Top Videos

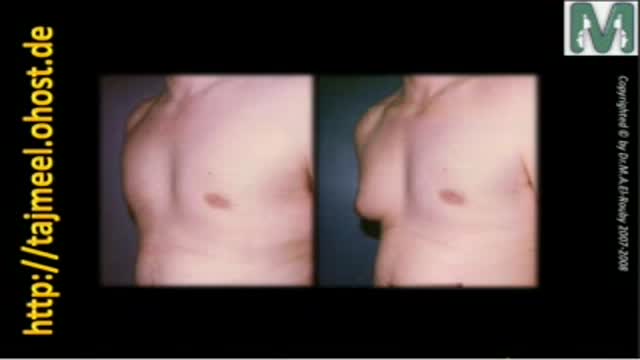
Breast reduction can relieve strain from shoulder straps, neck, back, and upper arms.
It can provide an uplift to help clothes fit and look better. Traditionally, insurance companies would provide benefits for a broad range of breast sizes and gram weight of tissue to be removed from each breast. At present most insurance companies limit authorization when the doctor plans to remove less than 500gm weight per breast. Since many patients present with symptoms in a D cup to DD cup, often, the very removal of over 500 grams weight may reduce the breasts too much. This amount of reduction may not be in harmony with body shape. Newer methods of breast assembly after reduction, will tighten things using internal brassiere techniques that also compact and reduce breast volume. Therefore, a gram weight reduction of 500gms in some patients combined with internal tightening efforts, could pose an over-reduction. With the unreliability of insurance support in some cases, it is best not to look solely at gram weight in the surgical planning of breast reduction. When excess skin and weight is removed, the improved location of the breasts on the chest will give marked relief of symptoms.
Surgery takes from 2 to 5 hours and can be done as an outpatient or with a brief overnight stay. When possible, no scarring other than around the areola can be planned which follows the Brazilian and French methods (Goes and Benelli). For very large reductions, a vertical method, or T pattern approach is offered. Recovery is a few days, with special care to avoid strain for 4 to 6 weeks. Some soreness may persist for a few weeks. The breasts can appear tight, swollen, and bruised at first, but will usually settle to their near final look by 6 weeks. There may be sutures to be removed in some cases. Costs relate to the severity of the sag, and weight of the breasts.
The operation can make a stunning change in body image, relief of upper body symptoms, and offer a cosmetic lift to naturally sloping breasts.

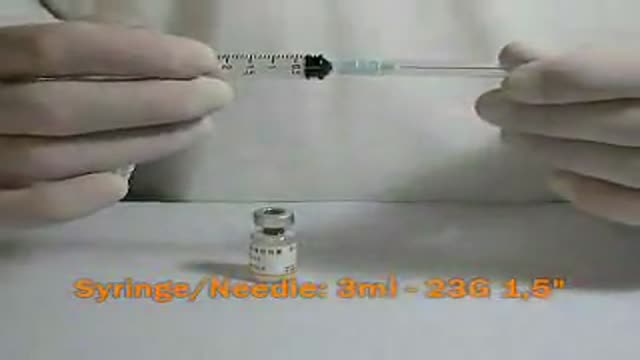
If you are a medical student, a resident, a primary care physician or you practice in an emergency department, you can improve your suture skills with this detailed instruction. As you practice towards a cosmetically perfect technique, your confidence will increase, especially when dealing with complex wounds. Areas of study include: methods of closure, closure materials, anesthetics, suture removal, infection, prophylaxis, when to call in a plastic surgeon, recapping techniques and more
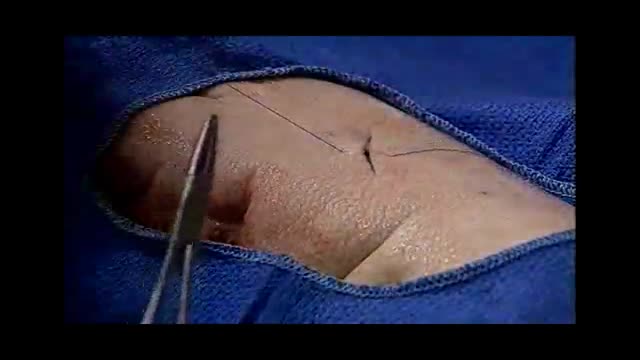
are you a medical student, a resident, a primary care physician or you practice in an emergency department, you can improve your suture skills with this detailed instruction. As you practice towards a cosmetically perfect technique, your confidence will increase, especially when dealing with complex wounds. Areas of study include: methods of closure, closure materials, anesthetics, suture removal, infection, prophylaxis, when to call in a plastic surgeon, recapping techniques and more

This endoscopy shows a patient with cancer of the larynx, Laryngeal cancer is the most common cancer of the upper respiratory tract. The incidence of laryngeal tumors is closely correlated with smoking, as head and neck tumors occur 6 times more often among cigarette smokers than among nonsmokers. The age-standardized risk of mortality from laryngeal cancer appears to have a linear relationship with increasing cigarette consumption. Death from laryngeal cancer is 20 times more likely for the heaviest smokers than for nonsmokers. It should be suspected in any patient with hoarseness of the voice for three weeks or longer until proven otherwise.