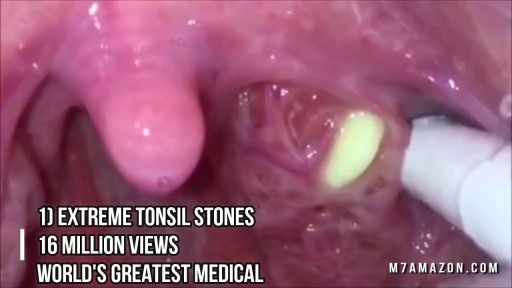
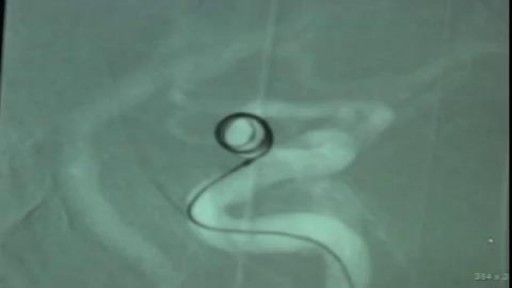
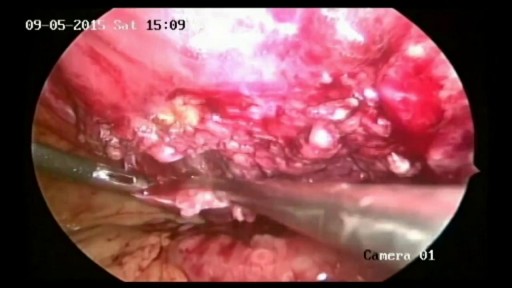
Top videos
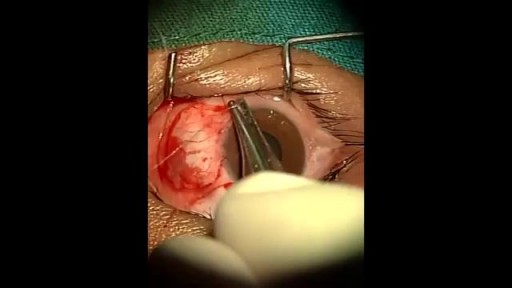
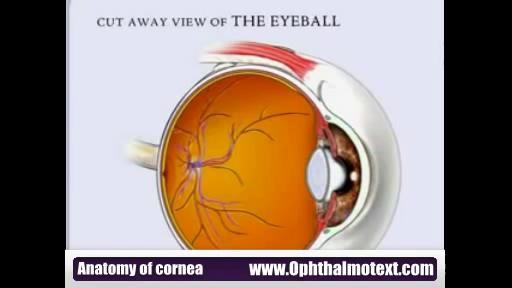
An eye web is a noncancerous, triangular growth that may occur on one or both eyes. It's more common in people who spend a lot of time in the sun, such as those who work outdoors. The painless growth may be slightly raised and contain obvious blood vessels. It may cause irritation and possibly affect vision. Treatment usually isn't necessary. Eyedrops or surgery may help in severe cases.
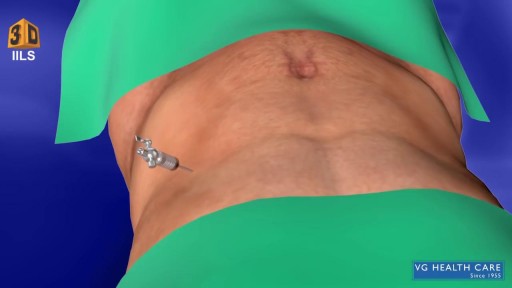
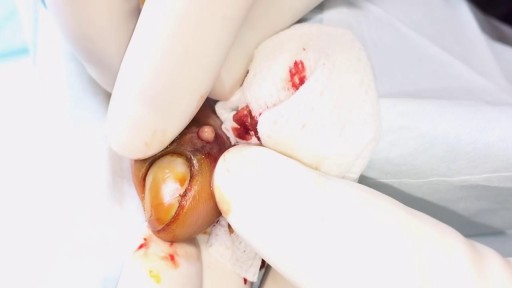
What Is an Appendectomy? An appendectomy is the surgical removal of the appendix. It’s a common emergency surgery that’s performed to treat appendicitis, an inflammatory condition of the appendix. The appendix is a small, tube-shaped pouch attached to your large intestine. It’s located in the lower right side of your abdomen. The exact purpose of the appendix isn’t known. However, it’s believed that it may help us recover from diarrhea, inflammation, and infections of the small and large intestines. These may sound like important functions, but the body can still function properly without an appendix. When the appendix becomes inflamed and swollen, bacteria can quickly multiply inside the organ and lead to the formation of pus. This buildup of bacteria and pus can cause pain around the belly button that spreads to the lower right section of the abdomen. Walking or coughing can make the pain worse. You may also experience nausea, vomiting, and diarrhea. It’s important to seek treatment right away if you’re having symptoms of appendicitis. When the condition goes untreated, the appendix can burst (perforated appendix) and release bacteria and other harmful substances into the abdominal cavity. This can be life-threatening, and will lead to a longer hospital stay. Appendectomy is the standard treatment for appendicitis. It’s crucial to remove the appendix right away, before the appendix can rupture. Once an appendectomy is performed, most people recover quickly and without complications. Why Is an Appendectomy Performed? An appendectomy is often done to remove the appendix when an infection has made it inflamed and swollen. This condition is known as appendicitis. The infection may occur when the opening of the appendix becomes clogged with bacteria and stool. This causes your appendix to become swollen and inflamed. The easiest and quickest way to treat appendicitis is to remove the appendix. Your appendix could burst if appendicitis isn’t treated immediately and effectively. If the appendix ruptures, the bacteria and fecal particles within the organ can spread into your abdomen. This may lead to a serious infection called peritonitis. You can also develop an abscess if your appendix ruptures. Both are life-threatening situations that require immediate surgery. Symptoms of appendicitis include: stomach pain that starts suddenly near the belly button and spreads to the lower right side of the abdomen abdominal swelling rigid abdominal muscles constipation or diarrhea nausea vomiting loss of appetite low-grade fever Although pain from appendicitis typically occurs in the lower right side of the abdomen, pregnant women may have pain in the upper right side of the abdomen. This is because the appendix is higher during pregnancy. Go to the emergency room immediately if you believe you have appendicitis. An appendectomy needs to be performed right away to prevent complications. What Are the Risks of an Appendectomy? An appendectomy is a fairly simple and common procedure. However, there are some risks associated with the surgery, including: bleeding infection injury to nearby organs blocked bowels It’s important to note that the risks of an appendectomy are much less severe than the risks associated with untreated appendicitis. An appendectomy needs to be done immediately to prevent abscesses and peritonitis from developing. How Do I Prepare for an Appendectomy? You’ll need to avoid eating and drinking for at least eight hours before the appendectomy. It’s also important to tell your doctor about any prescription or over-the-counter medications you’re taking. Your doctor will tell you how they should be used before and after the procedure. You should also tell your doctor if you: are pregnant or believe you may be pregnant are allergic or sensitive to latex or certain medications, such as anesthesia have a history of bleeding disorders You should also arrange for a family member or friend to drive you home after the procedure. An appendectomy is often performed using general anesthesia, which can make you drowsy and unable to drive for several hours after surgery. Once you’re at the hospital, your doctor will ask you about your medical history and perform a physical examination. During the exam, your doctor will gently push against your abdomen to pinpoint the source of your abdominal pain. Your doctor may order blood tests and imaging tests if appendicitis is caught early. However, these tests may not be performed if your doctor believes an emergency appendectomy is necessary. Before the appendectomy, you’ll be hooked up to an IV so you can receive fluids and medication. You’ll likely be put under general anesthesia, which means you’ll be asleep during surgery. In some cases, you’ll be given local anesthesia instead. A local anesthetic numbs the area, so even though you’ll be awake during the surgery, you won’t feel any pain. How Is an Appendectomy Performed? There are two types of appendectomy: open and laparoscopic. The type of surgery your doctor chooses depends on several factors, including the severity of your appendicitis and your medical history. Open Appendectomy During an open appendectomy, a surgeon makes one incision in the lower right side of your abdomen. Your appendix is removed and the wound is closed with stiches. This procedure allows your doctor to clean the abdominal cavity if your appendix has burst. Your doctor may choose an open appendectomy if your appendix has ruptured and the infection has spread to other organs. It’s also the preferred option for people who have had abdominal surgery in the past. Laparoscopic Appendectomy During a laparoscopic appendectomy, a surgeon accesses the appendix through a few small incisions in your abdomen. A small, narrow tube called a cannula will then be inserted. The cannula is used to inflate your abdomen with carbon dioxide gas. This gas allows the surgeon to see your appendix more clearly. Once the abdomen is inflated, an instrument called a laparoscope will be inserted through the incision. The laparoscope is a long, thin tube with a high-intensity light and a high-resolution camera at the front. The camera will display the images on a screen, allowing the surgeon to see inside your abdomen and guide the instruments. When the appendix is found, it will be tied off with stiches and removed. The small incisions are then cleaned, closed, and dressed. Laparoscopic surgery is usually the best option for older adults and people who are overweight. It has fewer risks than an open appendectomy procedure, and generally has a shorter recovery time. What Happens After an Appendectomy? When the appendectomy is over, you’ll be observed for several hours before you’re released from the hospital. Your vital signs, such your breathing and heart rate, will be monitored closely. Hospital staff will also check for any adverse reactions to the anesthesia or the procedure. The timing of your release will depend on: your overall physical condition the type of appendectomy performed your body’s reaction to the surgery In some cases, you may have to remain in the hospital overnight. You may be able to go home the same day as the surgery if your appendicitis wasn’t severe. A family member or friend will need to drive you home if you received general anesthesia. The effects of general anesthesia usually take several hours to wear off, so it can be unsafe to drive after the procedure. In the days following the appendectomy, you may feel moderate pain in the areas where incisions were made. Any pain or discomfort should improve within a few days. Your doctor may prescribe medication to relieve the pain. They might also prescribe antibiotics to prevent an infection after surgery. You can further reduce your risk for infection by keeping the incisions clean. You should also watch for signs of infection, which include: redness and swelling around the incision fever above 101°F chills vomiting loss of appetite stomach cramps diarrhea or constipation that lasts for more than two days Although there’s a small risk of infection, most people recover from appendicitis and an appendectomy with little difficulty. Full recovery from an appendectomy takes about four to six weeks. During this time, your doctor will probably recommend that you limit physical activity so your body can heal. You’ll need to attend a follow-up appointment with your doctor within two to three weeks after the appendectomy.
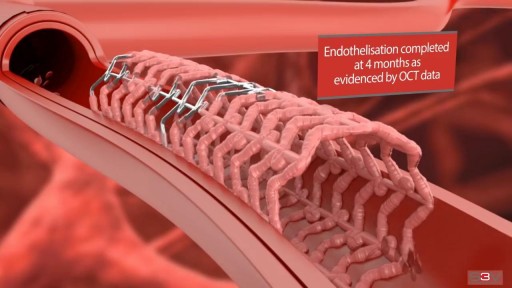
Angioplasty is a procedure to restore blood flow through the artery. You have angioplasty in a hospital. The doctor threads a thin tube through a blood vessel in the arm or groin up to the involved site in the artery. The tube has a tiny balloon on the end.

The objectives of hemodialysis are to extract toxic nitrogenous substances from the blood and to remove excess water. In hemodialysis, the blood, laden with toxins and nitrogenous wastes, is diverted from the patient to a machine, a dialyzer, in which the blood is cleansed and then returned to the patient. Diffusion, osmosis, and ultrafiltration are the principles on which hemodialysis is based.
The toxins and wastes in the blood are removed by diffusion—that is, they move from an area of higher concentration in the blood to an area of lower concentration in the dialysate. The dialysate is a solution made up of all the important electrolytes in their ideal extracellular concentrations.
The electrolyte level in the patient’s blood can be brought
under control by properly adjusting the dialysate bath. The semipermeable membrane impedes the diffusion of large molecules,
such as red blood cells and proteins.
#hemodialysis #dialysis #viral #urinaryinfection #shorts #medical #animation
*How to setup a dialysis Machine*
This is part one of two parts of *How to setup a dialysis Machine* Setting up the Fresenius 2008K hemodialysis machine.
________________________________________________________________
Additional Resources:
Technical training | Fresenius Medical Care
https://fmcna.com/faq/technical-training/
The Technical Training team Fresenius Renal Technologies, a division of ... closed room environment, as well as hands-on instruction using current machines. ... 2008® Series Troubleshooting Hemodialysis Systems – Workshop, Level II, 2.4 ...
[PDF]2008K Level I Training Manual - Fresenius Medical Care
https://fmcna.com/wp-content/u....ploads/documents/490
I 2008K TRAINING COURSE AGENDA. II HEMODIALYSIS REVIEW. III HYDRAULIC DESCRIPTION. IV MACHINE OPERATION. V INSTALLATION CHECKLIST ...
Training & education - Fresenius Medical Care
https://www.freseniusmedicalca....re.com/en/healthcare
Fresenius Medical Care — training and education for health care professionals. For patient support, home treatment, regulatory requirements, supporting guides ...
At-Home Hemodialysis Training | Fresenius Kidney Care
https://www.freseniuskidneycare.com › Treatments › At-Home Hemodialysis
Depending on the type of dialysis machine you will use, the training program lasts for about 4 to 8 weeks. You will continue to get your dialysis treatments while ...
Training with Fresenius 2008K - HD For Patients - Home Dialysis ...
forums.homedialysis.org › ... › HD For Patients
Nov 16, 2006 - 6 posts - 5 authors
Stacy and I have been in training with the Fresenius Baby K for the past 4 weeks. ... my doctor about doing home hemodialysis, so a much deserv… ... on giving you a quiet RO and makes the machine as quiet as possible.
The Dialysis Machine — Dialysis Technician's Training
https://dialysistechnicianstra....ining.com/the-dialys
The dialysis machine acts as an artificial replacement for the kidneys, ... Inc. Gambro; Fresenius Medical Care; Wilmed Global – reconditioned machines ...
Training – Renal Dynamics
https://www.renaldynamics.com › Services
Machines: • Fresenius Level I and II training • Introduction to dialysis and machines • Hands on demonstrations • Practical and written exams • Certification upon ...
2008K@home Fresenius Home Hemodialysis Machine
https://fmcna-hd.com/2008kathome.html
Back to 2008K2 Fresenius Dialysis Machine Go to 2008T Fresenius Dialysis ... Same clinical, technical training and same spare parts as 2008k machines

Demystify knee pain and discover nine of the most common causes of pain in this complex joint. Join Burke Selbst PT as we work through our simple screening for the most common types of problems.
Burke is the founder and clinical director of Focus Physical Therapy in Bend Oregon.
Find him:
https://focusptbend.com
https://facebook.com/focusphysio
Intro Song Credit
Adventures by A Himitsu https://www.youtube.com/channel/UCgFw...
Creative Commons — Attribution 3.0 Unported— CC BY 3.0
http://creativecommons.org/licenses/b...
Music released by Argofox https://youtu.be/8BXNwnxaVQE
Music provided by Audio Library https://youtu.be/MkNeIUgNPQ8

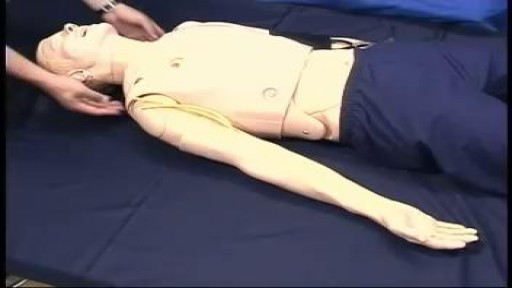
The thyroid gland lies in the midline of the anterior neck, just caudal to the thyroid cartilage. To inspect the thyroid gland, the examiner stands in front of the patient. The examiner asks the seated patient to dorsiflex (extend) the neck and swallow a sip of water. Minor enlargement of the gland may only become apparent on inspection in this position. Palpation of the thyroid gland is typically performed with the examiner standing behind the patient. Both lobes and the isthmus of the thyroid gland should be palpated for any nodules or diffuse enlargement. Mobility of the thyroid gland with swallowing should be assessed with palpation. Nodules arising from the thyroid gland typically move with swallowing. A hard, fixed thyroid gland could indicate malignancy. If a central nodule is identified, the patient is asked to protrude the tongue. Upward movement of the central nodule on protrusion of the tongue indicates a thyroglossal cyst. Auscultation is performed at the superior poles of bilateral lobes as this is where the superior thyroid artery is most superficial and bifurcates into its terminal branches. A bilateral bruit over the superior poles suggests Graves disease. Examination of the thyroid gland is completed by palpating the regional cervical lymph nodes for any enlargement.
Subscribe to AMBOSS YouTube for the latest clinical examination videos, medical student interviews, study tips and tricks, and live webinars!
Free 5 Day Trial: https://go.amboss.com/amboss-YT
Instagram: https://www.instagram.com/amboss_med/
Facebook: https://www.facebook.com/AMBOSS.Med/
Twitter: https://twitter.com/ambossmed
Blog: https://blog.amboss.com/us
#AMBOSSMed #ClinicalExamination #USMLE

Elbow Exam - Orthopaedic OSCE - Clinical Skills - Dr Gill
The elbow examination is a core skill - in this video, we demonstrate how to perform an elbow EXAM for an Orthopaedic Clinical Skills OSCE, which should be one of the more accessible examination stations for medical students.
For a passing grade in your Clinical Skills OSCE, an elbow assessment should follow the LOOK, FEEL, MOVE approach
Initially looking for erythema, scars, swelling and position
Palpating the elbow - specifically the olecranon, medial and lateral epicondyles, and radial head for heat, oedema and crepitus
Finally assess range of movement with flexion and extension at the elbow, before determining for tennis and golfers' elbows
Watch further orthopaedic examinations for your OSCE revision:
The Elbow - Deep Dive
https://youtu.be/SX5buhtCVDw
The Spine Examination:
https://youtu.be/pJxMHa6SCgU
The Knee examination
https://youtu.be/oyKH4EYfJDM
The Hip examination
https://youtu.be/JC9GKq5nSdQ
The GALS examination
https://youtu.be/5qJaf7gW-B0 - Gait, Arms, Legs, Spine - GALS screen
------------
Please note that there is no ABSOLUTE way to perform a clinical examination. Different institutions and even clinicians will have differing degrees of variations - the aim is the effectively identify medically relevant signs.
However during OSCE assessments. Different medical schools, nursing colleges and other health professional courses will have their own preferred approach to a clinical assessment - you should concentrate on THEIR marks schemes for your assessments.
The examination demonstrated here is derived from Macleods Clinical Examination - a recognised standard textbook for clinical skills.
Some people viewing this medical examination video may experience an ASMR effect
#clinicalskills #Elbow #DrGill