Top videos

Find our full video library only on Osmosis Prime: http://osms.it/more.
Join over 3 million current & future clinicians who learn by Osmosis, and over 130 universities around the world who partner with us to make medical and health education more engaging and efficient. We have unparalleled tools and materials to prepare you to succeed in school, on board exams, and as a future clinician. Sign up for a free trial at http://osms.it/more. If you're interested in exploring an institutional partnership, visit osmosis.org/educators to request a personalized demo.
Follow us on social:
Facebook: http://osms.it/facebook
Twitter: http://osms.it/twitter
Instagram for med: http://osms.it/instagram
Instagram for nursing: https://osms.it/ignursing
Linkedin: https://osms.it/linkedin
Our Vision: Everyone who cares for someone will learn by Osmosis.
Our Mission: To empower the world’s clinicians and caregivers with the best learning experience possible. Learn more here: http://osms.it/mission
Medical disclaimer: Knowledge Diffusion Inc (DBA Osmosis) does not provide medical advice. Osmosis and the content available on Osmosis's properties (Osmosis.org, YouTube, and other channels) do not provide a diagnosis or other recommendation for treatment and are not a substitute for the professional judgment of a healthcare professional in diagnosis and treatment of any person or animal. The determination of the need for medical services and the types of healthcare to be provided to a patient are decisions that should be made only by a physician or other licensed health care provider. Always seek the advice of a physician or other qualified healthcare provider with any questions you have regarding a medical condition. © 2023 Elsevier. All rights reserved.

This video - produced by students at Oxford University Medical School - demonstrates how to perform an examination of the respiratory system. It also indicates common pathologies encountered. It is part of a series of videos covering basic clinical examinations and is linked to Oxford Medical Education (www.oxfordmedicaleducation.com).

Cardiovascular Examination Clinical skills - Medical School Revision - Dr Gill
The cardiac exam is one of the clinical skills that medical students learn completely, as more often than not, patients will consult regularly about chest pain, and it is important to be able to identify key cardiovascular signs
As a junior doctor, the examination of the cardiovascular system can be almost a dreaded examination, as cardiac murmurs can literally take years of exposure in order to gain confidence with their identification through cardiac auscultation.
This video demonstrates not merely the examination of the heart, but the complete cardiovascular system including its peripheries.
I hope these clinical skill revision videos are helpful, please like and subscribe and join the community so that we can create more effective videos to help with your journey through medical school
#ClinicalExamination #ASMR #drgill
Some people have found this video useful for ASMR

In this video, the viewer will learn the key aspects of the newborn physical exam, and how to distinguish between normal and abnormal findings.
Direct Links to chapters:
0:00-Intro
1:30-Head
3:49-Face
8:05-Neck
8:30-Chest
10:13-Abdomen
11:01-Groin
13:17-Extremities
14:05-Back
14:47-Neurologic
Please visit: www.openpediatrics.org
OPENPediatrics™ is an interactive digital learning platform for healthcare clinicians sponsored by Boston Children's Hospital and in collaboration with the World Federation of Pediatric Intensive and Critical Care Societies. It is designed to promote the exchange of knowledge between healthcare providers around the world caring for critically ill children in all resource settings. The content includes internationally recognized experts teaching the full range of topics on the care of critically ill children. All content is peer-reviewed and open access-and thus at no expense to the user.
For further information on how to enroll, please email: openpediatrics@childrens.harvard.edu
Please note: OPENPediatrics does not support nor control any related videos in the sidebar, these are placed by Youtube. We apologize for any inconvenience this may cause.

Ear Examination ENT is often a challenging examination, crossing over with the cranial nerve examination of the vestibular cochlear exam as well at other neurological assessments of balance
Here we will review the ear examination, looking both at the use of the otoscope, but also the Dix-Hallpike Manoeuvre, along with HINTS assessment. the Webers and Rinne's test is also included to determine types of hearing loss.
Often these ear examination techniques are performed separately, depending on the patients presenting complaint
#EARExamination #DrGill #ClinicalSkills

The most reliable clinical sign to detect ascites is checking for bilateral flank dullness. If a patient with ascites is lying supine, fluid accumulates in the flank regions, leading to dullness on percussion. At the same time, the air-filled bowel loops are forced upwards by the free fluid due to buoyancy, resulting in tympanitic percussion. To locate specifically where dullness shifts to tympany, or the air-fluid level, percussion should be performed from the sides towards the middle. To confirm that the dullness is caused by ascites, ask the patient to switch to a lateral decubitus position. If ascites is present, the air-filled bowel loops will shift accordingly and remain at the surface of the fluid. As a result, the air-fluid level will shift as well. This is known as shifting dullness.
Subscribe to AMBOSS YouTube for the latest clinical examination videos, medical student interviews, study tips and tricks, and live webinars!
Free 5 Day Trial: https://go.amboss.com/amboss-YT
Instagram: https://www.instagram.com/amboss_med/
Facebook: https://www.facebook.com/AMBOSS.Med/
Twitter: https://twitter.com/ambossmed
Blog: https://blog.amboss.com/us
#AMBOSSMed #ClinicalExamination
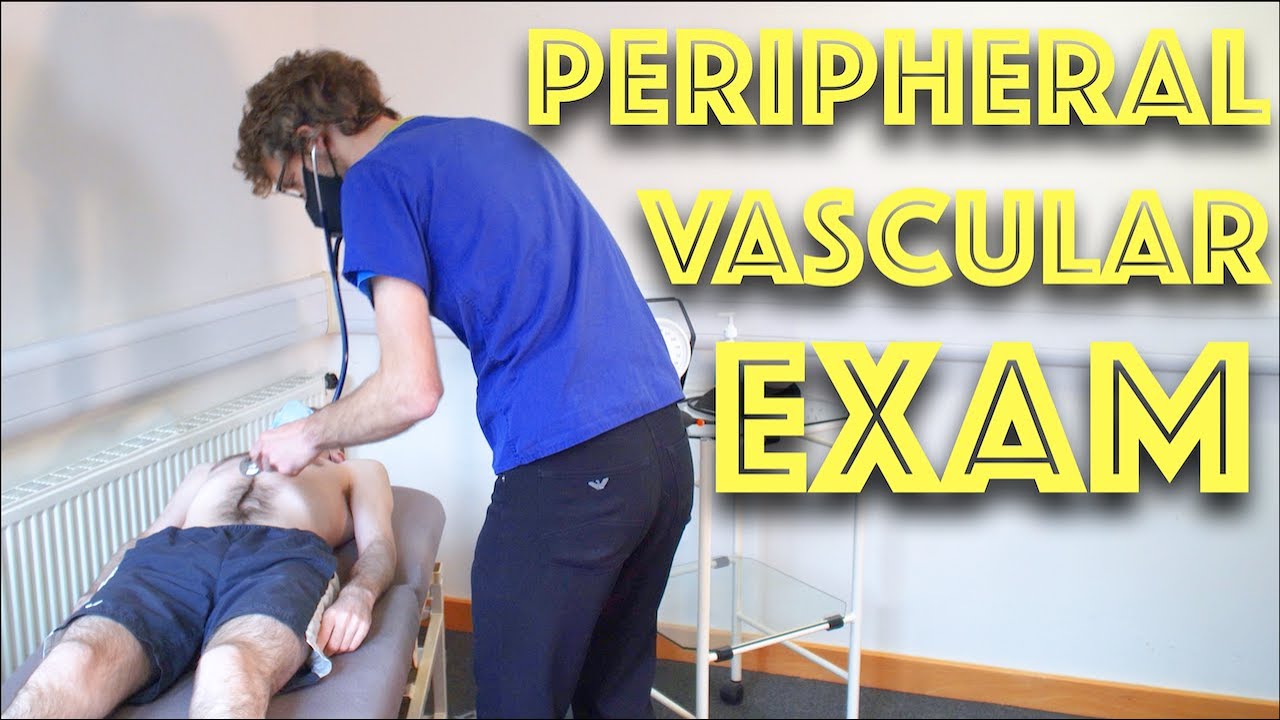
Peripheral Vascular Examination OSCE - Clinical Skills - Dr Gill
In the cardiovascular examination, particularly in the case of an OSCE station, we conclude the examination often by stating that the examiner would want to perform:
- An ECG
- Check full blood count
- and "do a peripheral vascular examination
In this video, we demonstrate that oft-talked about, but comparatively less common examination.
Starting off, with the examination of the hands, the radial, brachial and carotid pulses. before moving down to assess for a AAA, checking the femoral and popliteal pulses, before wrapping up around the ankle with the posterior tibial and dorsalis pedis pulses
For completeness, the cardiovascular examination is demonstrated here
https://www.youtube.com/watch?v=ECs9O5zl6XQ&t=2s
#PeripheralVascular #ClinicalSkills #DrGill

Lesson on clinical examination of a scaphoid fracture and assessment of the anatomic snuffbox. The scaphoid bone is one of the carpal bones of the wrist. A scaphoid fracture is important to rule out due to risk of avascular necrosis, which is a compromise of bone vasculature leading to death of the bone. Scaphoid fractures can occur with a FOOSH injury. In this lesson, we discuss the clinical assessment to rule out a scaphoid fracture, including assessing and localizing the anatomic snuffbox.
If you find this lesson helpful, please consider liking, subscribing, and clicking the notification bell to help support this channel and stay up-to-date on future lessons.
*Subscribe for more free medical lessons* https://www.youtube.com/channe....l/UCFPvnkCZbHfBvV8Ap
-------------------------------------------------------------------------------------------------------------
For books and more information on these topics
https://www.amazon.com/shop/jjmedicine
Support future lessons (and get other cool stuff) ➜ https://www.patreon.com/jjmedicine
Follow me on Twitter! ➜ https://twitter.com/JJ_Medicine
Come join me on Facebook! ➜ https://www.facebook.com/JJ-Me....dicine-1006426481611
Start your own website with BlueHost ➜ https://www.bluehost.com/track/jjmedicine/
Check out the best tool to help grow your YouTube channel (it’s helped me!)
https://www.tubebuddy.com/jjmedicine
-------------------------------------------------------------------------------------------------------------
Check out some of my other lessons.
Medical Terminology - The Basics - Lesson 1:
https://www.youtube.com/watch?v=04Wh2E9oNug
Fatty Acid Synthesis Pathway:
https://www.youtube.com/watch?v=WuQS_LpNMzo
Wnt/B Catenin Signaling Pathway:
https://www.youtube.com/watch?v=NGVP4J9jpgs
Upper vs. Lower Motor Neuron Lesions:
https://www.youtube.com/watch?v=itNd74V53ng
Lesson on the Purine Synthesis and Salvage Pathway:
https://www.youtube.com/watch?v=e2KFVvI8Akk
Gastrulation | Formation of Germ Layers:
https://www.youtube.com/watch?v=d6Kkn0SECJ4
Introductory lesson on Autophagy (Macroautophagy):
https://www.youtube.com/watch?v=UmSVKzHc5yA
Infectious Disease Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Dermatology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Pharmacology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Hematology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Rheumatology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Endocrinology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
Nephrology Playlist
https://www.youtube.com/playli....st?list=PLRjNoiRtdFw
----------------------------------------------------------------------------------------------------
**MEDICAL DISCLAIMER**: JJ Medicine does not provide medical advice, and the information available on this channel does not offer a diagnosis or advice regarding treatment. Information presented in these lessons is for educational purposes ONLY, and information presented here is not to be used as an alternative to a healthcare professional’s diagnosis and treatment of any person/animal.
Only a physician or other licensed healthcare professional are able to determine the requirement for medical assistance to be given to a patient. Please seek the advice of your physician or other licensed healthcare provider if you have any questions regarding a medical condition.
----------------------------------------------------------------------------------------------------
*Although I try my best to present accurate information, there may be mistakes in this video. If you do see any mistakes with information in this lesson, please comment and let me know.*
I am always looking for ways to improve my lessons! Please don't hesitate to leave me feedback and comments - all of your feedback is greatly appreciated! :) And please don't hesitate to send me any messages if you need any help - I will try my best to be here to help you guys :)
Thanks for watching! If you found this video helpful, please like and subscribe!
JJ

#ComprehensiveClinicalClass
History, Examination and Management of Hernia
Mentor: Dr. Nishanth, Consultant Surgeon, Bengaluru.
THE WHITE ARMY
To make studies more interesting and enjoyable, we are constantly trying to share most important tables, charts, diagrams, mnemonics, scoring systems, diagnostic criterias, motivating quotes and other useful study materials on
ANDROID APP - All in 1 Free Medical Education App for Medicos
https://play.google.com/store/....apps/details?id=com.
INSTAGRAM PAGE
@the_whitearmy
https://www.instagram.com/the_whitearmy/
TELEGRAM GROUP
PDFs, PPTs and other study materials stored for easy, convenient access and download.
https://t.me/whitearmyofmedicos
Anyone interested to present clinical cases, willing to join whatsapp discussion group, can send a mail to whitearmyofmedicos@gmail.com
#StudyManiaInSocialMedia
#HelpOthersToHelpOurselves
#StudyEnjoyingEnjoyStudying
DISCLAIMER
THE WHITE ARMY does not own or claim to own any of the media used in the following video/stream. The media belong to their respective owners who may have copyright over them.The media have been taken from various sources and are used for medical educational purposes only. The following video/stream may contain images that may not be suitable for all audiences, viewer discretion is advised.

Learn with Dr. Wahdan 2
You can download the lecture from this link
https://docdro.id/5ni1FFZ

The anatomy of the direct and indirect inguinal hernia.
Music:
Berries and Lime by Gregory David
https://www.epidemicsound.com/track/z6iCiiyCPm/

This is how Paraumbilical hernia looks like and how it is examined although it looks very simple but in exam it can be very difficult to perform all steps in small amount of time. This can be short case or even long of #cpsp #fcps #mbbs #medicalstudent #mbbsexams #plab2 #plab #plab1 and MS #genernalknowledge #surgery exams
#para-umbilical hernia
#umbilical hernia #paraumbilical #hernia repair#laparoscopic paraumbilical hernia repair. #umbilical defect, #vetral hernia surgery. #herniatreatment #herniatreatment #ventral hernia hernia,#laparoscopic ventral hernia repair,umbilicus,carl lowe jr,hernia repair,training,north carolina,hernia repair surgery,charlotte,operation,laparoscopic,bulge,surgery,surgeon,dr. lowe,ipom repair,live surgery,mesh,
#mesh #ipom repair

In this video, Professor Dan Reinstein performs a bilateral LASIK procedure filmed in real-time to demonstrate the full 8 and-a-half minute procedure from multiple angles. The superior design and experience of the Carl Zeiss Meditec Visumax femtosecond Laser for flap creation is seen, where the patient is only in contact with the device for about 30 seconds with extremely low contract force such that the patient feels effectively nothing, there are no red splodges (subconjunctival haemorages) left behind. From the surgeons' standpoint there is no device that is easier to use or faster for LASIK flap creation. The Carl Zeiss Meditec MEL80 excimer laser portion of the procedure is seamlessly integrated and incorporates all the features that make clinical outcomes so reproducible including the unique cone-for-controlled-atmosphere (CCA) and high efficiency, high sensitivity calibration test which can be performed for each individual patient to compensate for minor changes in energy that occur with excimer laser devices during the course of a day.
For reference to the clinical outcomes for LASIK with the MEL80 in presbyopia using PRESBYOND Laser Blended Vision see:
Reading glasses presbyopia (ageing eyes) only:
LASIK for presbyopia correction in emmetropic patients using aspheric ablation profiles and a micro-monovision protocol with the Carl Zeiss Meditec MEL 80 and VisuMax.
J Refract Surg. 2012 Aug;28(8):531-41. Reinstein DZ, Carp GI, Archer TJ, Gobbe M.
http://www.ncbi.nlm.nih.gov/pubmed/22869232
Short sighted, astigmatism and presbyopia (ageing eyes)
LASIK for Myopic Astigmatism and Presbyopia Using Non-Linear Aspheric Micro-Monovision with the Carl Zeiss Meditec MEL 80 Platform.
J Refract Surg. 2011 Jan;27(1):23-37. Epub 2010 Mar 1.
Reinstein DZ, Archer TJ, Gobbe M.
http://www.ncbi.nlm.nih.gov/pubmed/20205360
Long-sighted, astigmatism and presbyopia (ageing eyes)
LASIK for hyperopic astigmatism and presbyopia using micro-monovision with the Carl Zeiss Meditec MEL80 platform.
J Refract Surg. 2009 Jan;25(1):37-58. Reinstein DZ, Couch DG, Archer TJ.
http://www.ncbi.nlm.nih.gov/pubmed/19244952
For more information about laser eye surgery and PRESBYOND Laser Blended Vision, please contact the London Vision Clinic on 020 7224 1005.
Ever considered getting laser eye surgery, but didn’t know how it worked? Allow us to help!
There are three different main types of laser eye surgery: LASIK, SMILE, and Surface Laser Treatments, and each can be explained pretty easily.
LASIK uses two lasers to open up a thin flap on the surface of the cornea, and then reshapes the cornea underneath. The flap is then placed back over the reshaped cornea, and heals independently with time.
SMILE uses one laser to reshape the cornea through a small, self-healing hole.
And Surface Eye Treatments remove the clear skin over the eye, to then reshape the cornea underneath with - you guessed it - a laser!

If you are tired of dealing with glasses or squinting to read signs in the distance, then you should consider LASIK Eye Surgery. In this outpatient refractive procedure, lasers are used to correct vision issues by changing the structure of the cornea. This may entirely eliminate reliance upon glasses or contacts. In this interactive LASIK Eye Surgery, you will assist in numbing the patient’s eye and cleaning the area for the procedure. With a speculum, you will hold the eye open, mark the cornea using a water-soluble ink, then attach a suction ring to it. After that, a specialized blade device is used to cut into the corneal flap and peel it back so that the laser can clear away corneal tissue underneath. This process corrects the shape of the cornea in less than a minute before putting the corneal flap back in place. After the procedure, we will go over LASIK Eye Surgery recovery instructions. Scrub in and let’s get started!






