Top videos

Learn Basic Laparoscopic Surgery, the components of a laparoscopic surgical setup, optimal positioning and ergonomics in laparoscopic surgery, and much more. Check out the full course for free here: https://www.incision.care/free-trial
What is Laparoscopic Surgery:
Laparoscopic surgery describes procedures performed using one or multiple small incisions in the abdominal wall in contrast to the larger, normally singular incision of laparotomy. The technique is based around principles of minimally invasive surgery (or minimal access surgery): a large group of modern surgical procedures carried out by entering the body with the smallest possible damage to tissues. In abdominopelvic surgery, minimally invasive surgery is generally treated as synonymous with laparoscopic surgery as are procedures not technically within the peritoneal cavity, such as totally extraperitoneal hernia repair, or extending beyond the abdomen, such as thoraco-laparoscopic esophagectomy. The term laparoscopy is sometimes used interchangeably, although this is often reserved to describe a visual examination of the peritoneal cavity or the purely scopic component of a laparoscopic procedure. The colloquial keyhole surgery is common in non-medical usage.
Surgical Objective of Laparoscopic Surgery:
The objective of a laparoscopic approach is to minimize surgical trauma when operating on abdominal or pelvic structures. When correctly indicated and performed, this can result in smaller scars, reduced postoperative morbidity, shorter inpatient durations, and a faster return to normal activity. For a number of abdominopelvic procedures, a laparoscopic approach is now generally considered to be the gold-standard treatment option.
Definitions
Developments of Laparoscopic Surgery:
Following a number of smaller-scale applications of minimally invasive techniques to abdominopelvic surgery, laparoscopic surgery became a major part of general surgical practice with the introduction of laparoscopic cholecystectomy in the 1980s and the subsequent pioneering of endoscopic camera technology. This led to the widespread adoption of the technique by the early- to mid-1990s. The portfolio of procedures that can be performed laparoscopically has rapidly expanded with improvements in instruments, imaging, techniques and training — forming a central component of modern surgical practice and cross-specialty curricula [2]. Techniques such as laparoscopically assisted surgery and hand-assisted laparoscopic surgery have allowed the application of laparoscopic techniques to a greater variety of pathology. Single-incision laparoscopic surgery, natural orifice transluminal endoscopic surgery, and minilaparoscopy-assisted natural orifice surgery continue to push forward the applications of minimally invasive abdominopelvic techniques; however, the widespread practice and specific indications for these remain to be fully established. More recently, robotic surgery has been able to build on laparoscopic principles through developments in visualization, ergonomics, and instrumentation.
This Basic Laparoscopic Surgery Course Will Teach You:
- Abdominal access techniques and the different ways of establishing a pneumoperitoneum
- Principles of port placement and organization of the operative field
- Key elements of laparoscopic suturing, basic knotting and clip application
Specific attention is paid to the following hazards you may encounter:
- Fire hazard and thermal injury
- Lens fogging
- Contamination of insufflation system
- Complications from trocar introduction
- Limitations of Veress needle technique
- Limitations of open introduction technique
- Complications of the pneumoperitoneum
- Gas embolism
- Mirroring and scaling of instrument movements
- Firing clip applier without a loaded clip
The following tips are designed to improve your understanding and performance:
- Anatomy of a laparoscope
- Checking for optic fiber damage
- "White balance" of camera
- Checking integrity of electrosurgical insulation
- Access at Palmer's point
- Lifting abdominal wall before introduction
- Confirming position of Veress needle
- Umbilical anatomy
- Identification of inferior epigastric vessels under direct vision
- Translumination of superficial epigastric vessels
- Selection of trocar size
- Aiming of trocar
- Working angles in laparoscopic surgery
- Choice of suture material
- Instruments for suturing
- Optimal ergonomics for suturing
- Extracorporeal needle positioning
- Optimal suture lengths
- "Backloading" needle
- Intracorporeal needle positioning
- Hand movements when suturing
- Optimal positioning of scissors
- Extracorporeal knot tying
- Visualization of clip applier around target structure
- Common clip configurations
Ettore Vulcano, MD, Foot and Ankle Orthopedic Surgeon at Mount Sinai West, discusses a new minimally invasive bunion surgery that has patients walking immediately after surgery, and getting back to an active lifestyle much quicker than with the traditional surgery.

http://www.amerra.com In this patient education video from Colorectal Surgical Associates in Houston, Texas, learn more about the single incision laparoscopic colectomy procedure. This minimally invasive procedure uses a mini incision that
results in less pain, fewer complications, earlier recovery, and a smaller scar. Colorectal cancer is the second leading cause of cancer death in the United States. For more information please visit our website: www.csamd.com or call (713)-790-0600.

Mini-Laparoscopic Cholecystectomy with Intraoperative Cholangiogram for Symptomatic Cholelithiasis (Gallstones) - Standard
Authors: Brunt LM1, Singh R1, Yee A2
Published: September 26, 2017
AUTHOR INFORMATION
1 Department of Surgery, Washington University, St. Louis, Missouri
2 Division of Plastic and Reconstructive Surgery, Washington University, St. Louis, Missouri
DISCLOSURE
No authors have a financial interest in any of the products, devices, or drugs mentioned in this production or publication.
ABSTRACT
Minimal invasive laparoscopic cholecystectomy is the typical surgical treatment for cholelithiasis (gallstones), where patients present with a history of upper abdominal pain and episodes of biliary colic. The classic technique for minimal invasive laparoscopic cholecystectomy involves four ports: one umbilicus port, two subcostal ports, and a single epigastric port. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has instituted a six-step strategy to foster a universal culture of safety for cholecystectomy and minimize risk of bile duct injury. The technical steps are documented within the context of the surgical video for (1) achieving a critical view of safety for identification of the cystic duct and artery, (2) intraoperative time-out prior to management of the ductal structures, (3) recognizing the zone of significant risk of injury, and (4) routine intraoperative cholangiography for imaging of the biliary tree. In this case, the patient presented with symptomatic biliary colic due to a gallstone seen on the ultrasound in the gallbladder. The patient was managed a mini-laparoscopic cholecystectomy using 3mm ports for the epigastric and subcostal port sites with intraoperative fluoroscopic cholangiogram. Specifically, the senior author encountered a tight cystic duct preventing the insertion of the cholangiocatheter and the surgical video describes how the author managed the cystic duct for achieving a cholangiogram, in addition to the entire technical details of laparoscopic cholecystectomy.

"Laparoscopic Placement of a
Peritoneal Dialysis Catheter"
Houston Methodist DeBakey Heart & Vascular Center, presents a cardiovascular procedure featuring Eric K. Peden, MD, Shri Timbalia, MD, and Kenneth Livingston as they demonstrate “Laparoscopic Placement of a
Peritoneal Dialysis Catheter".
Surgery: Eric K. Peden, MD, Shri Timbalia, MD, and Kenneth Livingston
Narration: Kenneth Livingston
** This medical education program may contain graphic content. **
_________________________________
A DeBakey CV Education event
Presented by Houston Methodist DeBakey Heart & Vascular Center.
Building on Dr. Michael E. DeBakey’s commitment to excellence in education, Houston Methodist DeBakey CV Education is an epicenter for cardiovascular academic and clinical educational programs that support the provision of optimal care to patients suffering from cardiovascular conditions and diseases.
FOR MORE INFORMATION
DeBakey CV Education:
https://www.houstonmethodist.o....rg/education/medical
For the latest education and training opportunities from DeBakey CV Education: http://bit.ly/HMdebakeyemail
Follow Us:
Facebook: https://www.facebook.com/debakeycvedu
Twitter: https://twitter.com/DeBakeyCVedu
Livestream: https://livestream.com/debakey
SmugMug: https://debakey.smugmug.com/
Want concise, relevant reviews of the hottest topics in CV medicine? Subscribe for FREE to the Methodist DeBakey Cardiovascular Journal for quarterly, peer-reviewed issues delivered to your door.
https://journal.houstonmethodist.org/

Laparoscopic surgery is minimally-invasive (keyhole) surgery and it is performed through very small incisions, using a camera to guide the surgeon during the procedure. Miss Sarah Mills, a top colorectal surgeon, explains why laparoscopic surgery is performed over alternative methods.
Make an appointment with Miss Sarah Mills here: https://www.topdoctors.co.uk/doctor/sarah-mills

Pediatric surgeons at Texas Children’s Hospital West Campus perform general surgical procedures such as circumcisions, removal of foreign objects, hernia repair, and suturing of minor lacerations. While more complex surgeries take place at the Texas Children’s Main Campus, pre-operative and follow-up outpatient care for those procedures is available at the West Campus.
Everything about Texas Children’s Hospital West Campus is dedicated to the health and wellness of children. As greater Houston's first suburban hospital designed exclusively for children, we offer the expert care you've come to trust from Texas Children's Hospital coupled with a location that's convenient and accessible for area families. Our facility is located just off the westbound feeder road of the Katy Freeway (at I-10 and Barker Cypress).
For more information about Texas Children's Hospital West Campus, visit http://www.texaschildrens.org/....Locate/In-the-Commun
Meet Dr. Allen Milewicz, chief of community surgery at Texas Children's West Campus
https://www.youtube.com/watch?v=uMoCdipuKfA&index=16&list=PLiN68C9rloPBD-E9ChWhVy73h7V3SEMlm

Johns Hopkins Children’s Center Surgeon-in-Chief David Hackam provides information about general pediatric surgery and when it is time to see a general pediatric surgeon. #PediatricSurgery #JohnsHopkins
For more information on general pediatric surgery at Johns Hopkins Children's Center, visit https://www.hopkinsmedicine.or....g/johns-hopkins-chil
FAQ's
0:02 What is a general pediatric surgeon?
0:31 When is it time to see a pediatric surgeon?
1:02 What are some of the most common surgical problems seen by general pediatric surgeons?
1:43 Describe research being done in the field.
2:15 Why choose Johns Hopkins Children's Center for general pediatric surgery?

Having surgery can be frightening for anyone, but it's especially scary for kids who don't always understand what's going on, or what the grown-ups are saying. We're here to help!
Join Avrie, who had surgery at the Sacred Heart Children's Hospital pediatric surgery center in Spokane, WA. Maybe after watching and hearing her story, you and your kiddo will feel better about having surgery in the hospital.
Follow Avrie's trip - from check-in, vital signs and pre-op checks; meeting the doctor who will do his surgery, along with the anesthesiologist, surgery nurse and the Child Life Specialist; the trip to the Operating Room; waking up in the recovery room with his mom by his side; and getting ready to go home.
To learn more about the pediatric surgery center at Sacred Heart Children's Hospital, visit https://washington.providence.....org/locations-direct

Mr Brian MacCormack talking about Paediatric Surgery Emergencies. This talk is part of the Paediatric Emergencies 2022 event. To get your CME certificate for watching the video please visit https://www.paediatricemergenc....ies.com/conference/p
#PaediatricEmergencies #PaediatricEmergencies2022 #PaediatricSurgery

Children are special patients, and their medical needs are unique, including their surgical needs. At UNC Hospitals, an expert and experienced team of physicians treat children in a kid-friendly and family-centered environment. UNC Pediatric Surgeon Dr. Timothy Weiner explains

As a pediatric surgeon at NewYork-Presbyterian/Weill Cornell Medical Center, Dr. Nitsana Spigland treats newborns, children, teens, and young adults requiring surgical interventions. She specializes in antenatal counseling and newborn congenital malformations.
Learn more about Dr. Spigland at: https://www.nyp.org/physician/nspigland.

Must Watch Very Special New Funny Video 2023 Doctor Funny Video Injection Wala Funny Video | Comedy Video Episode 124 By Fun Comedy Ltd
@funcomedyltd
#funcomedyltd
#doctor
#comedy
#wala
Hello Dear Viewers,
If We have any mistake. please comment and tell us, what is our mistake? We will try to solve this mistake next. please watch our videos and give us confidence to trying best. Thank you for watching this video.
IMPORTANT NOTE:-
This video are no any kind of risk. This video are totally acting no risk no Dangerous act no Physical Harm or Death its ok for viewers.
injection wala comedy video injection wala video injection funny video injection injection wala injection injection doctor doctor doctor sui wala wala suji wala suji wala cartoon doctor cartoon funny video tui tui injection cartoon 22 cartoon video injection video cartoon cartoon comedy video doctor video wala cartoon busy fun ltd my family our fun tv fun tv 24 fun tv 420 funny day funny family ding dong bidik fun tv roma fun tv
#cartoon
#comedyvideo
#doctor_doctor
#busyfunltd
#newfunnyvideo2022
#newfunniestcomedy
#injectionfunnyvideo
#sui_wala
#myfamily
#busyfunltd
#funnyday
#bidikfuntv
#mohafuntv
#dingdong

This multi award winning video talks about a time of increased demands on our healthcare system and healthcare providers, ensuring that each and every patient and their family members are provided with compassionate care is a massive goal, but one that the staff at the Royal Alexandra Hospital are pursuing every day. Good quality care is always important, but caring for our patients is what they will really remember.

Ellis and Cathy demonstrate how to administer blood to a patient.
Our Critical Nursing Skills video tutorial series is taught by Ellis Parker MSN, RN-BC, CNE, CHS and intended to help RN and PN nursing students study for your nursing school exams, including the ATI, HESI and NCLEX.
#NCLEX #ClinicalSkills #Blood #bloodtransfusion #HESI #Kaplan #ATI #NursingSchool #NursingStudent #Nurse #RN #PN #Education #LVN #LPN
00:00 What to expect blood transfusion
00:26 First steps for a blood transfusion
1:03 Priming the tubing for blood transfusion
2:29 Confirming the blood for transfusion
4:36 Hanging the blood for transfusion
5:06 Clamping a Y-tube
5:34 Priming the blood for transfusion
7:00 Responding to a blood transfusion reaction
🚨 Reminder: shipping deadlines are looming 👀
🎁 Regular Shipping: Order by Friday, December 15
🚀 Expedited Shipping: Order by Monday, December 18
🔍 Still searching for last-minute gifts? Consider a Level Up RN Gift Card! 💌 It’s not only a thoughtful present but also the perfect way to share treasures like Pharmacology Flashcards OR digital treasures like Flashables Digital Nursing Flashcards & the Level Up RN membership. Give the gift of knowledge this holiday season! 🧠⚡️💖 bit.ly/LevelUpRNGC
🚪 Access our Cram Courses, Quizzes and Videos all in one ad free space with Level Up RN Membership https://bit.ly/LevelUpRNMembership
Want more ways to MASTER Clinical Skills? Check out our flashcards & videos!
👇👇👇👇👇👇👇👇👇👇
👉 https://bit.ly/clinicalnursingskills 👈
☝️👆☝️👆☝️👆☝️👆☝️👆
This is your one-stop-shop for materials to help you LEARN & REVIEW so you can PASS Nursing School.
🤔🤔🤔 DO YOU WANT TO PASS your classes, proctored exams and the NCLEX? 🤔🤔🤔 Our resources are the best you can buy. They are built with a single goal: help you pass with no fluff. Everything you need, and nothing you don’t. Don’t take our word for it, though! Check out our hundreds of ⭐️⭐️⭐️⭐️⭐️ reviews from nurses who passed their exams and the NCLEX with Level Up RN.
🗂️ Our Ultimate Nursing School Survival kit is your number 1 resource to get through nursing school and to pass the NCLEX. Whether you're just starting school or you’re already prepping for the NCLEX, this bundle of flashcards is the best you can buy. It covers all the information you need to know to pass all your exams and it has FREE shipping!
➡️ https://bit.ly/TUNSSK ⬅️
L👀king for EVEN MORE resources to survive Nursing School? Make your Nursing School experience your own! Life’s difficult enough—learning shouldn’t be.
🪅 Games https://nursesquad.com
💻 Digital resources https://bit.ly/NursingStudyCourses
📅 Organizational tools https://bit.ly/OrganizingSchool
✨Want perks? Join our channel!
https://youtube.com/leveluprn/join
🏷 Head to https://leveluprn.com/specials for all our latest deals!🥳️
📧 LOOKING FOR FREE RESOURCES TO HELP WITH YOUR EXAMS? Get exclusive tips, latest video releases and more delivered to your email!
➡️ https://leveluprn.com/signup ⬅️
⚕ 👩 LEVEL UP NURSE SQUAD 👩⚕️
All of the nurses at Level Up RN are here to help! Cathy Parkes started helping her fellow classmates back when she was in nursing school, tutoring so they could pass their exams and graduate. After she got her BSN and started working as an RN at Scripps Encinitas Hospital, she started this YouTube channel to help nursing students around the world. Since then she has built a team of top-notch dedicated nurses and nurse educators who are focused on improving nursing education and supporting career advancement for nurses everywhere. With flashcards, videos, courses, organizational tools and more, we are singularly focused on helping students and nurses Level Up on their exams and nursing careers.
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full lesson on IM Injections here:
https://nursing.com/lesson/ski....lls-06-01-pill-crush
Check out our new Nurse Care Plan Lessons here:
https://bit.ly/3BPRfPL
Get Access to Thousands of Lessons here:
https://nursing.com/courses/
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
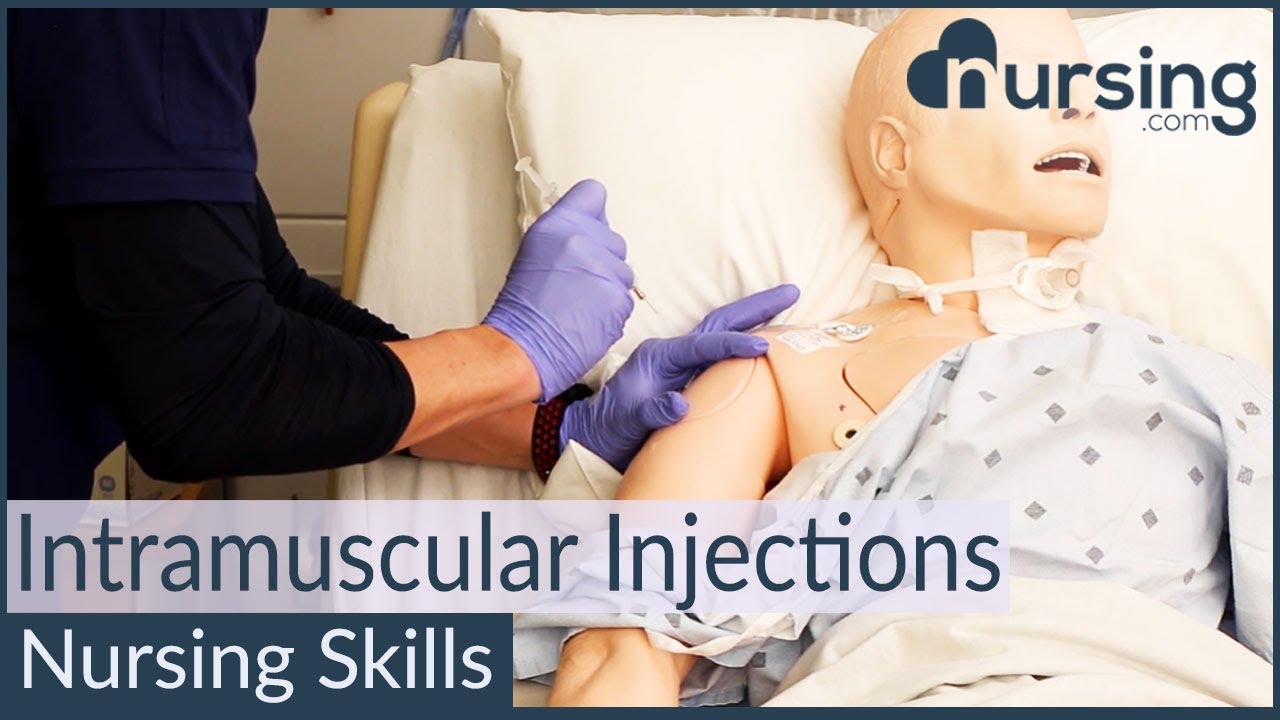
Intramuscular Injection Techniques (Nursing Skills)
In this video, we’re going to look at proper administration techniques for intramuscular medication administration. Of course, always follow your 5 rights and calculate the correct volume for administration. We love you guys! Go out and be your best selves today! And, as always, happy nursing!
Bookmarks:
0.05 Introduction to Intramuscular injections
0.16 site and needle selection
0.35 site sterilization
0.43 Z track method
0.58 needle insertion
1.10 medication injection
1.14 needle removal
1.25 bandaging and needle disposal
1.30 documentation and patient monitoring
1.35 Outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.

Hand hygiene for healthcare workers: Learn how to perform hand washing with soap and water (nursing procedures).
There are two ways to perform hand hygiene as a nurse. You can use soap and water or an alcohol-based hand rub (also called hand sanitizer or hand gel).
Hand hygiene is essential for providing safe patient care. If hand hygiene is not performed regularly, germs can be easily be spread to patients, other healthcare workers, and even yourself.
Hand hygiene is ALWAYS performed before and after patient care, after coming into contact with any type of body fluid or open wounds, when touching any object that is near a patient (hand railing, bedside table etc.), removing gloves, prior to eating, or after using the bathroom.
This video discusses when you should use soap and water versus an alcohol-based hand gel, when to perform hand hygiene, and demonstrates how to perform hand hygiene using soap and water.
Notes: https://www.registerednursern.....com/how-to-perform-h
More nursing skills: https://www.youtube.com/watch?v=DBHnd3N-5Ns&list=PLQrdx7rRsKfUhd_qQYEbp0Eab3uUKhgKb
Facebook: https://www.facebook.com/RegisteredNurseRNs
Instagram: https://www.instagram.com/registerednursern_com/
Twitter: https://twitter.com/NursesRN
#handhygiene #handwashing #nursingskills
Subscribe: http://www.youtube.com/subscri....ption_center?add_use
Nursing School Supplies: https://www.registerednursern.....com/the-ultimate-lis
Popular Playlists:
NCLEX Reviews: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Fluid & Electrolytes: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing Skills: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing School Study Tips: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing School Tips & Questions" https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Teaching Tutorials: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Types of Nursing Specialties: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Healthcare Salary Information: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
New Nurse Tips: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Nursing Career Help: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
EKG Teaching Tutorials: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Dosage & Calculations for Nurses: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf
Diabetes Health Managment: https://www.youtube.com/playli....st?list=PLQrdx7rRsKf

http://www.utexas.edu
Nursing students practice their skills on mannequins and each other in the Nursing Skills Lab.



