Top videos

Three to five years after gastric bypass surgery, some patients start to regain weight because the size of their stoma (the opening at the bottom of the stomach pouch) or their stomach pouch itself has increased. This can keep you from feeling full after small meals.
To resolve this problem, our surgeons use new surgical tools to create and suture folds into the pouch, reducing its volume and at the stoma to decrease its diameter. The surgeon performs the procedure entirely through the mouth -- inserting an endoscope under heavy sedation -- so there are no external incisions into the body.

SSFTV is the official YouTube channel of the Seattle Science Foundation. Subscribe now to be updated on the latest videos: tinyurl.com/yt8kt8mg.
The Seattle Science Foundation is a not for profit organization dedicated to advancing the quality of patient care through education, research, innovation and technology. As a physician driven organization, we have created a trusted community of nationally recognized experts from the world’s best medical and academic institutions.
To join our upcoming meeting for CME credit, visit https://www.ssfcme.org.
Get Social With SSF:
On Instagram: https://www.instagram.com/seattlesciencefoundation
On Facebook: https://www.facebook.com/SeattleScienceFoundation
On Twitter: https://twitter.com/seattlescifdtn
On LinkedIn: https://www.linkedin.com/company/756824
On YouTube: http://www.ssfyoutube.org
Learn More at http://www.seattlesciencefoundation.org
Dr. Rod J. Oskouian, is a neurosurgeon who specializes in the diagnosis and treatment of complex spinal disorders. Dr. Oskouian is currently the Chief of Spine at the Swedish Neuroscience Institute and President and CEO of the Seattle Science Foundation. His research and clinical focus is on scoliosis, spinal deformities and anomalies, osteoporosis, spinal cord injury, degenerative disc disease, spinal oncology, stereotactic spinal radiosurgery, and minimally invasive spinal surgery. He has published in numerous medical journals and textbooks, including Neuroscience, Neurosurgery, Neurosurgical Clinics of North America, the Journal of Neurosurgery, Neurosurgical Focus and Spine.
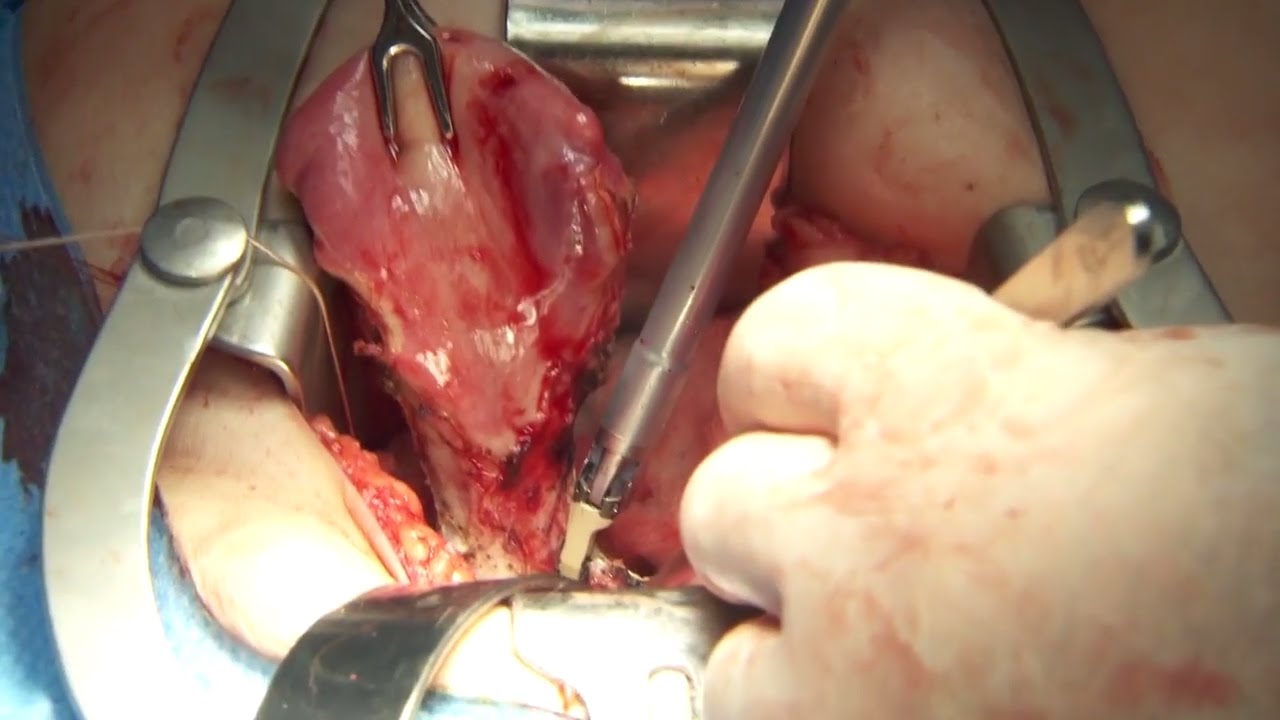
Olympus has extended the value of its award-winning combined surgical energy device, THUNDERBEAT, to open surgical procedures. Watch Dr. Francois Blaudeau master use of THUNDERBEAT Open Extended Jaw (OEJ) in a total abdominal hysterectomy.
http://medical.olympusamerica.com/products/thunderbeat?utm_source=youtube&utm_campaign=Total%20Abdominal%20Hysterectomy%20Surgery%20-%20THUNDERBEAT&utm_medium=description&utm_term=energy&utm_content=surgical
Subscribe and 🔔 to the BBC 👉 https://bit.ly/BBCYouTubeSub
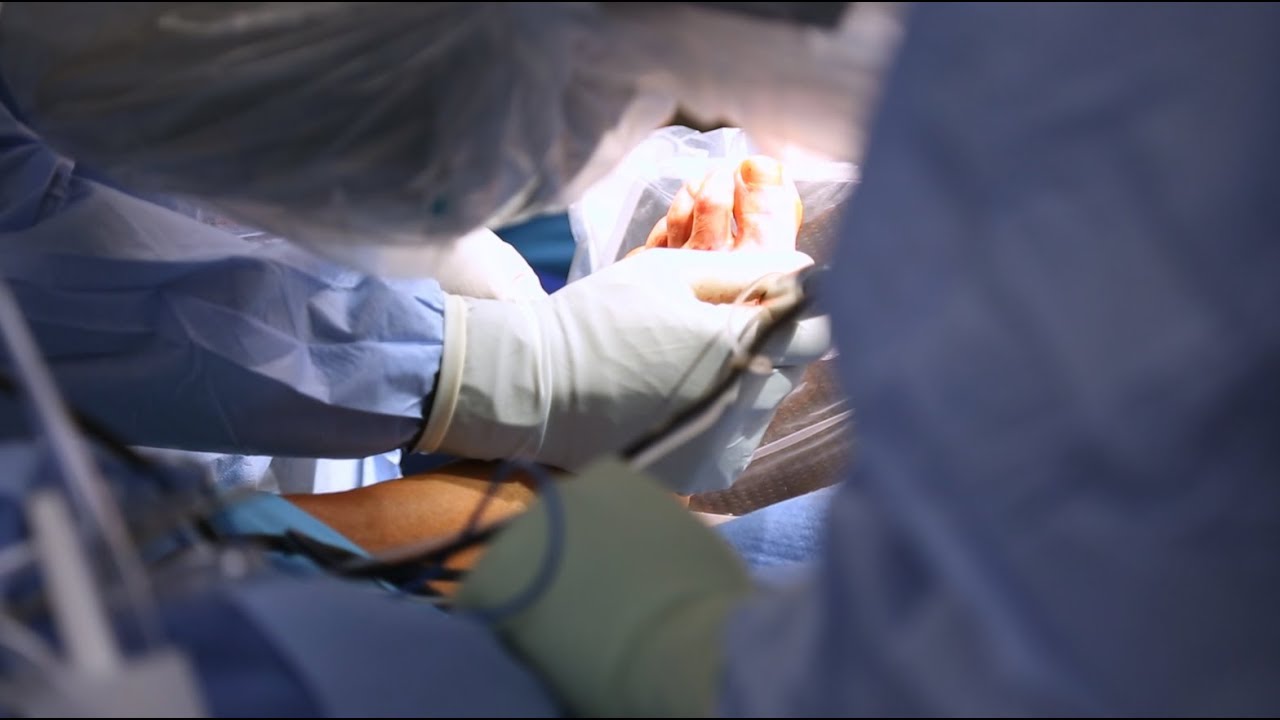
Watch the BBC first on iPlayer 👉 https://bbc.in/iPlayer-Home http://www.bbc.co.uk/human Richard Edwards undergoes a double hand transplant in which his hands are amputated and replaced with hands from a donor. This is the first time this has been done. Three months later the new hands are already changing his life.
#bbc
All our TV channels and S4C are available to watch live through BBC iPlayer, although some programmes may not be available to stream online due to rights. If you would like to read more on what types of programmes are available to watch live, check the 'Are all programmes that are broadcast available on BBC iPlayer?' FAQ 👉 https://bbc.in/2m8ks6v.

Gastric bypass, also called Roux-en-Y gastric bypass surgery, is considered a “metabolic” procedure because it changes how your body absorbs fat, calories and nutrients. This metabolic change occurs because your gastrointestinal tract is altered when your gastric bypass surgeon attaches the smaller section of your stomach directly to your small intestine. As a result, your appetite changes and you feel full faster.
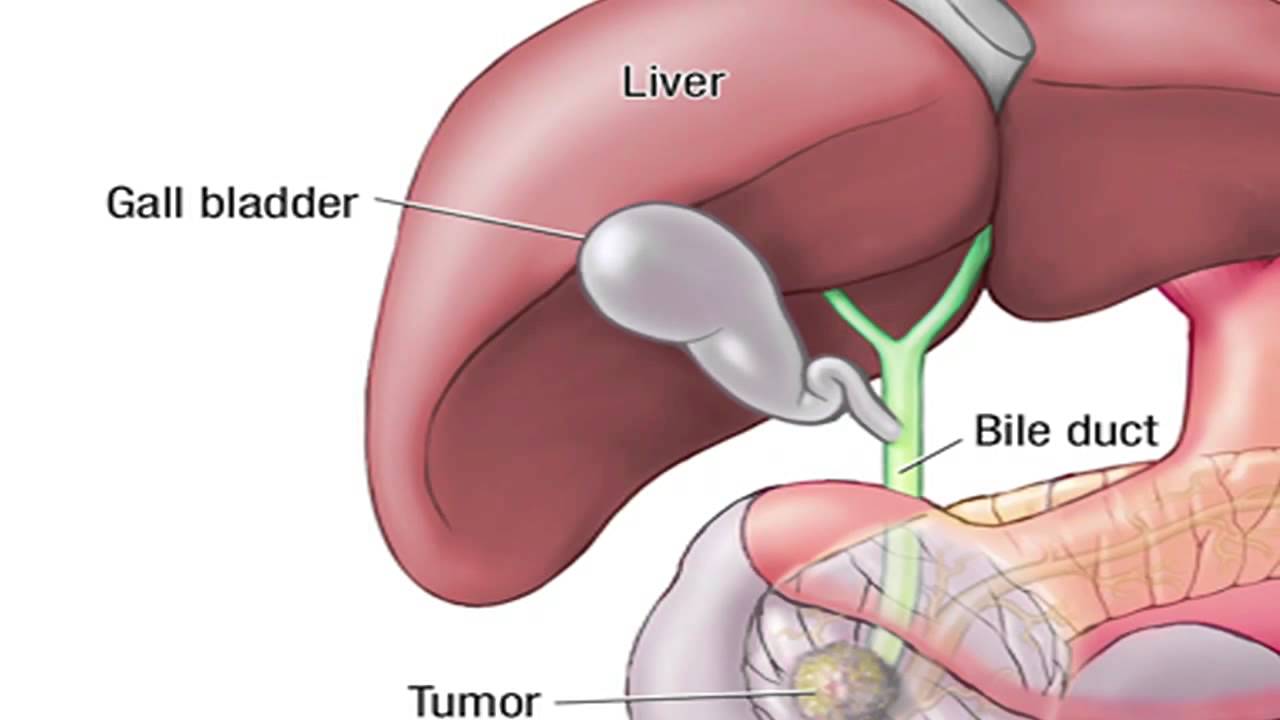
Dr. Horacio Asbun, Mayo Clinic in Florida, explains the Whipple procedure using this animated graphic of a pancreas. Cancer of the pancreas affects 45,000 people every year in the U.S., and it is the fourth leading cause of cancer-related deaths. The five-year overall survival rate if a tumor is detected early and surgically removed is 22 percent, versus 6 percent without early detection and surgery. To learn more, visit http://mayocl.in/2zk7FDi.
This video in Spanish/español: https://www.youtube.com/watch?v=N_zWboNMKWk

If a fetal lung lesion is causing heart failure, fetal surgery may be performed to remove the CCAM before birth. http://fetalsurgery.chop.edu
N. Scott Adzick, MD, Mark Johnson, MD, and Holly Hedrick, MD, experts from the Center for Fetal Diagnosis and Treatment at Children’s Hospital of Philadelphia, explain when fetal intervention for CCAM is recommended, the various approaches that may be used to treat the most complex fetal lung lesions before birth, and how these procedures are performed.
One concern with fetal lung lesions is that they take up space in the chest. If the lung mass grows and pushes the heart and other organs out of place, it can lead to complications such as fetal hydrops (heart failure in the fetus). If this happens, a fetal surgery procedure may be performed to remove the CCAM before birth.
In other cases, an EXIT procedure may be performed to partially deliver the baby, so the team can remove the mass before the baby is fully delivered.
In this video series, parents, nurses and doctors from Children’s Hospital of Philadelphia’s Center for Fetal Diagnosis and Treatment talk about the different types of fetal lung lesions like congenital cystic adenomatoid malformation (CCAM) and bronchopulmonary sequestration (BPS), the importance of accurate diagnosis and monitoring, and the most advanced treatment options currently available. They also discuss follow-up care and long-term outcomes for babies diagnosed with fetal lung lesions.
Thousands of Canadians undergo surgery every year, so how can you best prepare? The first step is having a dialogue, says Sunnybrook anesthesiologist Dr. Colin McCartney. Read the blog for more: http://sunnyview.sunnybrook.ca

For more information about Mohs surgery, please visit https://cle.clinic/3x7CRTy
Mohs surgery is a highly effective skin cancer removal procedure that takes just a few hours. It is most often used to treat basal cell and squamous cell carcinomas, the two most common skin cancers.
Chapters:
0:00 How effective is Mohs Surgery?
0:23 When is Mohs Surgery used?
0:50 How does Mohs Surgery work?
1:55 Does Mohs Surgery cure skin cancer?
2:06 How long is the recovery period after Mohs Surgery?
Resources:
Skins Cancer: https://cle.clinic/3G2MMM8
How Skin Cancer Is Found and Removed — At the Same Appointment: https://cle.clinic/3r9Wzu6
The Best Strategies To Reduce Your Risk of Skin Cancer: https://cle.clinic/38Bazqn
The information in this video was accurate as of 4.8.2022 and is for information purposes only. Consult your local medical authority or your healthcare practitioner for advice.
▶Share this video with others: https://youtu.be/aCV1UZ0Yj-o
▶Subscribe to learn more about Cleveland Clinic:
https://www.youtube.com/user/C....levelandClinic?sub_c
#ClevelandClinic #MohsSurgery #SkinCancer
Ettore Vulcano, MD, Foot and Ankle Orthopedic Surgeon at Mount Sinai West, discusses a new minimally invasive bunion surgery that has patients walking immediately after surgery, and getting back to an active lifestyle much quicker than with the traditional surgery.

Mini-Laparoscopic Cholecystectomy with Intraoperative Cholangiogram for Symptomatic Cholelithiasis (Gallstones) - Extended
Authors: Brunt LM1, Singh R1, Yee A2
Published: September 26, 2017
AUTHOR INFORMATION
1 Department of Surgery, Washington University, St. Louis, Missouri
2 Division of Plastic and Reconstructive Surgery, Washington University, St. Louis, Missouri
DISCLOSURE
No authors have a financial interest in any of the products, devices, or drugs mentioned in this production or publication.
ABSTRACT
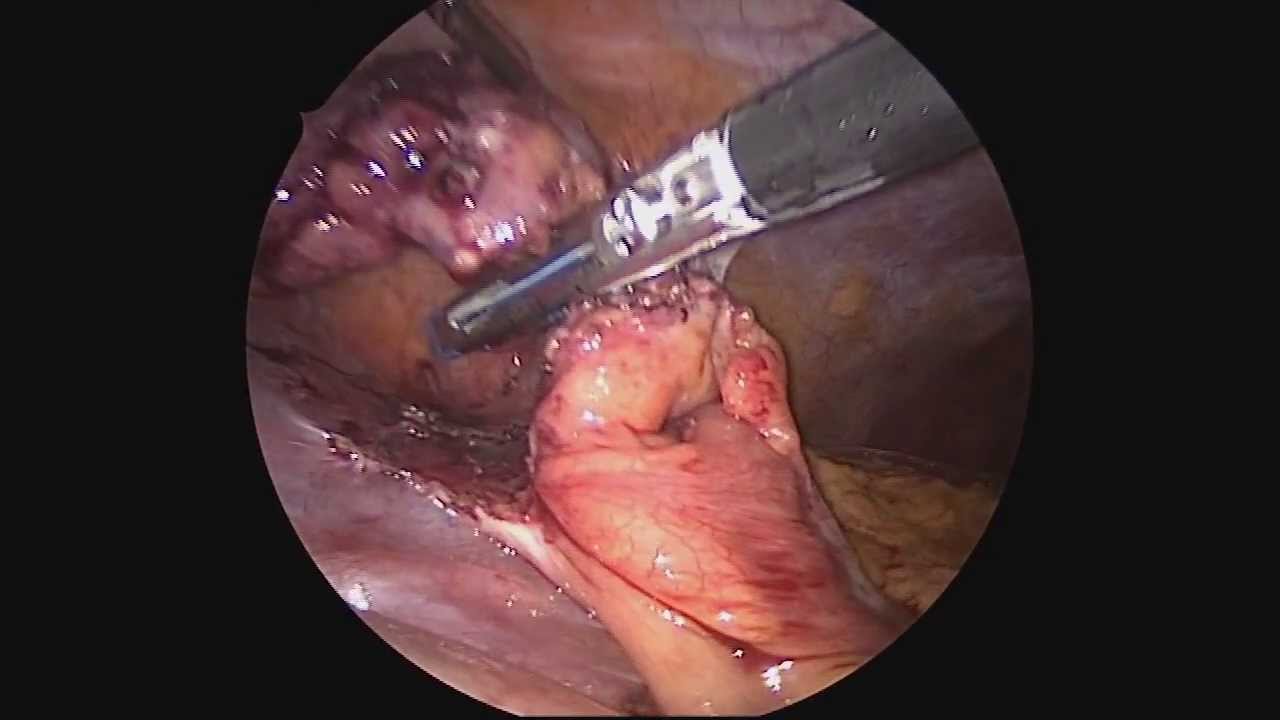
Minimal invasive laparoscopic cholecystectomy is the typical surgical treatment for cholelithiasis (gallstones), where patients present with a history of upper abdominal pain and episodes of biliary colic. The classic technique for minimal invasive laparoscopic cholecystectomy involves four ports: one umbilicus port, two subcostal ports, and a single epigastric port. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has instituted a six-step strategy to foster a universal culture of safety for cholecystectomy and minimize risk of bile duct injury. The technical steps are documented within the context of the surgical video for (1) achieving a critical view of safety for identification of the cystic duct and artery, (2) intraoperative time-out prior to management of the ductal structures, (3) recognizing the zone of significant risk of injury, and (4) routine intraoperative cholangiography for imaging of the biliary tree. In this case, the patient presented with symptomatic biliary colic due to a gallstone seen on the ultrasound in the gallbladder. The patient was managed a mini-laparoscopic cholecystectomy using 3mm ports for the epigastric and subcostal port sites with intraoperative fluoroscopic cholangiogram. Specifically, the senior author encountered a tight cystic duct preventing the insertion of the cholangiocatheter and the surgical video describes how the author managed the cystic duct for achieving a cholangiogram, in addition to the entire technical details of laparoscopic cholecystectomy.

.
Chapters
0:00 Introduction
1:04 Why do doctors perform laparoscopy?
2:11 How is laparoscopy performed?
3:22 Result
3:47 Risk of laparoscopy
Laparoscopy (from Ancient Greek λαπάρα (lapára) 'flank, side', and σκοπέω (skopéō) 'to see') is an operation performed in the abdomen or pelvis using small incisions (usually 0.5–1.5 cm) with the aid of a camera. The laparoscope aids diagnosis or therapeutic interventions with a few small cuts in the abdomen.[1]
Laparoscopic surgery, also called minimally invasive procedure, bandaid surgery, or keyhole surgery, is a modern surgical technique. There are a number of advantages to the patient with laparoscopic surgery versus an exploratory laparotomy. These include reduced pain due to smaller incisions, reduced hemorrhaging, and shorter recovery time. The key element is the use of a laparoscope, a long fiber optic cable system that allows viewing of the affected area by snaking the cable from a more distant, but more easily accessible location.
Laparoscopic surgery includes operations within the abdominal or pelvic cavities, whereas keyhole surgery performed on the thoracic or chest cavity is called thoracoscopic surgery. Specific surgical instruments used in laparoscopic surgery include obstetrical forceps, scissors, probes, dissectors, hooks, and retractors. Laparoscopic and thoracoscopic surgery belong to the broader field of endoscopy. The first laparoscopic procedure was performed by German surgeon Georg Kelling in 1901. There are two types of laparoscope:[2]
A telescopic rod lens system, usually connected to a video camera (single-chip or three-chip)
A digital laparoscope where a miniature digital video camera is placed at the end of the laparoscope, eliminating the rod lens system
The mechanism mentioned in the second type is mainly used to improve the image quality of flexible endoscopes, replacing conventional fiberscopes. Nevertheless, laparoscopes are rigid endoscopes. Rigidity is required in clinical practice. The rod-lens-based laparoscopes dominate overwhelmingly in practice, due to their fine optical resolution (50 µm typically, dependent on the aperture size used in the objective lens), and the image quality can be better than that of the digital camera if necessary. The second type of laparoscope is very rare in the laparoscope market and in hospitals.[citation needed]
Also attached is a fiber optic cable system connected to a "cold" light source (halogen or xenon) to illuminate the operative field, which is inserted through a 5 mm or 10 mm cannula or trocar. The abdomen is usually insufflated with carbon dioxide gas. This elevates the abdominal wall above the internal organs to create a working and viewing space. CO2 is used because it is common to the human body and can be absorbed by tissue and removed by the respiratory system. It is also non-flammable, which is important because electrosurgical devices are commonly used in laparoscopic procedures.[3]
Procedures
Surgeons perform laparoscopic stomach surgery.
Patient position
During the laparoscopic procedure, the position of the patient is either in Trendelenburg position or in reverse Trendelenburg. These positions have an effect on cardiopulmonary function. In Trendelenburg's position, there is an increased preload due to an increase in the venous return from lower extremities. This position results in cephalic shifting of the viscera, which accentuates the pressure on the diaphragm. In the case of reverse Trendelenburg position, pulmonary function tends to improve as there is a caudal shifting of viscera, which improves tidal volume by a decrease in the pressure on the diaphragm. This position also decreases the preload on the heart and causes a decrease in the venous return leading to hypotension. The pooling of blood in the lower extremities increases the stasis and predisposes the patient to develop deep vein thrombosis (DVT).[4]
Gallbladder
Rather than a minimum 20 cm incision as in traditional (open) cholecystectomy, four incisions of 0.5–1.0 cm, or more recently, a single incision of 1.5–2.0 cm,[5] will be sufficient to perform a laparoscopic removal of a gallbladder. Since the gallbladder is similar to a small balloon that stores and releases bile, it can usually be removed from the abdomen by suctioning out the bile and then removing the deflated gallbladder through the 1 cm incision at the patient's navel. The length of postoperative stay in the hospital is minimal, and same-day discharges are possible in cases of early morning procedures.[citation needed]
Colon and kidney
Dr. Celia Divino, Chief, Division of General Surgery at The Mount Sinai Hospital, performs a laparoscopic appendectomy. Visit the Division of General Surgery at http://bit.ly/18z944M. Click here to learn more about Dr. Celia Divino http://bit.ly/12RF0ee

This Basic Laparoscopic Surgery: Abdominal Access and Trocar Introduction course will teach you the steps of Laparoscopic Surgery. View the full course for free by signing up on our website: https://www.incision.care/
What is Laparoscopic Surgery:
Laparoscopic surgery describes procedures performed using one or multiple small incisions in the abdominal wall in contrast to the larger, normally singular incision of laparotomy. The technique is based around principles of minimally invasive surgery (or minimal access surgery): a large group of modern surgical procedures carried out by entering the body with the smallest possible damage to tissues. In abdominopelvic surgery, minimally invasive surgery is generally treated as synonymous with laparoscopic surgery as are procedures not technically within the peritoneal cavity, such as totally extraperitoneal hernia repair, or extending beyond the abdomen, such as thoraco-laparoscopic esophagectomy. The term laparoscopy is sometimes used interchangeably, although this is often reserved to describe a visual examination of the peritoneal cavity or the purely scopic component of a laparoscopic procedure. The colloquial keyhole surgery is common in non-medical usage.
Surgical Objective of Laparoscopic Surgery:
The objective of a laparoscopic approach is to minimize surgical trauma when operating on abdominal or pelvic structures. When correctly indicated and performed, this can result in smaller scars, reduced postoperative morbidity, shorter inpatient durations, and a faster return to normal activity. For a number of abdominopelvic procedures, a laparoscopic approach is now generally considered to be the gold-standard treatment option.
Definitions
Developments of Laparoscopic Surgery:
Following a number of smaller-scale applications of minimally invasive techniques to abdominopelvic surgery, laparoscopic surgery became a major part of general surgical practice with the introduction of laparoscopic cholecystectomy in the 1980s and the subsequent pioneering of endoscopic camera technology. This led to the widespread adoption of the technique by the early- to mid-1990s. The portfolio of procedures that can be performed laparoscopically has rapidly expanded with improvements in instruments, imaging, techniques and training — forming a central component of modern surgical practice and cross-specialty curricula [2]. Techniques such as laparoscopically assisted surgery and hand-assisted laparoscopic surgery have allowed the application of laparoscopic techniques to a greater variety of pathology. Single-incision laparoscopic surgery, natural orifice transluminal endoscopic surgery, and minilaparoscopy-assisted natural orifice surgery continue to push forward the applications of minimally invasive abdominopelvic techniques; however, the widespread practice and specific indications for these remain to be fully established. More recently, robotic surgery has been able to build on laparoscopic principles through developments in visualization, ergonomics, and instrumentation.
This Basic Laparoscopic Surgery: Abdominal Access and Trocar Introduction course will teach you:
- How to access the abdomen using an open, closed, and direct optical-entry technique
- Principles underlying safe abdominal insufflation
- The vascular anatomy of the abdominal wall and its implications for trocar placement
- How to introduce trocars into the peritoneal cavity
- The principle of triangulation and how this can be applied to organizing a laparoscopic surgical field
Specific attention is given to these hazards you may encounter:
- Intravascular, intraluminal, or extraperitoneal needle position
- Limitations of a closed introduction technique
- Abdominal surgical history
- Limitations of an open introduction technique
- Optical trocar entry in thin individuals
- Visualization of non-midline structures
- Limitations of direct optical-entry techniques
- Limitations of clinical examination to confirm intraperitoneal insufflation
- Leakage of insufflation gas
These tips are designed to help you improve your understanding and performance:
- Alternative left upper quadrant approach
- Testing Veress needle before use
- Lifting the abdominal wall for Veress needle introduction
- "Hanging-drop test"
- Palmer's test
- Confirming intra-abdominal insufflation
- Subcutaneous tissue retraction
- Anatomy of the umbilicus
- Retraction of abdominal wall fascia
- Finger sweep of anterior abdominal wall
- Lifting the abdominal wall for optical trocar introduction
- Identification of venous bleeding at the end of a procedure
- Identification of inferior epigastric vessels by direct vision
- Peritoneal folds of the anterior abdominal wall
- Transillumination of superficial epigastric vessels
- Infiltration of local anesthetic at port sites
- Aiming of trocars
- Selection of trocar size
- Maintaining direct vision

OB_A_1013
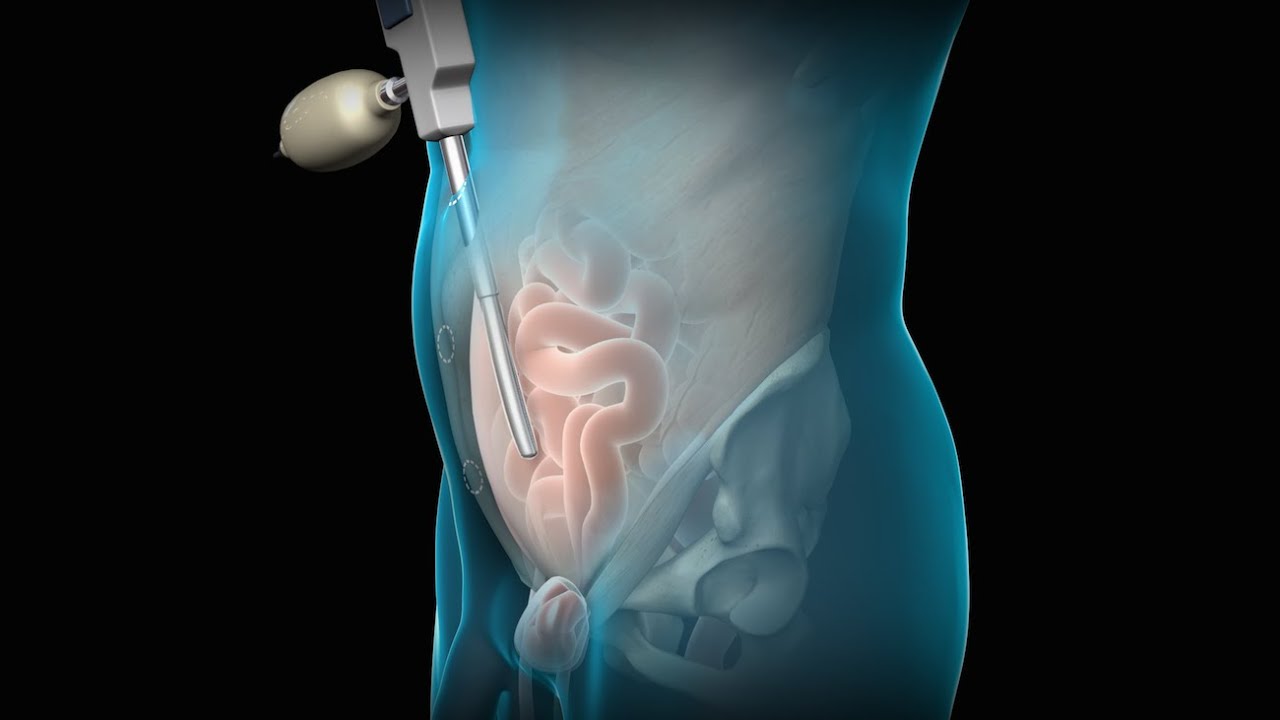
3D animation depicting the operating room and initial procedure preparing the patient for a laparoscopic hysterectomy. The patient is prepped and draped in the usual fashion and surrounded by the surgeon and surgical assistants. The skin is elevated, an infraumbilical incision is made, a trocar port is inserted through the incision and the abdomen is insufflated. Finally, a laparoscope is inserted into the port to allow for direct visualization of the uterus and the surgery can begin.
To view more animations and exhibits, visit our medical library: https://www.trialexhibitsinc.c....om/library/multimedi
Contact us on your next case for consulting, trial graphics, animations, medical illustrations or presentation services. 800-591-1123 [a]www.trialex.com[/a]
This video is for reference only. The video may not be otherwise used, reproduced nor modified. For more information to purchase a copy or permission to use this animation on your next case, project, website or TV, contact us at [a]www.trialex.com[/a] or 800-591-1123.
Copyright @ Trial Exhibits, Inc.

UChicago Medicine organ transplant surgeon Dr. Rolf Barth explains a how the laparoscopic donor nephrectomy – also known as the single-port nephrectomy – procedure works to remove an organ donor’s kidney from their body to be transplanted into a recipient. This minimally invasive kidney donor transplant surgery allows living organ donors the get back to their lives more quickly than the traditional approach and leaves them with a nearly invisible scar in the belly button.
Learn more about living kidney donation: https://www.uchicagomedicine.o....rg/conditions-servic
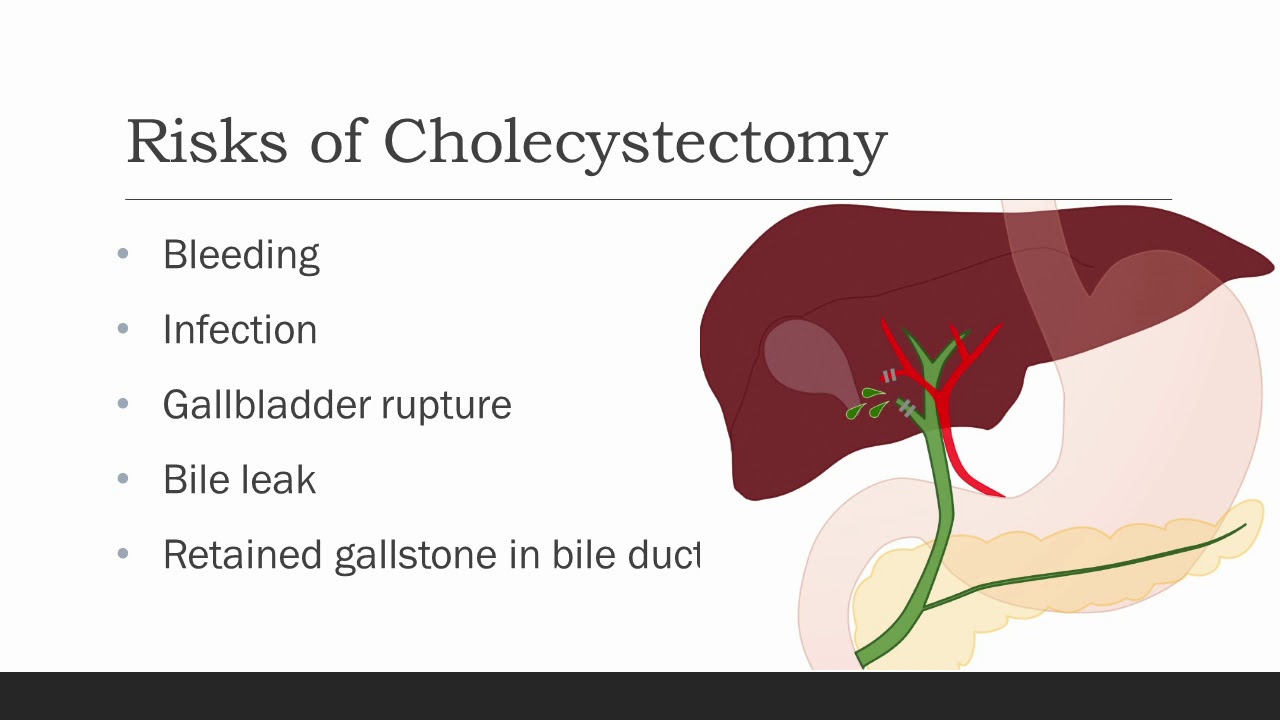
Cholecystectomy means removal of the gallbladder. The most common reasons
your doctor might recommend a cholecystectomy are biliary colic, cholecystitis,
choledocolithiasis, or gallstone pancreatitis. Biliary colic, also known as symptomatic
cholelithiasis, is caused by gallstones, which are hardened deposits of bile. Gallstones are
common in the general population, and gallstones alone are not a reason for gallbladder
removal if they do not cause symptoms. However, sometimes gallstones can get caught at the
neck of the gallbladder, causing pain when the gallbladder contracts against them trying to
release its bile, especially after a fatty meal. With biliary colic, the pain typically resolves within
an hour or so. Occasionally, a stone or some other blockage may prevent the gallbladder from
emptying over a long period of time, causing an increase in pressure and trapped fluid within the
gallbladder. This can cause inflammation and infection of the gallbladder, which we call
cholecystitis. Choledocholithiasis is when there are one or more stones in the bile ducts, which
can cause back up of bile into the liver, and depending on the location of the stones, could
cause pancreatitis, which is inflammation of the pancreas. Other reasons for gallbladder
removal, though less common, are gallbladder polyps and cancer. All of these are reasons for
gallbladder removal.

Mini-Laparoscopic Cholecystectomy with Intraoperative Cholangiogram for Symptomatic Cholelithiasis (Gallstones) - Standard
Authors: Brunt LM1, Singh R1, Yee A2
Published: September 26, 2017
AUTHOR INFORMATION
1 Department of Surgery, Washington University, St. Louis, Missouri
2 Division of Plastic and Reconstructive Surgery, Washington University, St. Louis, Missouri
DISCLOSURE
No authors have a financial interest in any of the products, devices, or drugs mentioned in this production or publication.
ABSTRACT
Minimal invasive laparoscopic cholecystectomy is the typical surgical treatment for cholelithiasis (gallstones), where patients present with a history of upper abdominal pain and episodes of biliary colic. The classic technique for minimal invasive laparoscopic cholecystectomy involves four ports: one umbilicus port, two subcostal ports, and a single epigastric port. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has instituted a six-step strategy to foster a universal culture of safety for cholecystectomy and minimize risk of bile duct injury. The technical steps are documented within the context of the surgical video for (1) achieving a critical view of safety for identification of the cystic duct and artery, (2) intraoperative time-out prior to management of the ductal structures, (3) recognizing the zone of significant risk of injury, and (4) routine intraoperative cholangiography for imaging of the biliary tree. In this case, the patient presented with symptomatic biliary colic due to a gallstone seen on the ultrasound in the gallbladder. The patient was managed a mini-laparoscopic cholecystectomy using 3mm ports for the epigastric and subcostal port sites with intraoperative fluoroscopic cholangiogram. Specifically, the senior author encountered a tight cystic duct preventing the insertion of the cholangiocatheter and the surgical video describes how the author managed the cystic duct for achieving a cholangiogram, in addition to the entire technical details of laparoscopic cholecystectomy.
To license this video for patient education or content marketing, visit: http://www.nucleushealth.com/?utm_source=youtube&utm_medium=video-description&utm_campaign=tephernia-030615
An inguinal hernia is a bulging of the intestine through a defect or weak spot in the wall of the lower abdomen. This video shows how inguinal hernias form and how they are treated.
#TotalExtraperitonealLaparoscopicInguinalHerniaRepair #TEP #laparoscopy
ANCE00200


