Top videos

Routine pelvic exams are important for good reproductive health. A woman should have her first GYN exam when she first thinks about becoming sexually active, when she becomes sexually active or when she turns 18.
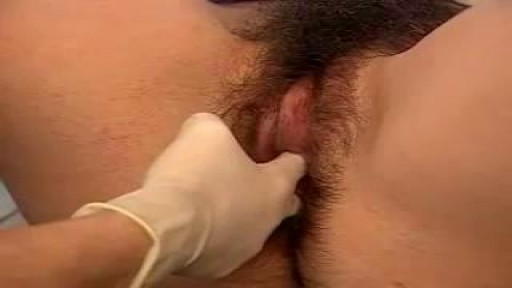
At the gynecologist, you will have a short general physical exam, including a breast exam. You will wear a hospital gown and nothing else. For the actual pelvic examination, you will lie down on an examination table with your feet resting in elevated “stirrups” (props that support your legs in the air). Stirrups might look a little scary, but they are there to keep you comfortable. Your legs will be spread apart, with your knees falling to each side so that your vagina is exposed. You may feel uncomfortable, but relax and realize that everyone goes through this.
External Exam
The practitioner will visually examine your vulva for discoloration, irritation, swelling and other abnormalities, and will gently feel for glands.
Internal Exam
There are two parts to the internal exam. The first involves a speculum, a metal or plastic instrument that the practitioner inserts into the vagina. The speculum is shaped like a duck’s bill, and once it is inserted into the vaginal canal, it is gently widened to spread the interior vaginal walls (this is not painful). As the vaginal walls are spread, the practitioner is able to see the walls of the vagina itself, and up the vaginal canal to the cervix. When viewing the vaginal canal and the cervix, the practitioner can look for discoloration, abnormal discharge, lesions, growths and signs of infection. It is possible for you to look at your own cervix during this process by propping yourself up on your elbows and using a mirror. Some practitioners ask if you would like to do this, but feel free to ask to if she doesn’t mention it first.
Pap Smear
Next the practitioner will take a pap smear. She/he uses a long-stemmed cotton swab to collect a sample of cells in the cervix. Some women feel a slight cramping sensation when their cervix is touched. The collected cells are smeared onto a slide and sent to a lab for testing and examination. The pap smear is extremely important for spotting abnormalities in the cervix which may indicate infection or disease.
STD Testing
If you are sexually active, the practitioner will test for STDs. The gynecologist will swab the inside of the cervix with a long cotton swab. The speculum is then taken out of the vagina. The samples are sent to a laboratory for various STD testing. The tests will probably take a couple days. Ask when your results will be available so you can call. If you want to be tested for HIV, syphilis, genital herpes or hepatitis you need to have blood taken. They can do that as well, but you will need to ask since it is not usually routine.
Manual Exam
The second part of the pelvic exam is called the manual or bi-manual exam. The practitioner will insert one or two fingers into your vagina and press with her/his other hand on the outside of your lower abdomen. They will use a lubricant on their fingers so it is more comfortable. The person can then feel the uterus, fallopian tubes and ovaries, and check for any swelling or tenderness. Once the doctor is finished checking your uterus and ovaries, the exam is complete. The entire pelvic exam (the parts involving your vagina, cervix, uterus, and ovaries) takes 3 to 5 minutes to complete.

Dr. Fizan Abdullah is head of the Division of Pediatric Surgery and vice chair of the Department of Surgery at Ann & Robert H. Lurie Children's Hospital of Chicago. His special interests include Chest wall deformities, pectus excavatum, abdominal wall defects, neonatal surgery, pulmonary and upper airway malformations, congenital diaphragmatic hernia, esophageal and gastrointestinal anomalies, hernia repair, tissue engineering, extracorporeal membrane oxygenation (ECMO), surgical safety protocols and surgical infections.
Learn more at www.luriechildrens.org
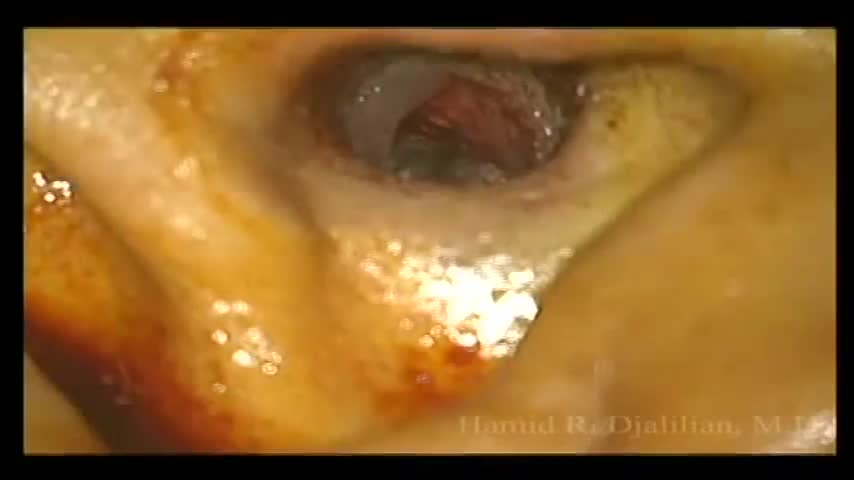
This is a surgery showing the removal of a large exostosis. Exostoses are bony growths in the ear canal from chronic exposure to cold water/air, most commonly from surfing. This patient had growths in both ears, which were completely obstructing the ear canals. This patient had a single exostosis that was blocking this side (the right side).
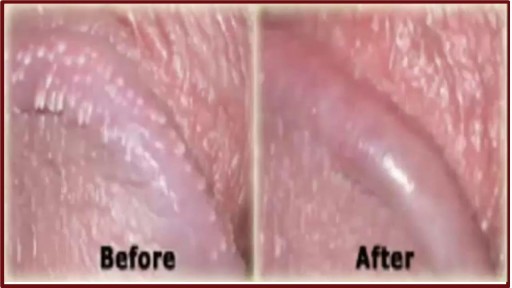
http://penilepapules.plus101.com/ ----- White Spots On Shaft, Pearly Penile Papules Treatment Cream, Single Red Bump On Shaft, Ppp Surgery. Common Home Made Remedies for Pearly Penile Papules. When it comes to treating pearly penile papules many people find it very difficult to reach one of the medical treatments. This is mainly because they are highly expensive and not many people can afford spending large amounts of money on surgery and recovery. In addition to that, these procedures have been reported as being quite risky, which make the men suffering from pearly penile papules think twice before going for one of the available surgeries. This is why, along the time, many homemade, natural treatments have been experienced, so that a cheaper and less risky way of curing pearly penile papules would be found. Some of the methods which have been tried proved to be very less effective, while some did not have any effect at all. Yet, there have also been methods which not only proved to be effective, but they were also considered to be much better than the medical treatment. Most of those who have tried the tea tree oil treatment reported significant diminish of the number of the papules from their penises. In addition to the clearing of the skin, they have also noticed that there were no side effects and the skin remained soft after the papules were removed. As the method was quite simple to put in practice (it requires the application of tea tree oil on the affected area with a cotton swab for three or four times per day), many men decided this was indeed a great solution to their problem.
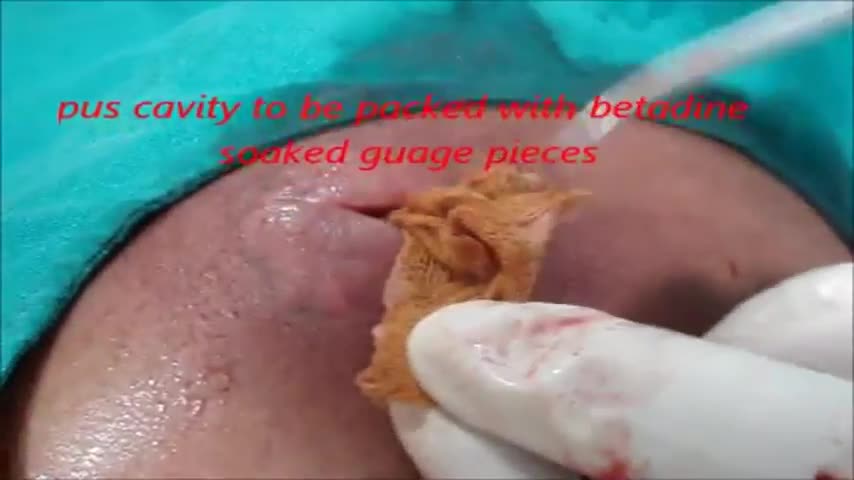
This poor old lady came with swelling in her left buttock for 10 days.She had history of injection in her buttocks two weeks back. She developed painful swelling and redness in her left gluteal region with difficulty in walking.It was diagnosed as injection abscess left gluteal region which needs incision and drainage under local anesthesia.Patient part painted and drapped.2% Lignocaine with adrenaline was infiltrated around the swelling for proper filed block.I use no-11 blade for stab incision over the swelling at the most fluctuating point of the abscess.You can watch how pus was flowing out from the cavity.The aim is to drain all pus from the abscess cavity.Finger exploration is essential to break all loculi inside the cavity, to know the depth and extend of the cavity and to fascilitate proper drainage of residual pus.after pus evacuation,, the cavity should be irrigated with normal saline and betadine solution.lastly the cavity to be packed with betadine soaked guage pieces.Proper dressing is essential.the dressing to be changed after 24 hours.daily dressing is essential with a good antibiotic coverage.the cavity usually obliterates within a period of seven to ten days.
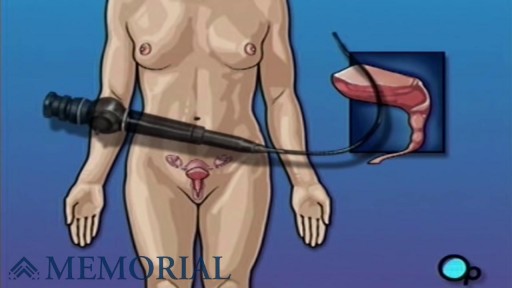
Cystoscopy (sis-TOS-kuh-pee) is a procedure that allows your doctor to examine the lining of your bladder and the tube that carries urine out of your body (urethra). A hollow tube (cystoscope) equipped with a lens is inserted into your urethra and slowly advanced into your bladder.

An animated description of the composition of bones.
Visit www.orthofilms.com for more videos and info.