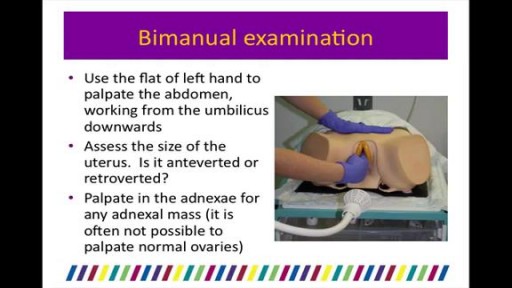
Top videos

Pain in joints or any part of body is very unpleasant and annoying experience. It is very common in people those suffering from arthritis. To get an end to all such pains, one can start using Generic Celebrex ( https://www.medexpressrx.com/celebrex-generic.aspx ). Here is a brief detail about this wonderful painkiller.

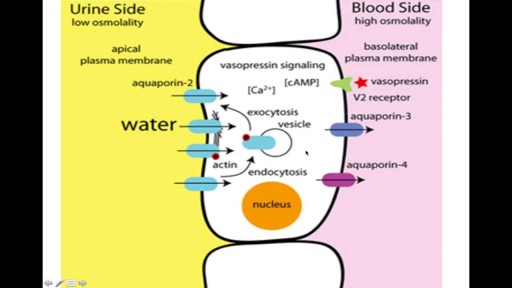
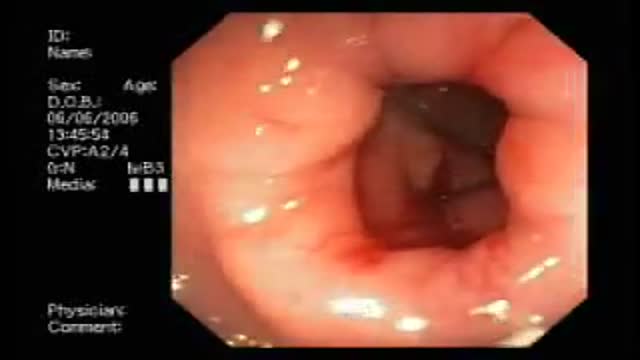
Furosemide is used to reduce extra fluid in the body (edema) caused by conditions such as heart failure, liver disease, and kidney disease. This can lessen symptoms such as shortness of breath and swelling in your arms, legs, and abdomen. This drug is also used to treat high blood pressure. Lowering high blood pressure helps prevent strokes, heart attacks, and kidney problems. Furosemide is a "water pill" (diuretic) that causes you to make more urine. This helps your body get rid of extra water and salt.
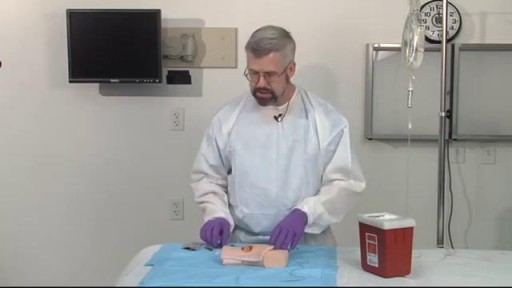
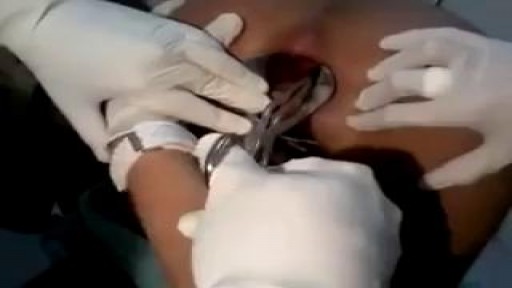
Venous cutdown is an emergency procedure in which the vein is exposed surgically and then a cannula is inserted into the vein under direct vision. It is used to get vascular access in trauma and hypovolemic shock patients when peripheral cannulation is difficult or impossible

Patient Greg Grindley communicates with host Bryant Gumbel and his wife for the first time while undergoing deep brain stimulation surgery at University Hospital's Case Medical Center in Cleveland, Ohio.
➡ Subscribe: http://bit.ly/NatGeoSubscribe
About National Geographic:
National Geographic is the world's premium destination for science, exploration, and adventure. Through their world-class scientists, photographers, journalists, and filmmakers, Nat Geo gets you closer to the stories that matter and past the edge of what's possible.
Get More National Geographic:
Official Site: http://bit.ly/NatGeoOfficialSite
Facebook: http://bit.ly/FBNatGeo
Twitter: http://bit.ly/NatGeoTwitter
Instagram: http://bit.ly/NatGeoInsta
Greg's First In-Surgery Conversation | Brain Surgery Live
https://youtu.be/zvqV_2zncNU
National Geographic
https://www.youtube.com/natgeo
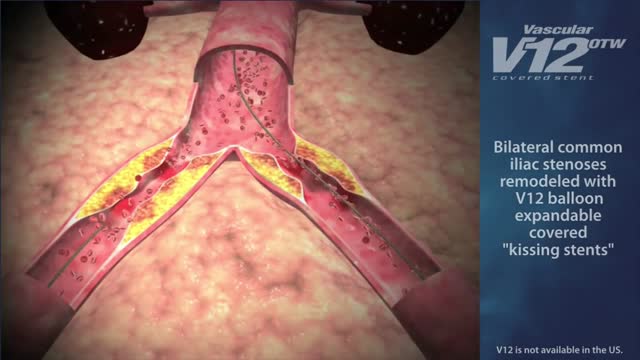
Indications for endovascular repair of the iliac artery are: Stenosis or (short-segment) occlusion of iliac artery (TASC type A and B, TASC C lesions are controversial) with ipsilateral lower extremity ischemia (lifestyle-limiting, progressive claudication, rest pain, gangrene). Patients with asymptomatic aneurysm greater than 4 cm in diameter. An iliac aneurysm which has also increased in size by 0.5 cm in last six months. Symptomatic iliac artery aneurysms mandate endovascular (or open) repair regardless of size. Patients with long occluded lesions/poor run-off/acute limb ischemia are poor endovascular candidates.
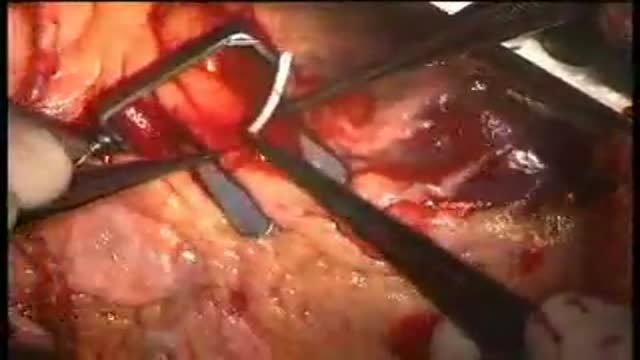
Beating heart or "off pump" coronary artery surgery is the latest revolution in the management coronary disease. It is being embraced world-wide by increasing numbers of surgeons. Many of the advantages are subtle but reduced mortality, stroke, and bleeding as well as earlier discharge are well-established benefits. A cardiac stabiliser is mandatory for this surgery, most are single use only and very expensive, this one is multiple use and is saving many healthcare dollars