Top videos
![Female Foley Insertion (Urinary Catheter) [How to Insert Nursing Skills]](https://i.ytimg.com/vi/Mq4Yh0-iozY/maxresdefault.jpg)
Pass your tests and improve your grades with the below FREE resources:
1) A FREE 140 Must Know Meds book
Click here to get your FREE copy of the 140 Must Know Meds Book: https://bit.ly/41rxSt0
2) A FREE test-taking tips webinar
Join us for our free test-taking tips webinar to boost your exam scores: https://bit.ly/nursingtesttaking
You can now test your knowledge with a free lesson quiz on NURSING.com!
Click here to take a free quiz: https://bit.ly/3HwJr8t
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full lesson on Female Foley Insertion here:
https://nursing.com/lesson/ski....lls-03-01-inserting-
Get the Male Foley Insertion lesson here:
https://nursing.com/lesson/ski....lls-03-02-inserting-
Get the Sterile glove application lesson here:
https://nursing.com/lesson/ski....lls-01-04-sterile-gl
Check out our new Nurse Care Plan Lessons here:
https://bit.ly/3BPRfPL
Get Access to Thousands of Lessons here:
https://nursing.com/courses/
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
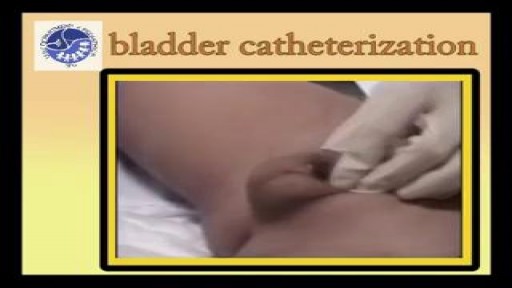
Female Foley Insertion (Urinary Catheter)- Nursing Skills
In this video, we’re going to look at inserting a Foley catheter in a female. Of course make sure you’ve verified your order and told the patient what’s happening. You’ll also typically want to perform perineal care before you start. Then, you’ll want to assist the patient into the appropriate position. For females, that’s supine with their knees bent and feet close to their hips – allowing their knees to fall to the side. You may need a helper to help hold the patient in this position. We love you guys! Go out and be your best selves today! And, as always, happy nursing!
Bookmarks:
0.05 Female Foley insertion introduction
0.15 Patient positioning
0.27 Opening the sterile kit
1.41 Setting up the sterile field
2.25 Prepping the remaining Foley kit items
2.34 Catheter lubrication
3.00 Saline syringe attachment
3.10 Iodine, swabs and cleansing the area
3.52 Catheter insertion (into urethra)
4.06 Balloon inflation
4.25 Final catheter setting
4.31 Securing the catheter and bag
4.48 Discarding your supplies
5.00 Documentation
5.08 Foley insertion outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.

There are lots of fallacies about the missionary position being the best position for getting pregnant. With the woman on her back and her partner on top, it is thought that gravity will assist the sperm to swim upwards towards the egg.

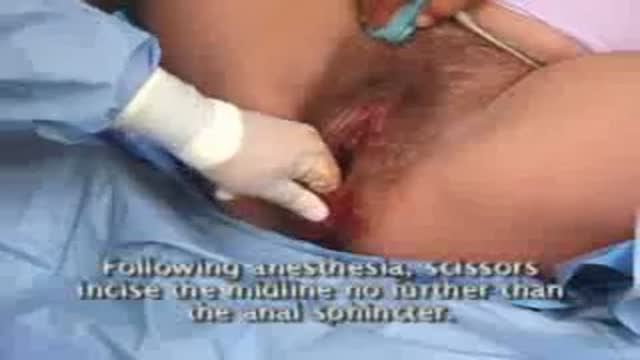
A digital rectal examination (DRE) is a simple procedure doctors use to examine the lower rectum and other internal organs. A DRE is done for a number of reasons. It's a quick, easy way to check the health of a man's prostate gland. It can detect conditions like an enlarged prostate
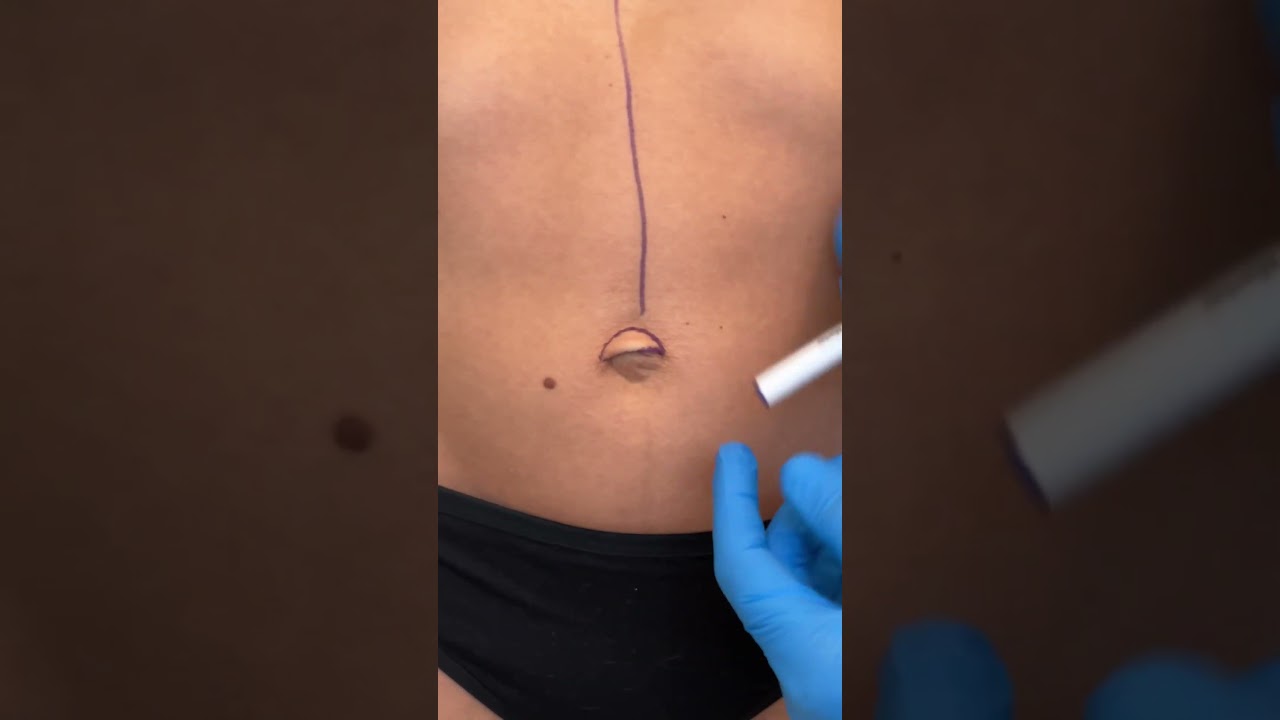
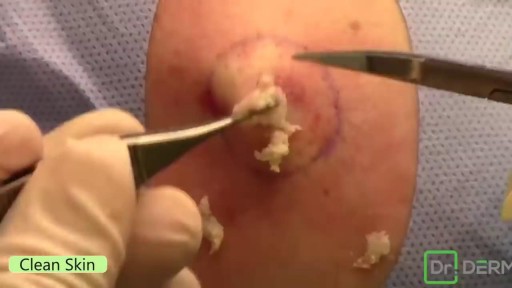
Check out @barrettplasticsurgery on TikTok!
Like and subscribe for more! #shorts #medical #plasticsurgery
More information:
www.drdanielbarrett.com