Top videos

Progressive multifocalleukoencephalopathy is a demyelinating illness of the central nervous system that typically occurs in immunosuppressed patients, especially those with AIDS. It is caused by reactivation of the polyomavirus JC (JC virus) and presents with neurologic deficits including hemiparesis, gait ataxia, visual symptoms, and altered mental status. It is not seen in non-immunosuppressed patients, and fever is not typical

ADC was first identified early in the AIDS epidemic as a common and novel CNS syndrome.(4,5) The three components of the term, AIDS dementia complex embody central features of the condition. AIDS emphasizes its morbidity and poor prognosis, particularly when its severity is at stage 2 or greater (see Table 1), a severity comparable to other clinical AIDS-defining complications of HIV-1 infection. Dementia designates the acquired and persistent cognitive decline with preserved alertness that usually dominates the clinical presentation and determines its principal disability. Complex emphasizes that this disease not only impairs the intellect, but also concomitantly alters motor performance and, at times, behavior. This involvement of the nervous system beyond cognition is evidence of a wider involvement of the CNS than occurs in some other types of dementia such as Alzheimer's disease. Additionally, myelopathy may be an important, indeed predominating, aspect of ADC, and organic psychosis may also be a feature in a subset of patients (see Rheumatologic and Musculoskeletal Manifestations of HIV). These manifestations are therefore also encompassed within this term. By contrast, neither neuropathy nor functional psychiatric disturbance are included in ADC.

Acute intermittent porphyria (AIP) is a rare autosomal dominant metabolic disorder affecting the production of heme, the oxygen-binding prosthetic group of hemoglobin. It is characterized by a deficiency of the enzyme porphobilinogen deaminase.

Hemolytic-uremic syndrome (or haemolytic-uraemic syndrome), abbreviated HUS, is a disease characterized by hemolytic anemia (anemia caused by destruction of red blood cells), acute kidney failure (uremia), and a low platelet count (thrombocytopenia).
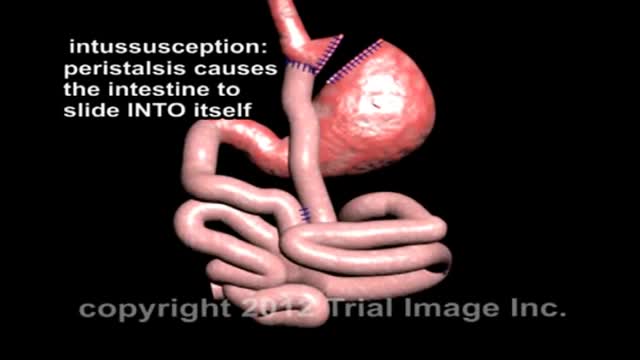
In cases when the presentation is unclear, ultrasonography is the imaging methodology of choice. The characteristic finding is the presence of a "target sign". Ultrasonography is not required in patients with obvious clinical diagnosis (as seen in this patient). Such patients can proceed directly to treatment with diagnostic and therapeutic air (pneumatic) or water-soluble (hydrostatic contrast) enema.

This is a Video in Clinical Medicine from the New England Journal of Medicine. Tympanocentesis in Children with Acute Otitis Media Overview Tympanocentesis is defined as needle aspiration of fluid from the middle ear. In children with acute otitis media, drainage of pus from the middle ear results in a rapid and marked improvement in symptoms and enables the clinician to prescribe tailored antimicrobial therapy. This video will demonstrate the technique of tympanocentesis. Indications Tympanocentesis is recommended in children with refractory acute otitis media, in immunocompromised children with otitis media, and in children with suppurative complications of acute otitis media, . . . .

Body Mass Index (BMI) is a person's weight in kilograms divided by the square of height in meters. A high BMI can be an indicator of high body fatness. BMI can be used to screen for weight categories that may lead to health problems but it is not diagnostic of the body fatness or health of an individual.May 15, 2015

There is a strong association with obesity. In children younger than 10 years, it is associated with metabolic endocrine disorders {hypothyroidism, panhypopituitarism, hypogonadism, renal osteodystrophy, growth hormone abnormalities). SCFE is considered chronic if it has been present more than 3 weeks and acute if it has been present for 3 weeks or less. It is called "stable" if the patient can bear weight and "unstable" if the patient cannot ambulate. Unstable SCFE is associated with more complications, including avascular necrosis of the femoral head (AVN). SCFE is diagnosed by x-ray of the pelvis and bilateral hips. The underlying cause is a widened epiphyseal growth plate, due to abnormal cartilage maturation and endochondral ossification. The treatment is surgical, requiring immediate internal fixation with a single screw. Delay in treatment {> 24 hours) leads to increased AVN, SCFE progression from stable to unstable, and high risk of future degenerative arthritis. Prophylactic contralateral fixation of the unaffected hip is not routinely done in the U.S., except in patients with endocrine abnormalities.

This patient's age, speech delay, bilateral lower-extremity weakness, apparent increase in calf diameter, and history of a wheelchair-bound uncle are typical of Duchenne muscular dystrophy (DMD). DMD is the most common muscular dystrophy of childhood that affects boys who have inherited a defective dystrophin gene on X-chromosome p21. Weakness begins in the proximal lower-extremity muscles and manifests as difficulty walking, running, jumping, and climbing stairs. Boys may push their arms on their thighs (Gower sign) to transition from sitting to standing.
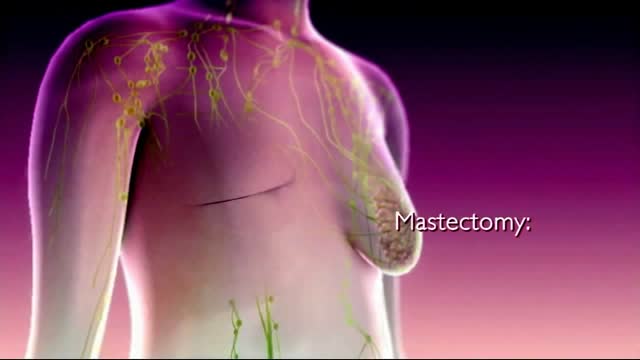
For both DCIS and invasive cancer, radiation therapy to the remaining breast tissue is generally recommended after surgery. A lumpectomy may also be called breast-conserving surgery, a partial mastectomy, quadrantectomy, or a segmental mastectomy. A mastectomy is the surgical removal of the entire breast.

The cause of HELLP syndrome is unknown, but there are certain factors that may increase your risk of developing it. Preeclampsia is the greatest risk factor. This condition is marked by high blood pressure and swelling, and it typically occurs during the last trimester of pregnancy.