Top videos

Watch more clips of Dr. James Kelly - https://www.youtube.com/playli....st?list=PLe2Je5-cHxP And for more information about brain injury and PTSD, please visit us at https://www.brainline.org.
Watch more clips of Pat LaFontaine - https://www.youtube.com/playli....st?list=PL5F3273C3C8
© 2018 WETA All Rights Reserved

Many U.S. hospitals still perform traditional surgery, over minimally invasive procedures, according to Johns Hopkins University researchers. Also, a new study on HPV vaccines. Wendy Gillette reports on the day's top health stories.

Ellis demonstrates how to connect an NG tube to suction.
#NCLEX #ClinicalSkills #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #NurseEducator
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.
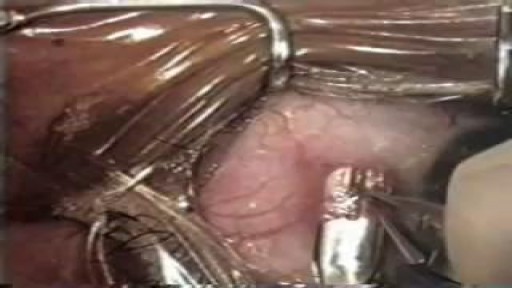
UPMC liver surgeons are among the most experienced in the world in performing minimally invasive liver surgery. Most patients benefit from less trauma and pain, minimal scarring, a shorter hospital stay, and faster recovery than from traditional surgery.
To learn more, please visit https://www.upmc.com/services/....liver-cancer/treatme

Glass ampules are often used to store medication, and as a nurse, you'll need to know how to use them.
In this video, I demonstrate how to clean an ampule using alcohol prep, how to open (or break) an ampule, as well as how to dispose of the ampule.
In addition, I show how to use an ample filter straw while drawing up (withdrawing) medication, how to use the syringe, and how to remove the air bubbles in the syringe.
This is another video in our series on clinical nursing skills.
Notes: https://www.registerednursern.....com/how-to-withdraw-
Website: https://www.registerednursern.com/
More Videos: https://www.youtube.com/watch?v=R2XMro13dD0&list=UUPyMN8DzkFl2__xnTEiGZ1w
Nursing Gear: https://teespring.com/stores/registerednursern
Instagram: https://www.instagram.com/registerednursern_com/
Facebook: https://www.facebook.com/RegisteredNurseRNs
Twitter: https://twitter.com/NursesRN
Popular Playlists:
NCLEX Reviews: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Fluid & Electrolytes: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing Skills: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Types of Human Body Tissue
In this video, I review four types of tissue.
Connective tissue, epithelial tissue, muscle tissue, and nerve tissue.
Tissues are made up of cells working together.
*
*
For more Life Science videos and summaries see,
http://www.moomoomath.com/Midd....le-School-Science-an
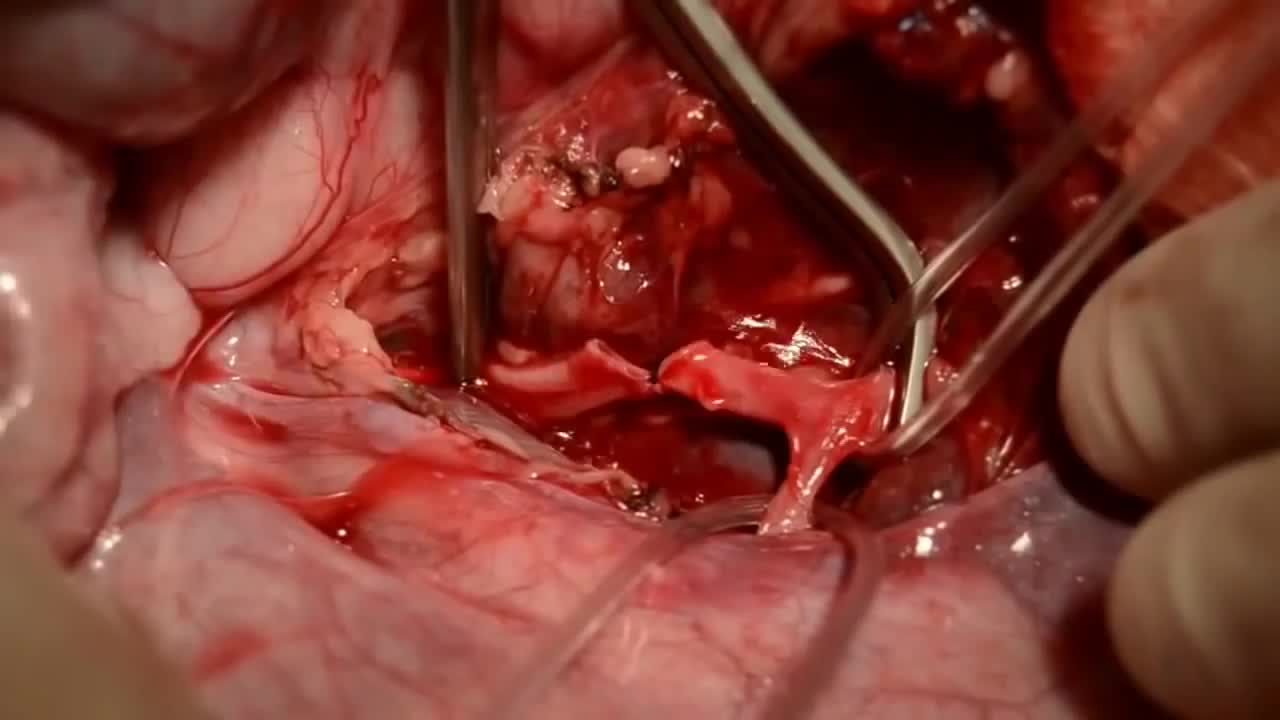
Throughout the body, there are several points at which blood vessels unite. The junctions are termed anastomoses. In the simplest sense, an anastomosis is any connection (made surgically or occurring naturally) between tube-like structures. Naturally occurring arterial anastomoses provide an alternative blood supply to target areas in cases where the primary arterial pathway is obstructed. They are most abundant in regions of the body where the blood supply may can be easily damaged or blocked (such as the joints or intestines). This article focuses on the arterial anastomotic networks of the upper limb.

The dentin is a hard tissue that forms the bulk of the tooth. It is similar to bone but is slightly harder, although softer than enamel. The dentin has numerous dentinal tubules that run across its length. Each dentinal tubule houses the cytoplasmic process of an odontoblast (odontoblastic process).
📄Notes for the video: https://www.hackdentistry.com/....bundles/revision-nin
💻Website: https://www.hackdentistry.com/
📰Blog: https://hackdentistry.substack.com/
Study resources on our website-
📖Oral pathology Revision Ninja (Notes, Videos & MCQs): https://www.hackdentistry.com/bundles/oral-pathology-revision-ninja
📖Oral Histology Revision Ninja (Notes, Videos & MCQs): https://www.hackdentistry.com/....bundles/revision-nin
📖Periodontics Revision Ninja (Notes & MCQs): https://www.hackdentistry.com/bundles/perio-rn
📖Question Bank: https://www.hackdentistry.com/bundles/question-bank
📖Access all content: https://www.hackdentistry.com/bundles/all-access-premium
References and further reading:
💡Berkovitz BKB, Hollan GR, Moxham BJ. Oral Anatomy, Histology and Embryology. 4th ed. Mosby Elsevier; 2009.
💡Nanci A. Tencate’s Oral Histology. Development, Structure and Function. 8th ed. Elsevier; 2013.
💡Kumar GS. Orban’s Oral Histology and Embryology.13th ed. Elsevier; 2011.
💡Avery JK. Oral development and Histology. 3rd ed. Thieme Medical Publishers; 2002.
Log in to https://www.hackdentistry.com and get access to:
I) Numerous Notes/Cheatsheets and Videos II) Thousands of quiz questions from our vast Question Bank!
HackDentistry is an edtech company that aims make learning dentistry fun,engaging and light hearted.
1) It focuses on helping students understand and retain core concepts in dentistry through highly visual sketch/whiteboard style video animations.
2) The platform helps improve exam performance by providing Revision Bundles and allowing students to test themselves using thousands of Practice Questions from a vast Question Bank. (multiple choice format).
3) It also provides for a community platform where students can come together, and engage with fellow dental students and dentists across the globe!
Facebook:
https://www.facebook.com/hackdentistry
Instagram:
https://www.instagram.com/hack.dentistry/
Twitter:
https://twitter.com/hckdentistry

Common Benign Pain Syndromes--Symptoms and Etiology:
1. Non-specific musculoskeletal pain: This is the most common cause of back pain. Patients present with lumbar area pain that does not radiate, is worse with activity, and improves with rest. There may or may not be a clear history of antecedent over use or increased activity. The pain is presumably caused by irritation of the paraspinal muscles, ligaments or vertebral body articulations. However, a precise etiology is difficulty to identify.
2. Radicular Symptoms: Often referred to as "sciatica," this is a pain syndrome caused by irritation of one of the nerve roots as it exits the spinal column. The root can become inflamed as a result of a compromised neuroforamina (e.g. bony osteophyte that limits size of the opening) or a herniated disc (the fibrosis tears, allowing the propulsus to squeeze out and push on the adjacent root). Sometimes, it's not precisely clear what has lead to the irritation. In any case, patient's report a burning/electric shock type pain that starts in the low back, traveling down the buttocks and along the back of the leg, radiating below the knee. The most commonly affected nerve roots are L5 and S1.
3. Spinal Stenosis: Pain starts in the low back and radiates down the buttocks bilaterally, continuing along the backs of both legs. Symptoms are usually worse with walking and improve when the patient bends forward. Patient's may describe that they relieve symptoms by leaning forward on their shopping carts when walking in a super market. This is caused by spinal stenosis, a narrowing of the central canal that holds the spinal cord. The limited amount of space puts pressure on the nerve roots when the patient walks, causing the symptoms (referred to as neurogenic claudication). Spinal stenosis can be congenital or develop over years as a result of djd of the spine. As opposed to true claudication (pain in calfs/lower legs due to arterial insufficiency), pain resolves very quickly when person stops walking and assumes upright position. Also, peripheral pulses should be normal.
4. Mixed symptoms: In some patients, more then one process may co-exist, causing elements of more then one symptom syndrome to co-exist.