Top videoer

Anxiety Disorder, How To Calm Anxiety, Beck Anxiety Inventory, Best Anxiety Medication ---- http://panic-attacks-anxiety.good-info.co --- They’re calling it the “Anxiety Destroyer Technique” Check it out... Last week I told you I stumbled upon a video presentation that teaches a simple trick to stop your next panic attack... and relieve high anxiety levels… in 60 seconds or less... Well, it seems the folks who have tried this technique already are amazed by it. In fact, some are so blown away by how much relief they’re enjoying that they’re now calling this little trick... the “Anxiety Destroyer Technique”. So guess what? I did some research. Turns out its not some Hocus-Pocus solution. It’s actually based on a revolutionary new clinically proven form of therapy, called Neuro Activation Therapy! This technique is unlike anything I’ve seen or heard about before. It has nothing to do with drugs breathing exercises, or anything you’ll read about in a book or website online. Best part: It’s not just a solution for panic attacks and anxiety. The same technique works on fears phobias, overwhelming levels or stress and worry, obsessive-compulsive disorder, social anxiety – even depression! I highly recommend you this technique. If you suffer from these issues, it really can help you. Click Here: http://panic-attacks-anxiety.good-info.co
Overview HIV is a virus that affects the immune system, specifically the CD4 cells. The CD4 cells help protect the body from illness. Unlike other viruses that the immune system can fight off, HIV can’t be eliminated by the immune system. The symptoms of HIV can vary greatly from person to person. No two people with HIV will likely experience the exact same symptoms. However, HIV will generally follow this pattern: acute illness asymptomatic period advanced infection Acute illness Approximately 80 percent of people who contract HIV experience flu-like symptoms within two to four weeks. This flu-like illness is known as acute HIV infection. Acute HIV infection is the primary stage of HIV and lasts until the body has created antibodies against the virus. The most common symptoms of this stage of HIV include: body rash fever sore throat severe headaches Less common symptoms may include: fatigue swollen lymph nodes ulcers in the mouth or on the genitals muscle aches joint pain nausea and vomiting night sweats Symptoms typically last one to two weeks. Anyone who has these symptoms and thinks they may have contracted HIV should consider scheduling an appointment with their healthcare provider to get tested. Symptoms specific to men Symptoms of HIV are generally the same in women and men. One HIV symptom that is unique to men is an ulcer on the penis. HIV may lead to hypogonadism, or poor production of sex hormones, in either sex. However, hypogonadism’s effects on men are easier to observe than its effects on women. Symptoms of low testosterone, one aspect of hypogonadism, can include erectile dysfunction (ED).

Surgery to treat men with prostate cancer is often followed by months of difficulty controlling urine flow, a condition known as urinary incontinence. But new research suggests that this problem may go away more quickly if the men perform certain exercises to strengthen their pelvic floor muscles.
Researchers from the Kaiser Permanente Medical Center in Los Angeles, California, found that men who were taught how to perform pelvic floor exercises before and after surgery were more likely to have regained continence three months later.
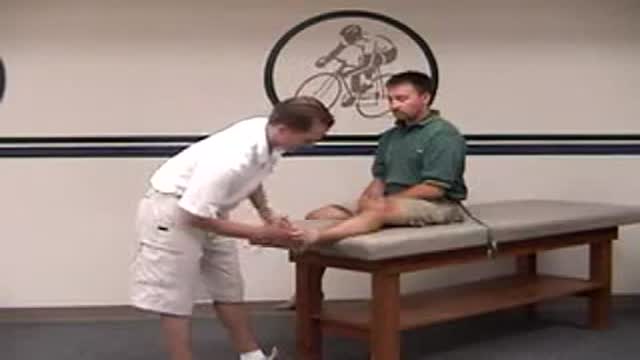
Men Doing Pelvic Exercises Recover Earlier
In the current study, the researchers randomly assigned 38 men scheduled for radical prostatectomy to either a treatment group or a control group. The men in the treatment group were referred to a physical therapist. They were instructed how to do Pelvic Floor Exercises both before and after surgery, using biofeedback to ensure they were using the proper muscles. The control group did not receive any formal instruction. All of the men completed questionnaires regarding bladder function at regular intervals over the next year.
Overall, 82% of the patients had regained continence (defined as not needing to use any absorbent pads) by the end of the year, including about equal numbers in both groups. But on average the men who had been educated about Pelvic exercises regained continence about one month earlier than those in the control group (at 12 weeks vs. 16 weeks).
Most of the men who did not regain continence within a year were still using at least three absorbent pads a day, indicating continued severe incontinence. The study authors explained that these men probably had extensive damage to the bladder sphincter or severe dysfunction of the bladder after surgery, and the exercises alone were unable to compensate for this.
But the exercises seemed to be effective. Pelvic floor exercise and education initiated prior to surgery is an effective noninvasive intervention useful for improving early return of urinary continence, the authors concluded. It would certainly have a positive impact on our patients undergoing radical prostatectomy in an effort to improve quality of life after major urological surgery.
The results of the study were published in the Journal of Urology (Vol. 170, No. 1: 130-133)

Vial medication administration nursing skill. Learn techniques to withdraw medication from a vial using a syringe with a needle.
Medications can come in different forms, such as ampules, vials, tablets, capsules, and so forth. When withdrawing medication from a vial, there are a few things you'll want to know as a nursing student or nurse.
First, there are different needles that can be attached to the syringe. You can use a traditional needle with a beveled tip; you can use a blunt-tip needle to reduce the risk of needle sticks; or you can use a filter needle, which is sometimes required or recommended when drawing medication from a vial, particularly in cases of reconstituted medication.
When withdrawing from a vial, you'll want to do these things (assuming they fit with the protocols and manufacturer's instructions):
NOTE: Some medications or vaccines may require a different technique, so always consult with the manufacturer's instructions.
-gather your supplies
-perform hand hygiene
-clean the vial's top with alcohol prep
-attach the appropriate needle
-stick the needle using a technique to prevent coring of the rubber on the vial (start with 45 degree angle, and as you puncture the vial, rotate the needle to a 90 degree angle in one smooth motion).
-push air into the vial equal to the amount of medication you plan to draw
-invert the vial to withdraw medication
-remove air bubbles
-and much more
See more Nursing Skills: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Notes: https://www.registerednursern.....com/how-to-withdraw-
Website: https://www.registerednursern.com/
More Videos: https://www.youtube.com/watch?v=R2XMro13dD0&list=UUPyMN8DzkFl2__xnTEiGZ1w
Nursing Gear: https://teespring.com/stores/registerednursern
Instagram: https://www.instagram.com/registerednursern_com/
Facebook: https://www.facebook.com/RegisteredNurseRNs
Twitter: https://twitter.com/NursesRN
Popular Playlists:
NCLEX Reviews: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Fluid & Electrolytes: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf

This is part 2 Herbal Medicine. Lecture presented to the International Congress of Pediatric Hepatology Sharm 2009. It is one of a series of lectures discussing the Alternative medicine practices with critical appraisal and measure the evidence.

http://yoursnoringcures.plus101.com
--Your Snoring Cures...How to Cure Snoring Naturally without Using Any Medication or Ridiculous Device!
How to Cure Snoring Naturally and Easily without Undertaking any Dangerous Surgery, Nor using any Medication or Ridiculous Device ! Doctors and Pharmaceutical Companies have tried to have my guide BANNED ...

Liposuction is a surgical procedure that is done to remove fat deposits from underneath the skin. Common areas that are treated: the abdomen, buttocks, thighs, upper arms, chest and neck. (use medical graphic of body with labeled parts) The procedure is usually done as an outpatient under some combination of local anesthesia and/or sedation:. This means you are awake but relaxed and pain free. Depending on the number of areas to be treated and the specific technique selected, it may take from one to several hours. A small incision (cut) is made through the skin near the area of the fat deposit. Multiple incisions may be needed if a wide area or multiple areas are being done. A long hollow tube called a cannula will be inserted through this incision. Prior to inserting the cannula, the doctor may inject a solution of salt water that contains an anesthetic (numbing) medication and another medication to decrease bleeding. The cannula is then inserted and moved under the skin in a way to loosen the fat deposits so they may be suctioned out. Because a significant amount of body fluid is removed with the fat, an intravenous (through the veins) fluid line will be kept going during the procedure.
A recent technique called “ultrasound-assisted lipoplasty” uses a special cannula that liquefies the fat cells with ultrasonic energy. You should ask your doctor which technique he/she will use and how it will affect the type of anesthesia you will need and the length of the procedure.
Why is this procedure performed?
Liposuction is done to restore a more normal contour to the body. The procedure is sometimes described as body sculpting. It should be limited to fat deposits that are not responsive to diet and exercise. It is suggested that you should be within 20of your ideal body weight at the time of surgery. If you are planning to lose weight you should delay this procedure. This is not obesity surgery. The maximum amount of fat that can be removed is usually less than 10 pounds. The best results are achieved in people who still have firm and elastic skin. Although rare, there are risks and complications that can occur with liposuction. You should be aware that all the complications are increased if you are a smoker. You will need to quit smoking or at least avoid smoking for a month before and after surgery. If you have had prior surgeries near any of the areas to be treated, this may increase the risk of complications and you should discuss this with your doctor. Any history of heart disease, diabetes, bleeding problems or blood clots in your legs may make you more prone to post-operative problems and you should discuss these with your doctor. Finally, as with any cosmetic procedure it is important to have realistic expectations. The goals, limitations, and expectations of the procedure should be discussed openly and in detail with your doctor. Most insurance companies do not cover cosmetic surgery.
What should I expect during the post-operative period?
After surgery you should be able to go home but you will need someone to drive you. In the first few days after surgery it is common for the incisions to drain fluid and you will have to change dressings frequently. Fresh blood is not usual and if you have any bleeding you should call your doctor immediately. In some cases a small tube may have been placed through the skin to allow drainage. You will be limited to sponge baths until the drains and dressings are removed. After that you may take showers but no baths for 2 weeks. You may experience pain, burning, and numbness for a few days. Take pain medicine as prescribed by your doctor. You may notice a certain amount of bruising and swelling. The bruising will disappear gradually over 1 to 2 weeks. Some swelling may last for up to 6 months. If you have skin sutures they will be removed in 7 to 10 days. You should be able to be up and moving around the house the day after surgery but avoid any strenuous activity for about 1

Leopold's Maneuvers are difficult to perform on obese women and women who have hydramnios. The palpation can sometimes be uncomfortable for the woman if care is not taken to ensure she is relaxed and adequately positioned. To aid in this, the health care provider should first ensure that the woman has recently emptied her bladder. If she has not, she may need to have a straight urinary catheter inserted to empy it if she is unable to micturate herself. The woman should lie on her back with her shoulders raised slightly on a pillow and her knees drawn up a little. Her abdomen should be uncovered, and most women appreciate it if the individual performing the maneuver warms their hands prior to palpation. First maneuver: Fundal Grip While facing the woman, palpate the woman's upper abdomen with both hands. A professional can often determine the size, consistency, shape, and mobility of the form that is felt. The fetal head is hard, firm, round, and moves independently of the trunk while the buttocks feel softer, are symmetric, and the shoulders and limbs have small bony processes; unlike the head, they move with the trunk. Second maneuver After the upper abdomen has been palpated and the form that is found is identified, the individual performing the maneuver attempts to determine the location of the fetal back. Still facing the woman, the health care provider palpates the abdomen with gentle but also deep pressure using the palm of the hands. First the right hand remains steady on one side of the abdomen while the left hand explores the right side of the woman's uterus. This is then repeated using the opposite side and hands. The fetal back will feel firm and smooth while fetal extremities (arms, legs, etc.) should feel like small irregularities and protrusions. The fetal back, once determined, should connect with the form found in the upper abdomen and also a mass in the maternal inlet, lower abdomen. Third maneuver: Pawlick's Grip In the third maneuver the health care provider attempts to determine what fetal part is lying above the inlet, or lower abdomen.[2] The individual performing the maneuver first grasps the lower portion of the abdomen just above the symphysis pubis with the thumb and fingers of the right hand. This maneuver should yield the opposite information and validate the findings of the first maneuver. If the woman enters labor, this is the part which will most likely come first in a vaginal birth. If it is the head and is not actively engaged in the birthing process, it may be gently pushed back and forth. The Pawlick's Grip, although still used by some obstetricians, is not recommended as it is more uncomfortable for the woman. Instead, a two-handed approach is favored by placing the fingers of both hands laterally on either side of the presenting part. Fourth maneuver The last maneuver requires that the health care provider face the woman's feet, as he or she will attempt to locate the fetus' brow. The fingers of both hands are moved gently down the sides of the uterus toward the pubis. The side where there is resistance to the descent of the fingers toward the pubis is greatest is where the brow is located. If the head of the fetus is well-flexed, it should be on the opposite side from the fetal back. If the fetal head is extended though, the occiput is instead felt and is located on the same side as the back. Cautions Leopold's maneuvers are intended to be performed by health care professionals, as they have received the training and instruction in how to perform them. That said, as long as care taken not to roughly or excessively disturb the fetus, there is no real reason it cannot be performed at home as an informational exercise. It is important to note that all findings are not truly diagnostic, and as such ultrasound is required to conclusively determine the fetal position.

The oral contraceptive pill, commonly known as "the pill," is a hormone-based method of preventing pregnancy. It can also help resolve irregular menstruation, painful or heavy periods, endometriosis, acne, and premenstrual syndrome (PMS). Birth control pills work by preventing ovulation. No egg is produced, so there is nothing for the sperm to fertilize. Pregnancy cannot occur. "The pill" is used by nearly 16 percent of women aged 15 to 44 years in the United States, and it has both advantages and disadvantages. People with different risk factors may be advised to use a particular kind of pill. There are different types of contraceptive pills. They all contain synthetic forms of the hormones estrogen, progesterone, or both. Synthetic progesterone is called progestin. Combination pills contain progestin and estrogen. The "mini pill," contains only progestin. Monophasic pills all contain the same balance of hormones. With phasic pills, two or three different types of pill are taken each month, each with a different balance of hormones.
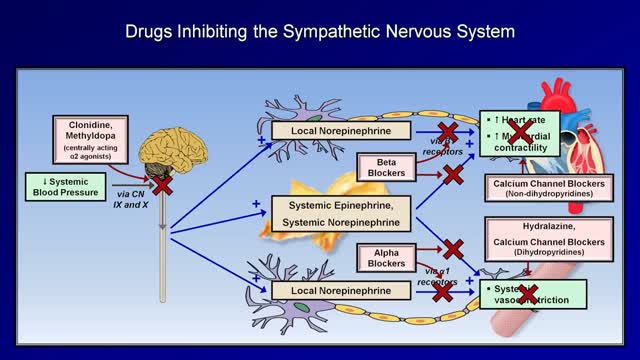
Medications to treat high blood pressure Thiazide diuretics. ... Beta blockers. ... Angiotensin-converting enzyme (ACE) inhibitors. ... Angiotensin II receptor blockers (ARBs). ... Calcium channel blockers. ... Renin inhibitors
This video is available for instant download licensing here: https://www.alilamedicalmedia.....com/-/galleries/all-
©Alila Medical Media. All rights reserved.
Support us on Patreon and get FREE downloads and other great rewards: patreon.com/AlilaMedicalMedia
All images/videos by Alila Medical Media are for information purposes ONLY and are NOT intended to replace professional medical advice, diagnosis or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding a medical condition.
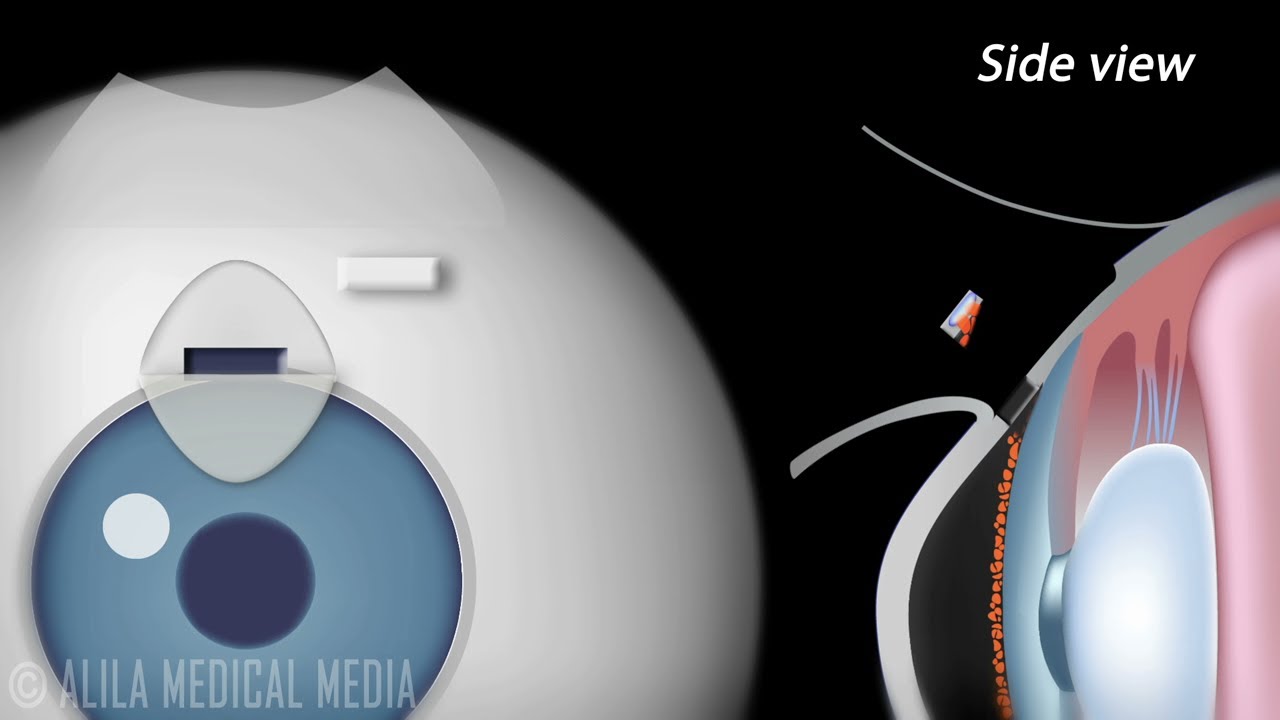
Trabeculectomy, also called Filtration Surgery, is a surgical procedure performed for treatment of glaucoma. The treatment involves removing part of the trabecular meshwork and creating a new escape route for the aqueous humor. When successful, it allows the aqueous fluid to drain from the eye into an area underneath the conjunctiva where it is subsequently absorbed by the body's circulatory system or filtered into tears.
In this procedure:
- A conjunctival pocket is created and maybe treated with Mitomycin or other antimetabolites for a few minutes. These drugs are used to prevent scarring of the operation site. Scarring, if occurs, may clog the new drainage canal, and is therefore the major reason the procedure may fail.
- A half thickness flap is then made in the sclera and is dissected all the way to the clear cornea.
- A block of scleral tissue including part of the trabecular meshwork and Schlemm's canal is then removed to make a hole into the anterior chamber of the eye.
- As the iris may plug up this hole from the inside, a piece of the iris maybe removed at this time. This is called iridectomy.
- The scleral flap is then sutured loosely back in place. These sutures can be released gradually during a couple of weeks after surgery. This allows adjustment of the aqueous flow in order to achieve target pressure and to avoid the complication of having a too low intraocular pressure.
- The conjunctiva is sewn back in place to cover the area.
After surgery, aqueous humor drains into a filtering area called a "bleb" under the conjunctiva. Since the surgery is usually performed near the top of the eye, the bleb can easily be concealed behind the upper eyelid.

TUMMY TUCK 🤩 Immediate OR Results
This patient wanted to get her abs back, but unfortunately NO diet or workout can tighten muscles that have been stretched apart from carrying a baby 👀 But we can fix that at Lemmon Avenue Plastic Surgery & Laser Center!
To learn more about the #tummytuck click here: https://drdeuber.com/procedures/tummy-tuck/
For #mommymakeover, click here: https://drdeuber.com/procedures/mommy-makeover/
👙
#MarkDeuberMD

Will you still love me if I have herpes? About 1 in 6 Americans between the ages of 14 and 49 is infected with herpes simplex virus type 2, according to a health survey released by the Centers for Disease Control and Prevention. If you’re living with herpes, HSV, HPV or other STDs, you're recommended to check out the largest STD support site STDdatings.

Antisocial personality disorder (ASPD) is defined by the American Psychiatric Association's Axis II (personality disorders) of the Diagnostic and Statistical Manual (DSM-IV-TR) as "a pervasive pattern of disregard for, and violation of, the rights of others that begins in childhood or early adolescence and continues into adulthood." Antisocial personality disorder is sometimes wrongly referred to as psychopathy or sociopathy. Currently, neither psychopathy nor sociopathy are valid diagnoses described in the Diagnostic and Statistical Manual of Mental Disorders, and the ICD-10 of the World Health Organization also lacks psychopathy as a diagnostic disorder. Psychopathy is normally seen as a subset of the antisocial personality disorder, but Blair believes that the antisocial personality disorder and psychopathy may be separate conditions altogether.