Los mejores videos

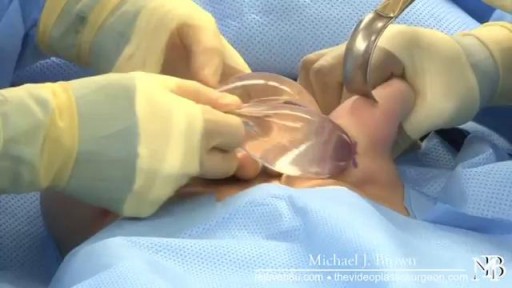
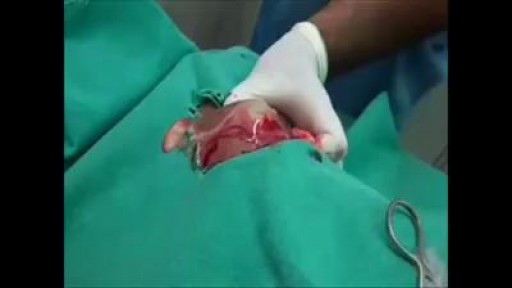
Breast reconstruction 3D Animation
on Friday, December 17, 2010
The primary part of the procedure can often be carried out immediately following the mastectomy. As with many other surgeries, patients with significant medical comorbidities (high blood pressure, obesity, diabetes) and smokers are higher-risk candidates. Surgeons may choose to perform delayed reconstruction to decrease this risk. Patients expected to receive external beam radiation as part of their adjuvant treatment are also commonly considered for delayed autologous reconstruction due to significantly higher complication rates with tissue expander-implant techniques in those patients. Breast reconstruction is a large undertaking that usually takes multiple operations. Sometimes these follow-up surgeries are spread out over weeks or months. If an implant is used, the individual runs the same risks and complications as those who use them for breast augmentation but has higher rates of capsular contracture (tightening or hardening of the scar tissue around the implant) and revisional surgeries. Outcomes based research on quality of life improvements and psychosocial benefits associated with breast reconstruction served as the stimulus in the United States for the 1998 Women's Health and Cancer Rights Act which mandated health care payer coverage for breast and nipple reconstruction, contralateral procedures to achieve symmetry, and treatment for the sequelae of mastectomy. This was followed in 2001 by additional legislation imposing penalties on noncompliant insurers. Similar provisions for coverage exist in most countries worldwide through national health care programs. There are many methods for breast reconstruction. The two most common are: * Tissue Expander - Breast implants This is the most common technique used in worldwide. The surgeon inserts a tissue expander, a temporary silastic implant, beneath a pocket under the pectoralis major muscle of the chest wall. The pectoral muscles may be released along its inferior edge to allow a larger, more supple pocket for the expander at the expense of thinner lower pole soft tissue coverage. The use of acellular human or animal dermal grafts have been described as an onlay patch to increase coverage of the implant when the pectoral muscle is released, which purports to improve both functional and aesthtic outcomes of implant-expander breast reconstruction. o In a process that can take weeks or months, saline solution is percutaneously injected to progressively expand the overlaying tissue. Once the expander has reached an acceptable size, it may be removed and replaced with a more permanent implant. Reconstruction of the areola and nipple are usually performed in a separate operation after the skin has stretched to its final size. * Flap reconstruction The second most common procedure uses tissue from other parts of the patient's body, such as the back, buttocks, thigh or abdomen. This procedure may be performed by leaving the donor tissue connected to the original site to retain its blood supply (the vessels are tunnelled beneath the skin surface to the new site) or it may be cut off and new blood supply may be connected. o The latissimus dorsi muscle flap is the donor tissue available on the back. It is a large flat muscle which can be employed without significant loss of function. It can be moved into the breast defect still attached to its blood supply under the arm pit (axilla). A latissimus flap is usually used to recruit soft-tissue coverage over an underlying implant. Enough volume can be recruited occasionally to reconstruct small breasts without an implant. o Abdominal flaps The abdominal flap for breast reconstruction is the TRAM flap or its technically distinct variants of microvascular "perforator flaps" like the DIEP/SIEP flaps. Both use the abdominal tissue between the umbilicus and the
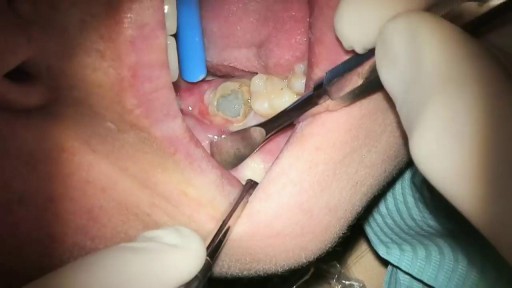
What Is It? Your wisdom teeth (third molars) usually start to erupt (enter your mouth) during the late teen years. Sometimes, there's not enough room for them. They may come into your mouth partially or not at all. Partial eruption of a wisdom tooth can create a flap of gum tissue next to the tooth. The flap can trap bits of food and debris. It can turn into a hotbed for bacteria. It's called pericoronitis if the tissue around the tooth becomes inflamed. Pericoronitis also can occur around a wisdom tooth that is still completely under the gums. Symptoms Symptoms include: Painful, swollen gum tissue in the area of the affected tooth. It can be difficult to bite down comfortably without catching the swollen tissue between your teeth. A bad smell or taste in the mouth Discharge of pus from the gum near the tooth More serious symptoms include: Swollen lymph nodes under your chin (the submandibular nodes) Muscle spasms in the jaw Swelling on the affected side of the face Diagnosis Usually, someone with pericoronitis goes to the dentist, complaining of pain in the area of the back tooth. Pericoronitis is diagnosed during the clinical exam. Your dentist will see inflamed gum tissue in the area of the unerupted or partly erupted wisdom tooth. The gums may be red, swollen or draining fluid or pus. Expected Duration Pericoronitis can be managed with antibiotics and warm salt water rinses. It goes away in about one week. However, it can return. This is likely to happen if the tooth does not completely enter the mouth and food and bacteria keep building up under the gum. Prevention You can help to prevent pericoronitis by brushing any erupting wisdom tooth and flossing around it. This will help make sure that food and bacteria do not build up under the gums. However, sometimes these steps do not work. If pericoronitis returns, you may need to have the flap of gum tissue removed. In some cases, the flap of tissue grows back and the wisdom tooth will need to be extracted. Treatment Pericoronitis can be tricky to treat. That's because the flap of gum tissue won't go away until the wisdom tooth emerges naturally, the tissue is removed or the tooth is removed. Your dentist will clean the area thoroughly by rinsing under the flap with water to remove bits of food and pus. Your dentist also may need to remove damaged tissue. If the area is infected, you'll most likely be given antibiotics. Your dentist will explain how to keep the area clean, which is the best way to prevent the problem from returning. This usually involves brushing and flossing daily and rinsing your mouth with water several times a day. These steps will help to prevent food from getting stuck under the gum flap. In some cases, your dentist may suggest removing the erupting tooth. Or the dentist may want to remove the tooth above it, which bites down on the gum below. If your dentist thinks the tooth may erupt fully into the mouth without problems, he or she may leave it alone. However, if pericoronitis comes back, the tooth may be extracted. Pericoronitis that causes symptoms should be treated as soon as possible. If it is not, the infection can spread to other areas of your mouth. The most severe cases are treated in a hospital. They sometimes require intravenous antibiotics and surgery. When To Call a Professional If you have symptoms of pericoronitis, make an appointment to see your dentist. If your wisdom teeth are coming in, visit your dentist at least twice a year for regular checkups. During those visits, the dentist can check on the progress of your wisdom teeth. Prognosis Pericoronitis does not cause any long-term effects. If the affected tooth is removed or erupts fully into the mouth, the condition cannot return.
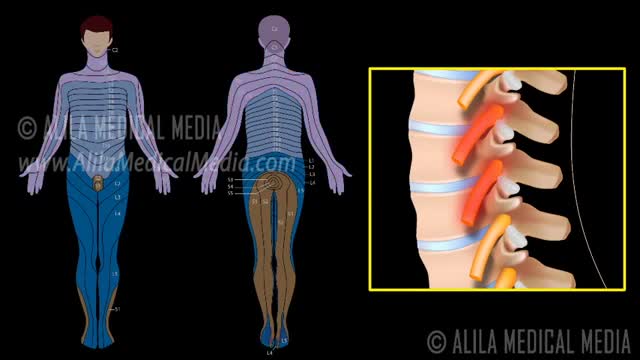
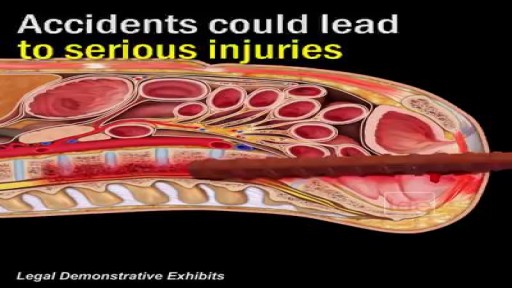
A nerve root block is an injection of local anesthetic (numbing medicine) and steroid injected under X-ray guidance into the area where the nerve exits the spinal column. A nerve root block is usually ordered by your doctor for pain in the arm or leg that follows the path of a single nerve. A nerve root block may be diagnostic (a test to determine the source of your pain) and/or therapeutic (to relieve your pain). If you get a period of sustained pain relief from the injection, the block may be repeated. Sometimes the block is done to help identify whether or not surgery might be helpful and at what level such surgery might be most helpful.
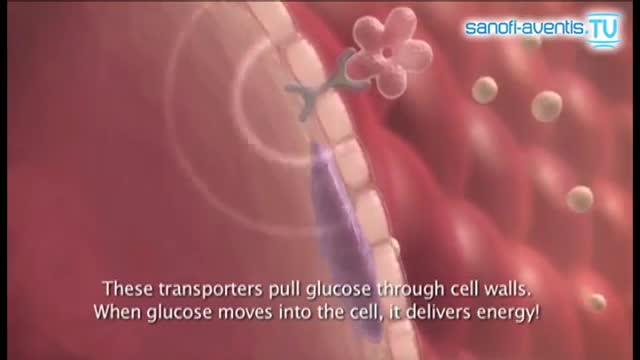
This hormone, insulin, causes the liver to convert more glucose into glycogen (this process is called glycogenesis), and to force about 2/3 of body cells (primarily muscle and fat tissue cells) to take up glucose from the blood through the GLUT4 transporter, thus decreasing blood sugar.

Dr. David Sneed of Aesthetica Med Spa in Austin discusses the latest liposuction technique known as Body Jet Water Liposuction - which is quickly gaining popularity due to the procedure being less invasive than traditional liposuction techniques, therefore minimizing recovery time and pain.

Strep throat is a bacterial infection that can make your throat feel sore and scratchy. Strep throat accounts for only a small portion of sore throats. If untreated, strep throat can cause complications, such as kidney inflammation or rheumatic fever. Rheumatic fever can lead to painful and inflamed joints, a specific type of rash or heart valve damage. Strep throat is most common in children, but it affects people of all ages. If you or your child has signs or symptoms of strep throat, see your doctor for prompt testing and treatment.

According to a Danish study , frequent sex may help prevent pre-eclampsia. Researchers believe it's because of a protein found in sperm that can regulate the body's immune system. Yet because the cause of preeclampsia is unknown, it's important to keep your prenatal visits and talk to your doctor about your risk.

Boqueras Causas, Como Se Quitan Las Boqueras, Porque Salen Boqueras En La Boca, Queilitis Angular --- http://queilitis-angular.good-info.co --- Hay Que Actuar Ante Los Primeros Signos De Queilitis Angular. Las Primeras Manifestaciones De Queilitis Angular Suelen Ser Tenues Y Apenas Molestas. Pero No Por Ello Hay Que Ignorarlas, Porque Pueden Derivar En Problemas Mayores. La Queilitis Angular O Lo Que Comúnmente Se Llaman Boqueras, Comienza Por Grietas Minúsculas En Los Extremos De La Boca. También Se Empieza A Sentir Ardor Y Molestias Al Mover Los Labios O Al Abrir La Boca. ¿Qué Sucede Si No Se Atienden De Inmediato Esas Pequeñas Molestias? Difícilmente Se Irán Por Si Solas Sino Que, Por El Contrario, Comenzarán A Agravarse. Las Minúsculas Grietas Se Harán Cada Vez Más Pronunciadas Por El Continuo Movimiento De La Boca. Al Intensificarse Las Grietas Pueden Llegar A Convertirse En Llagas Y A Sangrar. Y Las Infecciones No Tardarán En Aparecer. La Queilitis Angular Puede Ser En Un Primer Momento Molesta Para Quien La Sufre. A Medida Que Avanza, Las Pequeñas Manifestaciones En La Boca Comienzan A Ser Bien Visibles Y Desagradables. Por Lo Que Al Ardor, Picazón Y Dolor, Se Le Suma El Hecho De Querer Ocultar La Afección Ante Los Demás. Cosa Que No Es Fácil De Lograr. A Pesar De Ser Pequeña, La Boca Es Uno De Los Lugares Más Visible Y Observado. Si Hablamos, Comemos, Bebemos, Nuestra Boca Está En Primer Plano. Ante Los Primeros Signos De Queilitis Se Puede Recurrir A Una Crema O Pomada Adecuada, Antiséptica, Antimicótica O Antifúngica. Si Bien Los Extremos De La Boca Deben Permanecer Libres De Saliva O Transpiración, Deben Estar Bien Hidratados. Cualquier Crema Antiséptica Que Se Utilice Debe Ser Libre De Perfumes Y Colorantes Químicos. Debe Detener La Descamación, A La Vez Que Calmar El Picor. El Área Afectada Tendrá Que Permanecer Bien Aseada, Procediendo A Secarla Sin Frotar, Como Para Que No Se Resienta Aún Más La Piel De Los Labios Y Sus Adyacencias. Para Curar La Queilitis Angular No Alcanza Con Los Tópicos Que Se Puedan Utilizar, Por Más Efectivas Que Sean Sus Fórmulas Desde Las Primeras Aplicaciones. Hay Que Llevar A Cabo Una Nutrición Balanceada, Variada Y Suficiente, Con Vitaminas, Minerales Y Oligoelementos. Un Análisis De Laboratorio Podrá Determinar Si Está Haciendo Falta El Aporte De Alguna Vitamina O Mineral. Asimismo, Conviene Evitar Los Lugares Muy Fríos Y/O Húmedos, Así Como Los Espacios Contaminados Por Polvillos O Cualquier Sustancia Irritante Para La Piel. Recomendamos Siempre Actuar Ante Los Primeros Síntomas De Queilitis. Si Se Frena La Dolencia Antes De Que Prospere Y Haga Eclosión, Se Evitará El Sufrimiento Que Puede Implicar Lidiar Contra Lesiones Serias En La Boca. Y Se Evitarán Las Temibles Huellas De Cicatrices Que Pueda Dejar Una Afección Prolongada. ¿Qué Podemos Hacer Ya Mismo? Hoy Existe Un Novedoso Tratamiento, Totalmente Natural Y Muy Simple, Con El Que Se Puede Eliminar La Queilitis Angular O Boqueras En Tan Solo 7 Días (O Menos). Este Revolucionario Sistema Ataca La Verdadera Causa De La Enfermedad Y No Solo Los Síntomas, Asegurando Resultados A Largo Plazo. Si Usted Desea Eliminar Para Siempre Esas Grietas Dolorosas Y La Vergüenza Que Causa Esta Afección, Puede Conocer Este Método De Resultados Comprobados Haciendo Clic En El Siguiente Enlace http://queilitis-angular.good-info.co
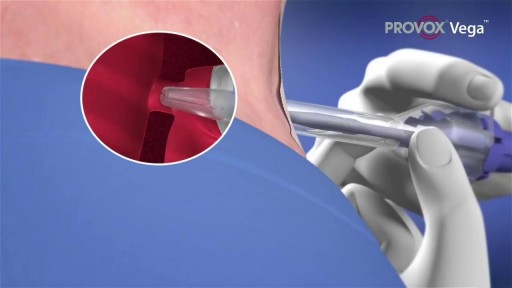
A voice prosthesis (plural prostheses) is an artificial device, usually made of silicone that is used to help laryngectomized patients to speak. During a total laryngectomy, the entire voice box (larynx) is removed and the windpipe (trachea) and food pipe (esophagus) are separated from each other.