Top videos
For patients in extremis from respiratory failure or shock, securing vascular access is crucial, along with establishing an airway and ensuring adequacy of breathing and ventilation. Peripheral intravenous catheter insertion is often difficult, if not impossible, in infants and young children with circulatory collapse. Intraosseous (IO) needle placement, shown in the images below, provides a route for administering fluid, blood, and medication. An IO line is as efficient as an intravenous route and can be inserted quickly, even in the most poorly perfused patients.

Toilet Training Boys, Training Potty, Best Way To Potty Train, What Age Do You Potty Train
http://potty-training-fast.good-info.co
Wanna have some fun imagining life without diapers?
Imagine if your child would disappear on their own
one minute and all of a sudden the next minute you
hear the toilet flush and the sink start to run.
Can you imagine it?
Life becomes so much easier the second your child
becomes potty trained and you start to wonder why
you didn't just get it over with sooner...
Would you start potty training right this weekend
if I handed you a guide that guaranteed to get your
child out of diapers in just 3 days?
Click the link below to check it out
http://potty-training-fast.good-info.co
Subscribe to our channel
http://potty-training-fast.blogspot.com/
https://www.youtube.com/watch?v=ck-4RTvP5F4
Toilet Training Boys, Training Potty, Best Way To Potty Train, What Age Do You Potty Train,
3day potty training,
toilet training tips for girls,
how to do potty training,
best potty training book,
potty training boys the easy way,
potty training activities,
how to potty training,
potty training video for toddlers,
when do you potty train,
how to potty train a kid,
potty training at 18 months,
havanese potty training,
how to potty train your baby,

Bone fractures are generally caused by injury, such as a fall, car accident, or sports injury, however, bone fractures can also be caused by osteoporosis. If you have a bone fracture, you must get immediate medical attention and keep the fracture immobilized until you can get help. After the fracture has been immobilized, you can then begin natural remedies to help heal broken bones fast.
Our surgeons take a compassionate, family-centered approach to both inpatient and outpatient care. We’re committed to making sure both you and your child understand our process. Told through a kid's eyes, this video tour reveals our caring approach.
To learn more about pediatric surgery at Stamford Hospital, visit: https://www.stamfordhealth.org..../care-treatment/pedi

In this video, we're going to share 11 things you should NOT do after a tummy tuck. These tips will help you recover from your surgery and keep you from having some common post-tummy-tuck complications. If you're considering a tummy tuck, then be sure to follow these post-operative guidelines!
Dr. William will share all the information you need to make the best decisions for your surgery and recovery. So sit back, relax, and enjoy this video on what NOT to do after an abdominoplasty!
#tummytuck #abdominoplastia #drwilliam
Want a Consultation?
Send us your information: https://drwilliammiami.typefor....m.com/YT-consultatio
Learn more about Dr. William Miami at: https://www.drwilliammiami.com
🔔 Subscribe to our Youtube channel, and stay tuned to all the latest information on cosmetic surgery.
Follow us on Social Media:
Instagram: https://www.instagram.com/drwilliammiami/
Facebook: https://www.facebook.com/Drwilliammiami/
Tiktok: https://www.tiktok.com/@drwilliammiami
OnlyFans: https://onlyfans.com/drwilliammiami
Ogee Recovery: https://ogeerecovery.com
305 Plastic Surgery
564 SW 42nd Ave 3rd floor
Coral Gables, FL 33134
Call us at (305) 209-1030

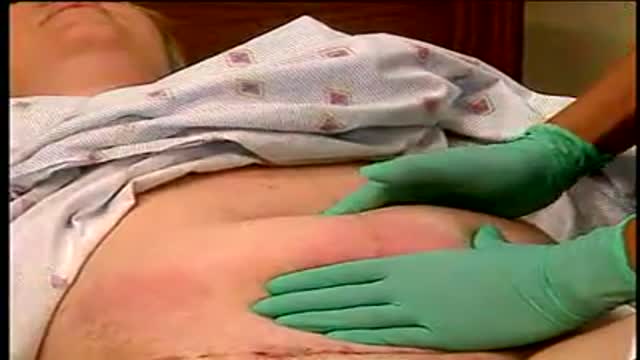
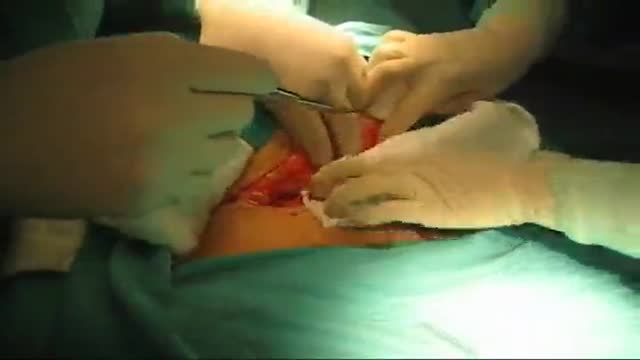
Hernia symptoms test diagnosis and surgery - This lecture explains about hernia symptoms, diagnosis and surgery to cure hernia disease. Stay tuned to this video lecture to get answer of the following questions -
what is hernia disease?
hernia symptoms?
hernia test?
hernia diagnosis?
hernia treatment?
Specifically the hernia surgery is explained in this video. So stay tuned to this video to more about hernia repair and details about hernia symptoms and diagnosis.
Watch this video lecture if you have hernia and want to know about hernia surgery and hernia operation related information.
For more information, log on to-
http://[a]www.shomusbiology.com%2F[/a]
Get Shomu's Biology DVD set here-
http://[a]www.shomusbiology.com%2F[/a]dvd-store/
Download the study materials here-
http://shomusbiology.com/bio-materials.html
Remember Shomu’s Biology is created to spread the knowledge of life science and biology by sharing all this free biology lectures video and animation presented by Suman Bhattacharjee in YouTube. All these tutorials are brought to you for free. Please subscribe to our channel so that we can grow together. You can check for any of the following services from Shomu’s Biology-
Buy Shomu’s Biology lecture DVD set- [a]www.shomusbiology.com%2Fdvd-store[/a]
Shomu’s Biology assignment services – [a]www.shomusbiology.com%2Fassignment[/a] -help
Join Online coaching for CSIR NET exam – [a]www.shomusbiology.com%2Fnet-coaching[/a]
We are social. Find us on different sites here-
Our Website – www.shomusbiology.com
Facebook page- https://www.facebook.com/ShomusBiology/
Twitter - https://twitter.com/shomusbiology
SlideShare- www.slideshare.net/shomusbiology
Google plus- https://plus.google.com/113648584982732129198
LinkedIn - https://www.linkedin.com/in/su....man-bhattacharjee-2a
Youtube- https://www.youtube.com/user/TheFunsuman
Thank you for watching the health tutorial video on Hernia symptoms test diagnosis and surgery.
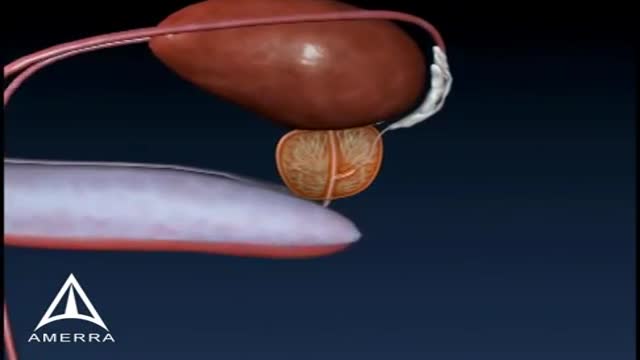
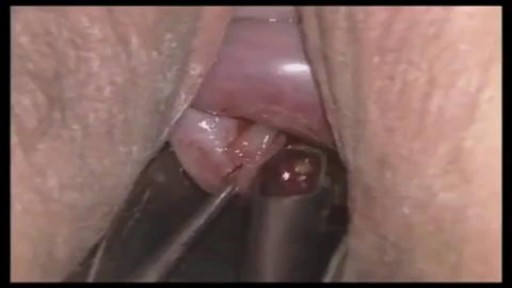
Prostate biopsy is a procedure in which small hollow needle-core samples are removed from a man's prostate gland to be examined microscopically for the presence of cancer. It is typically performed when the result from a PSA blood test rises to a level that is associated with the possible presence of prostate cancer.

Introduction to the Brachial Plexus Examination, 4 of 5 videos demonstrating the physical exam for evaluation of Brachial Plexus conditions.
Brachial plexus injury - Care at Mayo Clinic:
https://www.mayoclinic.org/dis....eases-conditions/bra
Watch all the videos in this series on this playlist:
https://www.youtube.com/playli....st?list=PLSWR1ylG_6J

In this video, we have explained the procedure of total #knee #replacement #surgery in patient in 3D animation.
Learn more: https://ecgkid.com
_____________________________________________________________________
Knee replacement, commonly known as complete knee replacement or knee arthroplasty, is a surgical treatment that resurfaces a knee that has been destroyed by arthritis. The extremities of the bones that make up the knee joint, as well as the kneecap, are capped with metal and plastic pieces. Someone with severe arthritis or a major knee injury may benefit from this procedure.
The knee joint can be affected by a variety of arthritis forms. The degradation of joint cartilage and neighboring bone in the knees can be caused by osteoarthritis, a degenerative joint disease that primarily affects middle-aged and older persons. Rheumatoid arthritis produces pain and stiffness by inflaming the synovial membrane and resulting in an excess of synovial fluid. Traumatic arthritis, or arthritis caused by an injury, can harm the joints.
The purpose of knee replacement surgery is to resurface damaged areas of the knee joint and cure knee discomfort that has not responded to prior therapies.

Having surgery can be frightening for anyone, but it's especially scary for kids who don't always understand what's going on, or what the grown-ups are saying. We're here to help!
Join Avrie, who had surgery at the Sacred Heart Children's Hospital pediatric surgery center in Spokane, WA. Maybe after watching and hearing her story, you and your kiddo will feel better about having surgery in the hospital.
Follow Avrie's trip - from check-in, vital signs and pre-op checks; meeting the doctor who will do his surgery, along with the anesthesiologist, surgery nurse and the Child Life Specialist; the trip to the Operating Room; waking up in the recovery room with his mom by his side; and getting ready to go home.
To learn more about the pediatric surgery center at Sacred Heart Children's Hospital, visit https://washington.providence.....org/locations-direct