TS is unknown. Early research suggested that TS is an inherited condition (often, the person's near or distant relatives have had some form of transient or chronic tic disorder or associated symptoms). Recent studies point to a combination of environmental and genetic factors as a cause of the disorder. The specific genes involved in the development of TS are still being investigated. Studies suggest that TS has a neurological basis and results from an abnormality which affects the brain's metabolism of certain neurotransmitters (chemicals in the brain that regulate behavior.) Current research being funded by the Tourette Syndrome Association (TSA) will help provide more information about the causes and genetic factors of TS.

The video is about the evolution of the anatomic UCLA laparoscopic technique over 1325 cases and demonstrates the key steps of our operation to improve patient safety and outcomes.
Learn more at http://urology.ucla.edu