Top videos
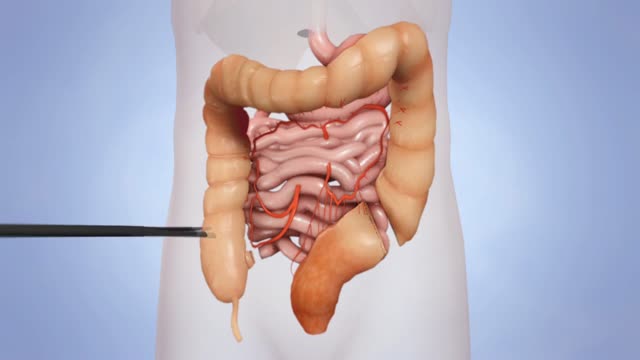
When the colon and rectum are removed (due to ulcerative colitis or familial adenomatous polyposis), another reservoir must be created for bowel contents (stool) to exit the body. Surgically creating a “J” shaped reservoir (called a J-pouch) is an option for selected patients to store and pass stool.

“Complete cure from groin hernia is now possible with Dr.Desarda's repair technique.......” Mesh is a foreign body. Therefore, its use in hernia repairs is known to cause all sorts of complications like pain, recurrence, infection etc. We have developed an innovative new technique of inguinal hernia repair without mesh. It uses your own body muscle for repair and gives virtually complete cure from inguinal hernia problem. An undetached strip of the external oblique aponeurosis is stitched on the weak area between the muscle arch and the inguinal ligament to form a new, strong and physiologically dynamic posterior wall that gives protection and prevents re-herniation. Normally patient goes home in a day after surgery and can drive car and go to office in 3-4 days time. This "Dr.Desarda's hernia repair" is now followed in many countries all over the world. We are surprised to see the enquiries from many patients in the developed countries asking for this repair in their country. This is because this operation does not use any foreign body like mesh for repair and therefore there are no complications that are seen in mesh repairs. A visit to Topix or other hernia forums show thousands of posts showing sufferings of many patients due to mesh repairs. But still why surgeons from developed countries are interested in mesh repairs is a big question for us. Please visit our website for more details: http://herniasurgery.tripod.com Our cell number: +91 9373322178

The da Vinci® Surgical System provides surgeons with an alternative to both traditional open surgery and conventional laparoscopy, putting a surgeon's hands at the controls of a state-of-the-art robotic platform. Our surgeons can perform even the most complex and delicate procedures through very small incisions with unmatched precision.

Amniocentesis,before the actual procedure, a local anesthetic is sometimes given to relieve the pain when inserting the needle used to withdraw the fluid. A needle is usually inserted through the mother's abdominal wall or at the end of the vagina, and through the wall of the uterus into the amniotic sac. With assistance from ultrasound, a physician aims towards an area of the sac that is away from the fetus and extracts a small amount of amniotic fluid for testing. The puncture heals, and the amniotic sac replenishes the liquid over a day or so. After the amniotic fluid is extracted, the fetal cells are separated from it using a centrifuge, and the fetal chromosomes are examined for abnormalities. Various genetic testing may be performed, but the three most common abnormalities tested for are Down's syndrome, Trisomy 18 and spina bifida. Amniocentesis can be performed as soon as sufficient amniotic fluid surrounds the fetus to allow a sample to be recovered relatively safely, usually no earlier than the 14th week of pregnancy. Often, genetic counseling is offered in conjunction with amniocentesis.
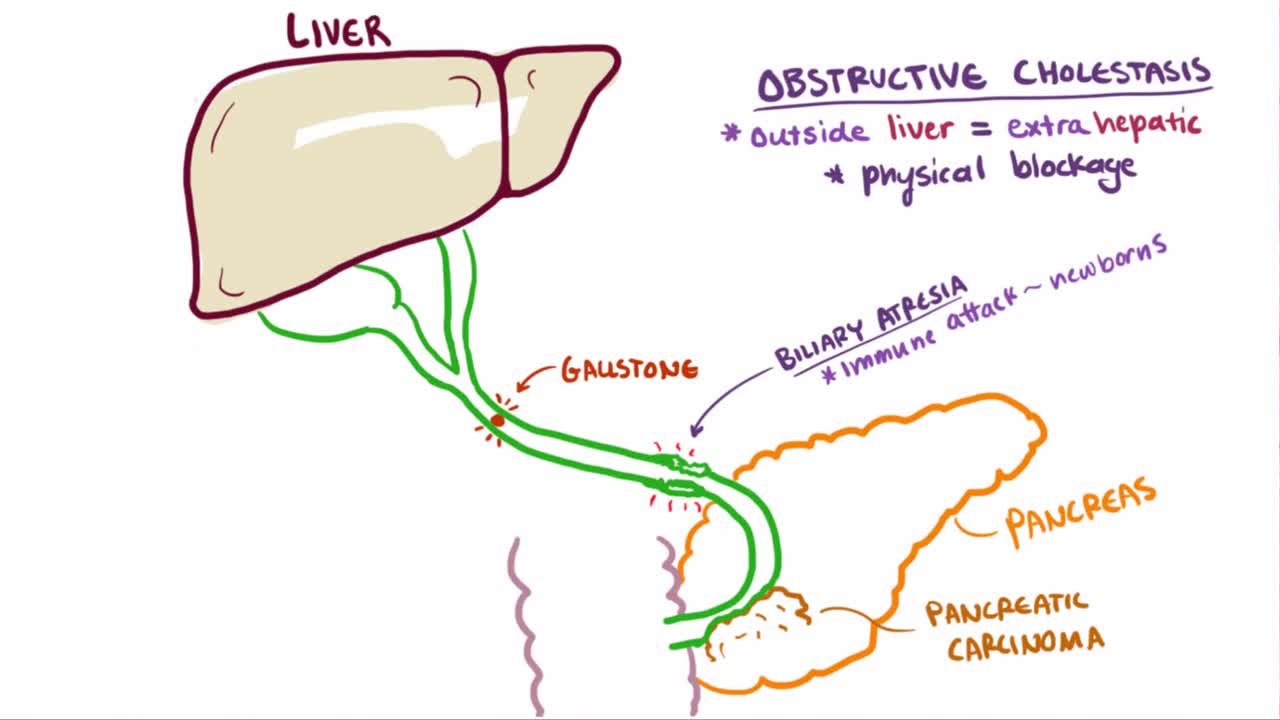
Cholestatic liver disease is a condition that results from an impairment of bile formation or bile flow to the gallbladder and duodenum (first section of the small intestine). ... The effects of cholestasis are profound and widespread, leading to worsening liver disease and systemic illness.
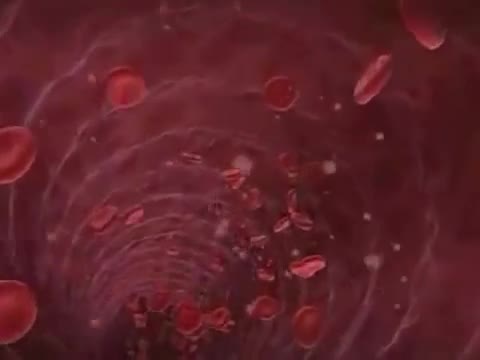
Sickle cell anemia (sickle cell disease) is a disorder of the blood caused by an inherited abnormal hemoglobin (the oxygen-carrying protein within the red blood cells). The abnormal hemoglobin causes distorted (sickled) red blood cells.
LIZ: The first time the doctor made my tip too narrow and I didnt look like myself. The second time the doctor made my tip too wide, and actually took out (removed) extra bone from the side of my nose. That didnt need to be taken out (removed)
My initial consultation with Dr. Nassif was fantastic! He treated me liker his own daughter, and was very caring and thorough. He went over everything!
DR. NASSIF: Liz came into me for a revision rhinoplasty. She told me that shes had two previous rhinoplasties. She was unhappy with the way her nose appeared on her face. She felt it was asymmetric, the tip was kind of bulbous, or large appearing, especially when she looked up, this view, it was very asymmetric. And so, her whole goal was to make it look better, hopefully make it her LAST surgery, and also to help with her breathing.
One of the things thats very important about revision rhinoplasty that you always have to consider is; What are you going to find in there? Even though you can feel the nose, you can palpate it, you can look at it, and you can guess what the other doctors have performed; your first up-hill battle is to see how much scar tissue youre going to be able to identify with. So when you have to open up the nose, you have to remove the scar tissue, identify it: whats there, whats present, whats been removed. Then after you do that, and you have cartilage now ready for grafting, or fascia, or perichondrium, you have to start rebuilding it. Rebuilding it (cartilage) is the second big stage after weve already carved everything; weve carved the cartilage. In that scenario when Im playing with the nose, in regards to staring at the profile, staring at the front of the nose, I go back and forth and look inside and outside of the nose to make sure its as symmetric as possible. That takes a long time One of Lizs main complaints was that on her profile, that her tip stuck out too far. And so one of the things I had to do in surgery is called a medial cura tuck-up, I had to push the tip back, by pushing the tip back, it can make the tip look a little bit wider. But in this situation, I was able to bring everything in as much as I can. After Im finished with everything, and Im happy, then we go ahead and we start to close the nose. Thats putting every little small stitch in perfectly, so that the scar will be minimally visible.

Surgery to treat men with prostate cancer is often followed by months of difficulty controlling urine flow, a condition known as urinary incontinence. But new research suggests that this problem may go away more quickly if the men perform certain exercises to strengthen their pelvic floor muscles.
Researchers from the Kaiser Permanente Medical Center in Los Angeles, California, found that men who were taught how to perform pelvic floor exercises before and after surgery were more likely to have regained continence three months later.
Men Doing Pelvic Exercises Recover Earlier
In the current study, the researchers randomly assigned 38 men scheduled for radical prostatectomy to either a treatment group or a control group. The men in the treatment group were referred to a physical therapist. They were instructed how to do Pelvic Floor Exercises both before and after surgery, using biofeedback to ensure they were using the proper muscles. The control group did not receive any formal instruction. All of the men completed questionnaires regarding bladder function at regular intervals over the next year.
Overall, 82% of the patients had regained continence (defined as not needing to use any absorbent pads) by the end of the year, including about equal numbers in both groups. But on average the men who had been educated about Pelvic exercises regained continence about one month earlier than those in the control group (at 12 weeks vs. 16 weeks).
Most of the men who did not regain continence within a year were still using at least three absorbent pads a day, indicating continued severe incontinence. The study authors explained that these men probably had extensive damage to the bladder sphincter or severe dysfunction of the bladder after surgery, and the exercises alone were unable to compensate for this.
But the exercises seemed to be effective. Pelvic floor exercise and education initiated prior to surgery is an effective noninvasive intervention useful for improving early return of urinary continence, the authors concluded. It would certainly have a positive impact on our patients undergoing radical prostatectomy in an effort to improve quality of life after major urological surgery.
The results of the study were published in the Journal of Urology (Vol. 170, No. 1: 130-133)