Top videos

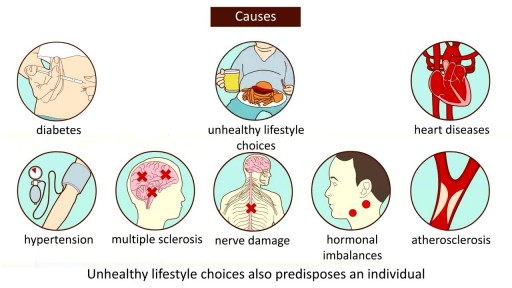
Mysterious massage from East Asia(CHINA).it can cure cure Erectile dysfunction,can let their life better.This video from mainland of China,so the language is Chinese mandarin.but you can see English show on the video too.Tiedang gong means kongfu of Iron penis&balls.

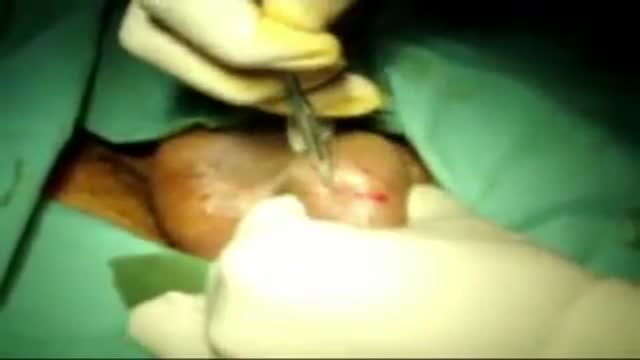
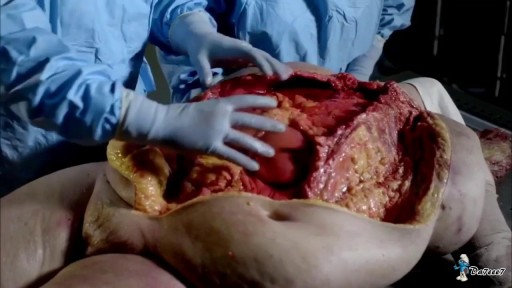
Brain port surgery is a minimally invasive surgical technique performed through a specially designed tube about the size of a dime. Using neuronavigation GPS-like guidance, the brain port is inserted into the brain with millimeter accuracy and is used as a channel to guide the surgeon and his/her instruments to various regions of the brain. Colloid cysts, metastatic tumors, and a variety of tumors within the ventricles are often candidates for this approach.

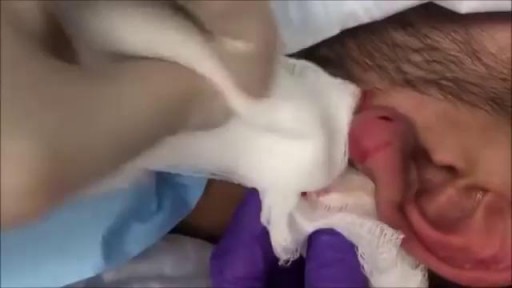
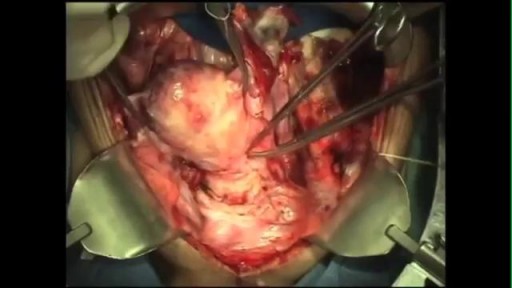
An excellent video demonstrating how a laparoscopy is performed to evaluate the uterus (note a small fibroid appearing as a bulge in the uterus), fallopian tubes and ovaries. Blue dye is injected into the uterus, entering the fallopian tubes and spilling from the end of the tubes into the abdominal cavity, confirming that both tubes are open

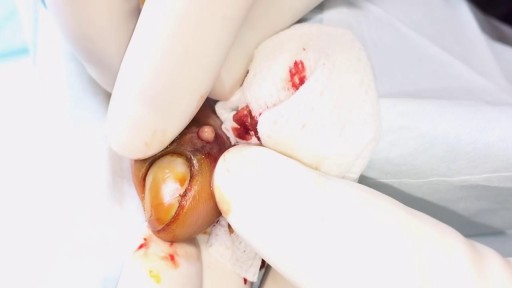
Do you think you have a hernia?
What are hernias?
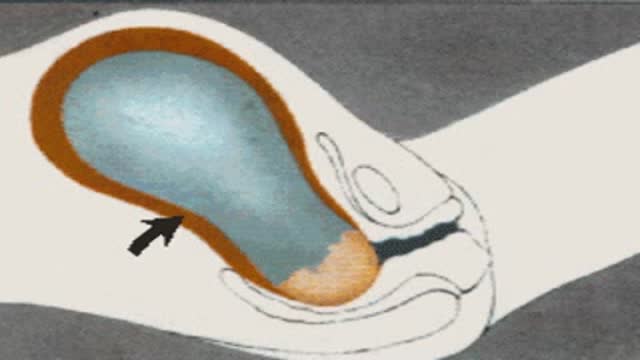
The hernias we address in this http://DoctorsExpressHartsdale.com Medical Minute are inguinal, or groin, hernias. More common in men than women, an inguinal hernia can occur when part of the small intestine protrudes through a weakness or tear in the area between your abdomen and your thigh- or your groin. It's possible for anyone to get an inguinal hernia, but it is more commonly found in males.
Hernias form a bulge and can be accompanied by pain. Men have an approximate 26% lifetime risk of having hernia at some point in their life, where as women have a much lower chance of one- only about 3% of women will experience a hernia at some point in their life. There are other types of hernias, such as abdominal, or "hiatal" hernias but groin hernias outnumber abdominal hernias by about 3 to 1.
What causes a hernia?
The cause of a hernia is not always known, but hernias are often the result of weak spots in the abdominal wall. Weaknesses can be due to congenital defects (present at birth) or formed later in life. Some risk factors for inguinal hernia include:
• fluid or pressure in the abdomen
• heavy lifting
• straining during urination or bowel movements
• obesity
• chronic cough
• pregnancy
Hernias often form in people with weakened abdominal muscles or in those who do a lot of heavy lifting or straining, which is why we see it quite often in young men. Physiology plays a part: men have testicles and scrotum which descend through the inguinal canal-much larger in men than in women. That is part of the reason men tend to be more susceptible to hernias than women.
Symptoms of hernia
Symptoms of inguinal hernia usually include a bulge in the groin area and pain, pressure, or aching at the bulge—especially when lifting, bending, or coughing. These symptoms usually subside during rest periods. Men may also experience swelling around the testicles.
Screening and Diagnosis of Hernias
If you are having abdominal pain or pelvic bulge and pain, you want to see physician, and he or she will do an exam. They will use their finger, to see if you have a bulge in your scrotum or on your groin and they'll see if its reducible or not. If the exam doesn't give them the answer, they can then perform an ultrasound, an inexpensive test that can tell you the same day whether a hernia is present.
What to do if you think you have a hernia
Most of the time hernias do not cause problems. People often live with hernias their entire life without them becoming aggravated or painful. When they do cause pain though, there is concern that complications may have arisen. Most common hernias are what we call reducible; you can take your finger or you can lie down in bed and due to the effects of gravity, the bulge in the groin will actually disappear, which means the intestinal contents actually go back into the abdominal cavity or to the correct location. If it's not reducible by lying down or using a finger or having a physician trying to reduce it, then there are concerns about complications such as strangulation, or incarceration occurring. If those concerns are there, then you need to see a surgeon, and there may be a need for surgery.
How to Treat a Hernia
As stated earlier, hernias can often be watched for years without being treated. If however, they are causing pain, we generally refer you to a surgeon who can do a very simple laparoscopic surgery.
If you suspect a hernia, but have not been diagnosed, you should see your doctor, and of course, we are happy to see you here at Doctors Express

In order to be able to look at tissues under a microscope, we need to first stain them with the right technique. Learn the main staining techniques used in histology today on our full video: https://khub.me/aux9w
Oh, are you struggling with learning anatomy? We created the ★ Ultimate Anatomy Study Guide ★ to help you kick some gluteus maximus in any topic. Completely free. Download yours today: https://khub.me/e0th1
As you probably know, histology is the study of the microscopic anatomy of cells and tissues. So we use staining methods to visualize and distinguish the different parts of cells and tissues since cells and their structures are usually transparent or colorless. The types of dyes used to color cells and their components can either be specific to particular structures, chemical groups or even molecules, and it can also be non-specific in which case most of the cell is stained in the same way.
When staining tissue samples, dyes that are used are either acidic or basic or a combination of the two. And why is that, you might be asking. Well, cellular structures such as nucleic acids or proteins have charged groups which are known as phosphate groups or carboxyl groups, just to name a couple. The dyes used in histology are colored organic compounds which also have a charge. Acidic dyes carry a negative charge and so they bind to positively-charged cell structures.
In the full version of this tutorial, we will cover some of the most common types of dyes used in histological staining of cells and their structures:
- basic dyes vs acidic dyes vs neutral dyes;
- hematoxylin and eosin;
- PAS - staining;
- Golgi method;
- Toluidine blue;
- Masson's trichrome;
- Osmium tetroxide;
To master this topic, click on the link and carry on watching the full video (available to Premium members): https://khub.me/aux9w !
Want to test your knowledge on the different types of cells and tissues? Take this quiz: https://khub.me/3g19f
Read more on how to interpret different histological sections on this complete article which goes through the different stains used in histology https://khub.me/saimh
For more engaging video tutorials, interactive quizzes, articles and an atlas of Human anatomy and histology, go to https://khub.me/pkvz2
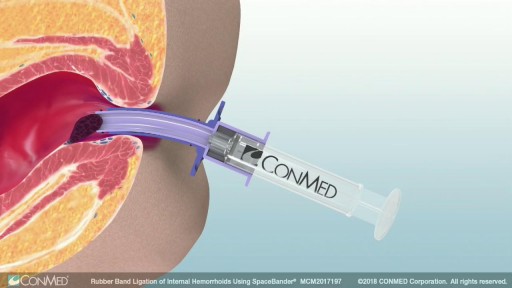
Rubber band ligation is a procedure in which the hemorrhoid is tied off at its base with rubber bands, cutting off the blood flow to the hemorrhoid. This treatment is only for internal hemorrhoids. To do this procedure, a doctor inserts a viewing instrument (anoscope) into the anus. The hemorrhoid is grasped with an instrument, and a device places a rubber band around the base of the hemorrhoid. The hemorrhoid then shrinks and dies and, in about a week, falls off. A scar will form in place of the hemorrhoid, holding nearby veins so they don't bulge into the anal canal. The procedure is done in a doctor's office. You will be asked whether the rubber bands feel too tight. If the bands are extremely painful, a medicine may be injected into the banded hemorrhoids to numb them. After the procedure, you may feel pain and have a sensation of fullness in the lower abdomen. Or you may feel as if you need to have a bowel movement. Treatment is limited to 1 to 2 hemorrhoids at a time if done in the doctor's office. Several hemorrhoids may be treated at one time if the person has general anesthesia. Additional areas may be treated at 4- to 6-week intervals.
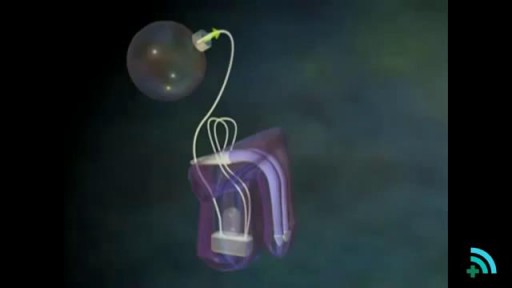
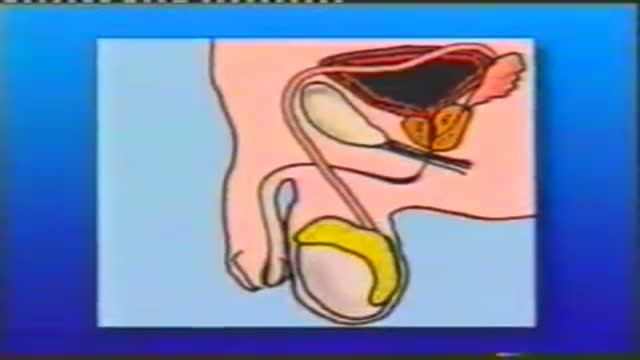
he inflatable penile prosthesis consists of two attached cylinders -- a reservoir and a pump -- which are placed surgically in the body. The two cylinders are inserted in the penis and connected by tubing to a separate reservoir of saline. The reservoir is implanted under the rectus muscles in the lower abdomen.
Throughout the body, there are several points at which blood vessels unite. The junctions are termed anastomoses. In the simplest sense, an anastomosis is any connection (made surgically or occurring naturally) between tube-like structures. Naturally occurring arterial anastomoses provide an alternative blood supply to target areas in cases where the primary arterial pathway is obstructed. They are most abundant in regions of the body where the blood supply may can be easily damaged or blocked (such as the joints or intestines). This article focuses on the arterial anastomotic networks of the upper limb.