Top videos

How to Imporve Sexual Health or Stamina Part 2 https://youtu.be/S17bCnwCLuI Dr. Aslam Naveed is a well known sexologist in Pakistan. He has treated more than 1 Lac patients since last 30 years of clinical Practice in sexology, he knows how to help the people facing sexual disorders. Contact: 021-34595050, 03432821919 sexologistpakistan.com facebook.com/menssexcareclinic/ Address: Men's Care Clinic, 2nd floor, The Modern Hospital Opposite Safari Park, University Road. Karachi.

Visit http://www.vipmedicalgroup.com or call us at (877) 739-5306 for more information on minimally invasive pain management treatments. At VIP Centers, we offer pain management services such as treatment for neck pain, back pain, shoulder pain, hip pain, knee pain, or any other joint pain related injury. Our highly skilled team of doctors are Harvard trained and Board Certified. They have a wealth of experience in pain medicine, sports medicine, bone and joint inflammation. The procedures we offer do not require a hospital stay, general anesthesia, or painful surgery. This means you can return to your normal activities immediately after your treatment.

Cameron Underwood Face Transplant Surgical Animation 2018 Eduardo D. Rodriguez, MD, DDS, chair of the Hansjörg Wyss Department of Plastic Surgery, and the Helen L. Kimmel Professor of Reconstructive Plastic Surgery, details the recent face transplant he performed on Cameron Underwood in January 2018 at NYU Langone Health.

How to Improve Sexual Health or Stamina Part 4 All Solution of Male Disorder Male Infertility Diagnostic and Treatment Re-Slim Care Latest Technology in Pakistan Dr. Aslam Naveed is a well known sexologist in Pakistan. He has treated more than 1 Lac patients since last 30 years of clinical Practice in sexology, he knows how to help the people facing sexual disorders. Contact: 02134965050, 03432821919 https://www.facebook.com/menssexcareclinic/ ADDRESS: Men’s Care Modern Hospital, Opposite, Safari Park, University Road, Karachi, Pakistan.

How to Improve Sexual Health or Stamina part 4 All Solution of Male Disorder Male Infertility Diagnostic and Treatment Re-Slim Care Latest Technology in Pakistan Dr. Aslam Naveed is a well known sexologist in Pakistan. He has treated more than 1 Lac patients since last 30 years of clinical Practice in sexology, he knows how to help the people facing sexual disorders. Contact: 02134965050, 03432821919 www.sexologistpakistan.com https://www.facebook.com/menssexcareclinic/ https://youtu.be/_fRbtwWtLoE Part 1 https://youtu.be/S17bCnwCLuI Part 2 https://youtu.be/CPAXxkdz7mM Part 3 https://youtu.be/YlsdBZJ4prg Part 4 https://youtu.be/fylxbK4azvs Part 5 https://youtu.be/Zb8TcdgJ7Io Part 6 https://youtu.be/0wbDDNAwsmo Part 7 https://youtu.be/gHDmwfsMgTw Part 8 https://youtu.be/IasXoRKUlV4 Part 9 ADDRESS: Men’s Care Modern Hospital, Opposite, Safari Park, University Road, Karachi, Pakistan.

All Solution of Male Disorder Male Infertility Diagnostic and Treatment Re-Slim Care Latest Technology in Pakistan Dr. Aslam Naveed is a well known sexologist in Pakistan. He has treated more than 1 Lac patients since last 30 years of clinical Practice in sexology, he knows how to help the people facing sexual disorders. Contact: 02134965050, 03432821919, 0345-8314663 http://www.sexologistpakistan.com/ https://www.facebook.com/menssexcareclinic/ https://www.youtube.com/channel/UCagSSgdEgQJWl_xfFM12BwA https://twitter.com/bettersexcare https://www.instagram.com/dr.aslamnaveed/ ADDRESS: Men’s Care Modern Hospital, Opposite, Safari Park, University Road, Karachi, Pakistan.

Cathy covers hemodialysis, including nursing care before, during, and after the procedure. Peritoneal dialysis, including nursing associated with the procedure. Key complications of hemodialysis, including disequilibrium syndrome and hypotension. Peritonitis, which is a key complication of peritoneal dialysis. Post-op nursing care and patient teaching associated with a kidney transplant.
Our Medical-Surgical video tutorial series is taught by Cathy Parkes BSN, RN, CWCN, PHN and intended to help RN and PN nursing students study for their nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #KidneyTransplant #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN #Renal #Hemodialysis
0:00 What to Expect
0:31 Hemodialysis
2:06 Nursing Care
2:47 Peritoneal Dialysis
3:23 Nursing Care
4:09 Dialysis Complications
4:19 Disequilibrium Syndrome
4:55 Hypotension
5:26 Peritonitis
5:57 Kidney Transplant
6:17 Nursing Care
6:40 Signs and Symptoms
6:51 Patient Teaching
7:17 Quiz Time!
8:27 Bloopers
🚨Head over to our interactive study guide and index ANYTIME and find out exactly which card we’re referencing. https://bit.ly/MedSurgIndex
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Medical-Surgical Nursing? Check out our flashcards, review games, videos, tips & more!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/AllMedSurg 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.

Dialysis patients need to choose their heart medicine carefully, as Canadian researchers say that some beta blockers are easily removed from the blood during treatment. Also, people who eat a Mediterranean diet may decrease their risk of developing kidney problems. Eboni Williams reports on the day's top health news.

For more information on peritoneal dialysis: https://www.massgeneralbrigham.....org/en/about/newsro
Why does someone need dialysis? What is peritoneal dialysis? How does it work? John Kevin Tucker, M.D., Nephrologist at Brigham and Women's Hospital and Vice President for Education at Mass General Brigham, discusses peritoneal dialysis and its benefits for people who have lost their kidney function.
Subscribe Link: https://www.youtube.com/channe....l/UCYrLjATd88gPwIKnt
0:00 - Intro
0:24 - Why Do I Need Dialysis?
1:42 - Treatment
2:02 - Why Is It Called Peritoneal Dialysis
2:35 - 2 Forms of Peritoneal Dialysis
3:50 - Continuous Cycling Peritoneal Dialysis
4:38 - Myths
5:55 - Preparing For Peritoneal Dialysis
About Mass General Brigham:
Mass General Brigham combines the strength of two world-class academic medical centers, five nationally ranked specialty hospitals, 11 community hospitals, and dozens of health centers. Our doctors and researchers accelerate medical breakthroughs and drive innovations in patient care. They are leaders in medical education, serving as Harvard Medical School faculty and training the next generation of physicians. Mass General Brigham’s mission is to deliver the best, affordable health care to patients everywhere. Together, we transform the health of our communities and beyond.
#MassGeneralBrigham #Peritoneal #Dialysis
Visit Mass General Brigham: https://www.massgeneralbrigham.org/
Find us on social:
Twitter: https://twitter.com/MassGenBrigham
Instagram: https://www.instagram.com/massgeneralbrigham/
Facebook: https://www.facebook.com/MassGeneralBrigham/
LinkedIn: https://www.linkedin.com/compa....ny/mass-general-brig
Mass General Brigham:
https://www.youtube.com/massgeneralbrigham
Peritoneal Dialysis: At Home Treatment for Kidney Failure | Mass General Brigham
https://youtu.be/of1T6hMEN_Q

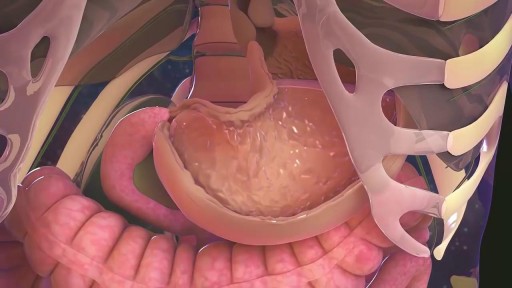
The objectives of hemodialysis are to extract toxic nitrogenous substances from the blood and to remove excess water. In hemodialysis, the blood, laden with toxins and nitrogenous wastes, is diverted from the patient to a machine, a dialyzer, in which the blood is cleansed and then returned to the patient. Diffusion, osmosis, and ultrafiltration are the principles on which hemodialysis is based.
The toxins and wastes in the blood are removed by diffusion—that is, they move from an area of higher concentration in the blood to an area of lower concentration in the dialysate. The dialysate is a solution made up of all the important electrolytes in their ideal extracellular concentrations.
The electrolyte level in the patient’s blood can be brought
under control by properly adjusting the dialysate bath. The semipermeable membrane impedes the diffusion of large molecules,
such as red blood cells and proteins.
#hemodialysis #dialysis #viral #urinaryinfection #shorts #medical #animation
![What does a fistula for dialysis look like? [CHT CERTIFICATION REVIEW] 2022](https://i.ytimg.com/vi/gjB5eKo4eh8/maxresdefault.jpg)
If this is the first time visiting us, make sure to subscribe to our channel here: https://bit.ly/2yXNBYp
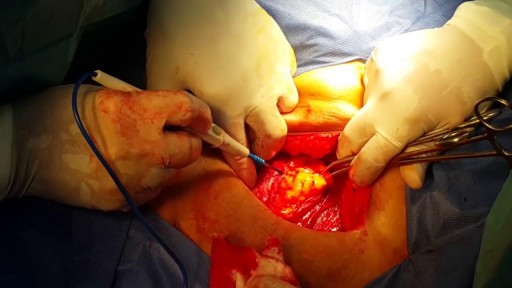
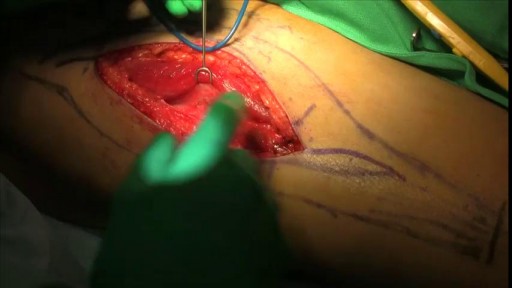
What does a fistula for dialysis look like?
A fistula for dialysis is a surgical connection between a vein and an artery.
In this video, I will show you a real fistula and how we should evaluate it before a dialysis connection.
Additional videos:
💉How to properly cannulate a fistula: https://youtu.be/IqoHnzFyhJQ
💉 What is a fistula for dialysis treatment: https://youtu.be/B5EEf-MklFk
💉 The 10-second assessment for fistulas: https://youtu.be/Uqo0LhjZSI8
💉 If you would like to be trained as a dialysis professional focused on offering quality of care to renal patients, visit our program details here: https://utopiahcc.com/hemodialysis-technician/
For nursing and technician schools😷 🩺 🎓, we can offer a special renal failure class to your students. For inquiries please contact us: info@utopiahcc.com
Where to find us:
Facebook: https://www.facebook.com/utopiahealth
Email: info@utopiahcc.com
Website: utopiahcc.com
🤔 Looking for renal and dialysis continuing education for your certification renewal? Check out our CE package where you will get a little over 40 contact hours for a small price and receive your certificates immediately.
Here's the link: https://bit.ly/3dbPvDZ
Want to watch *Free Dialysis Training Videos*?
https://utopiahcc.com/free-dia....lysis-video-training
__________________________________________________________
Additional resources:
What Does a Healthy AV Fistula Look Like? | Azura Vascular ...
www.azuravascularcare.com infodialysisaccess healt...
Jul 17, 2018 — An AV fistula is a surgically-created permanent access located under the skin, making a direct connection between a vein and an artery. An AV fistula is typically created in the non-dominant arm. If the veins in your arm are not large or healthy enough to support a fistula, it may be created in your leg.
Preparing for Dialysis (AV Fistula) Fact Sheets Yale ...
www.yalemedicine.org › conditions › preparing-dialysi...
To undergo dialysis, patients need a surgical procedure to create an access point for the dialysis machine. An AV fistula is the most common access point.
Vascular Access for Hemodialysis - Life Options
lifeoptions.org living-with-kidney-failure vascular-a...
Jump to How a Catheter Looks and Feels — This makes a pattern that looks a bit like a rope ladder. The next best way—for fistulas ONLY—is the “Buttonhole ...
Fistula or Graft Surgery · Needle Fear · How a Fistula or Graft Looks...
Taking Care of Your Fistula - DaVita
www.davita.com dialysis preparing-for-dialysis › ta...
An arteriovenous (AV) fistula is a type of access used for hemodialysis. ... access because it utilizes the patient's own vessels and does not require permanent placement of foreign materials such ... Look for redness or swelling around the fistula area. ... This sound may change from a whooshing noise to a whistle-like sound.
Vascular Access for Hemodialysis - Department of Surgery
surgery.ucsf.edu conditions--procedures vascular-ac...
The patient does not need anesthesia for this procedure. ... A vascular surgeon performs AV graft surgery, much like AV fistula surgery, in an outpatient center or ...
Frequently Asked Questions about Dialysis Access Surgery ...
www.bidmc.org transplant-institute frequently-aske...
Dialysis access surgery creates the vascular opening so a needle can be inserted for ... fluid and to correct electrolytes like potassium, sodium, phosphate and calcium, to name a few. ... Where are AV fistulas located and how long do they last?
Fistula and Graft Placement (Eric K. Peden, MD) - YouTube
www.youtube.com watch
Mar 28, 2016 — ... Bootcamp 2015 August 14 - 16, 2015 "Dialysis Access" Fistula and Graft Placement (Eric K. Peden, MD) DICET@Houstonmethodist.org.