Top videos
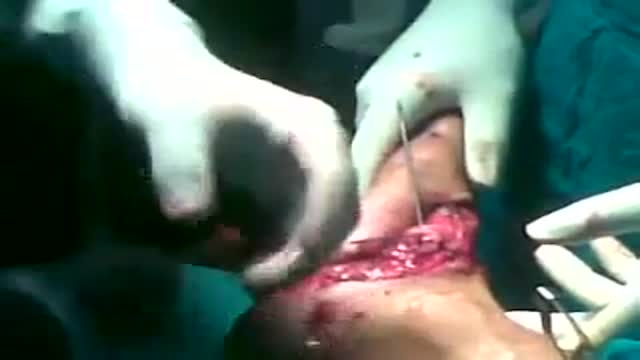
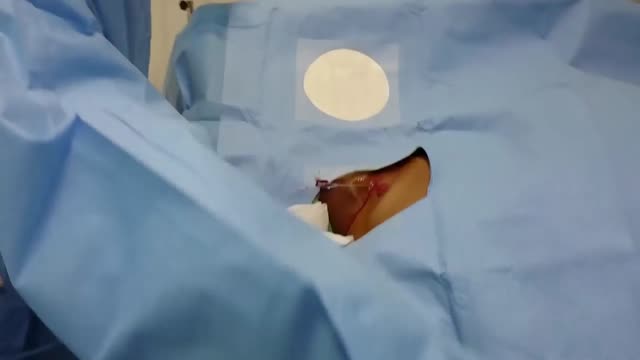
Kirschner wires or K-wires or pins are sterilized, sharpened, smooth stainless steel pins. Introduced in 1909 by Martin Kirschner, the wires are now widely used in orthopaedics and other types of medical and veterinary surgery. They come in different sizes and are used to hold bone fragments together (pin fixation) or to provide an anchor for skeletal traction. The pins are often driven into the bone through the skin (percutaneous pin fixation) using a power or hand drill. They also form part of the Ilizarov apparatus.
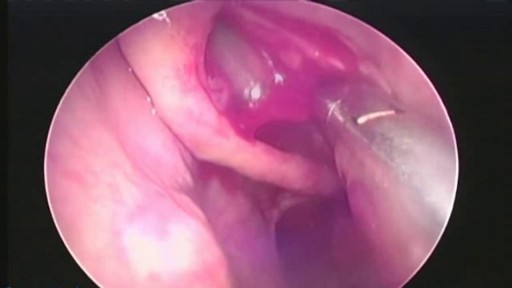
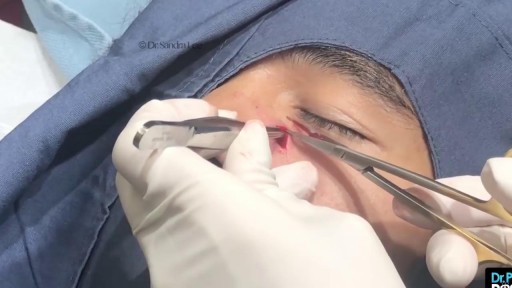
Nasal polyps are linked to allergic rhinitis, asthma, aspirin allergy, sinus infections, acute and chronic infections, something stuck in the nose, and cystic fibrosis. But many times the cause is unknown. Sometimes, people get them before they develop asthma or sinusitis
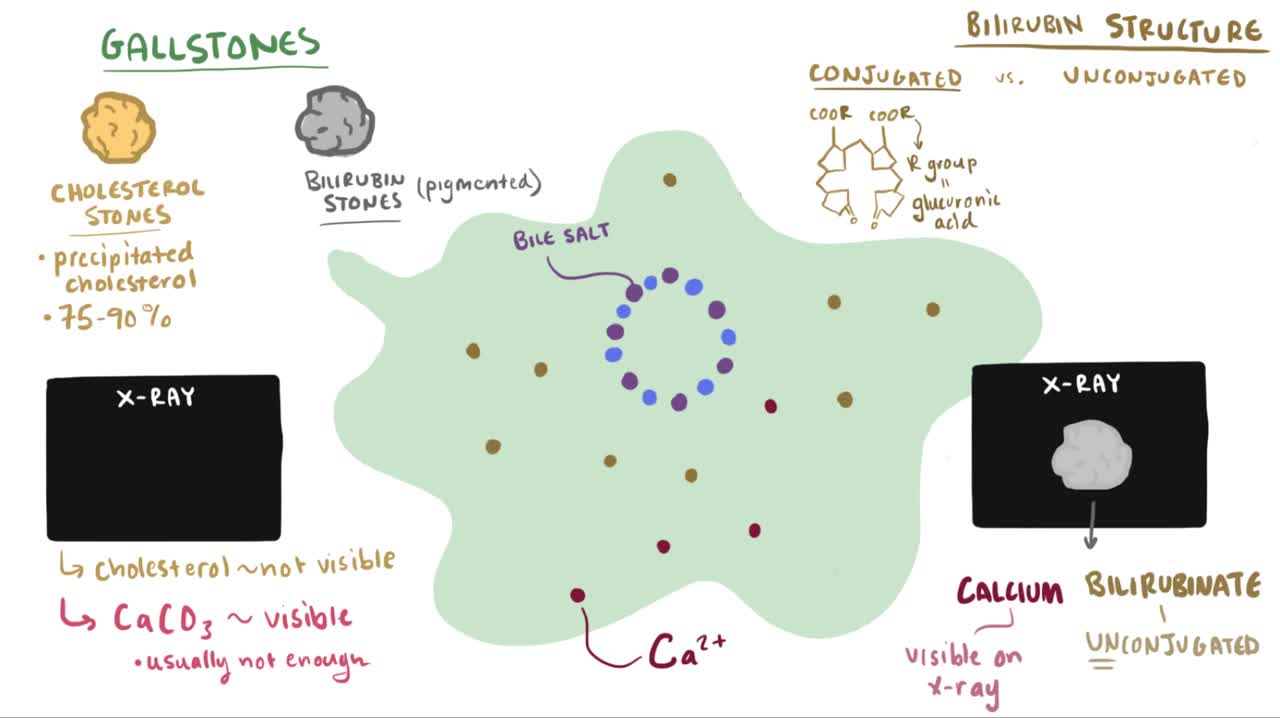
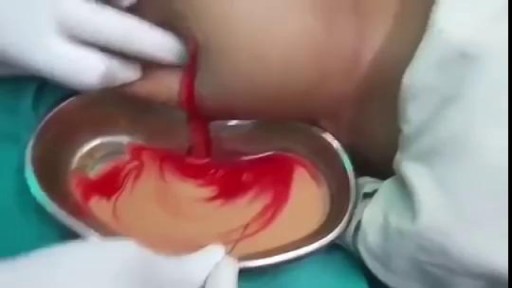
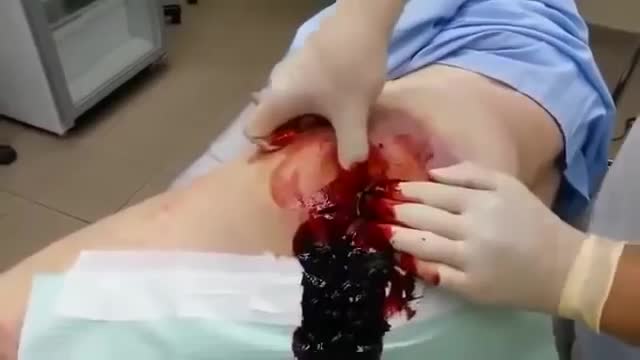
Cholelithiasis involves the presence of gallstones (see the image below), which are concretions that form in the biliary tract, usually in the gallbladder. Choledocholithiasis refers to the presence of 1 or more gallstones in the common bile duct (CBD).
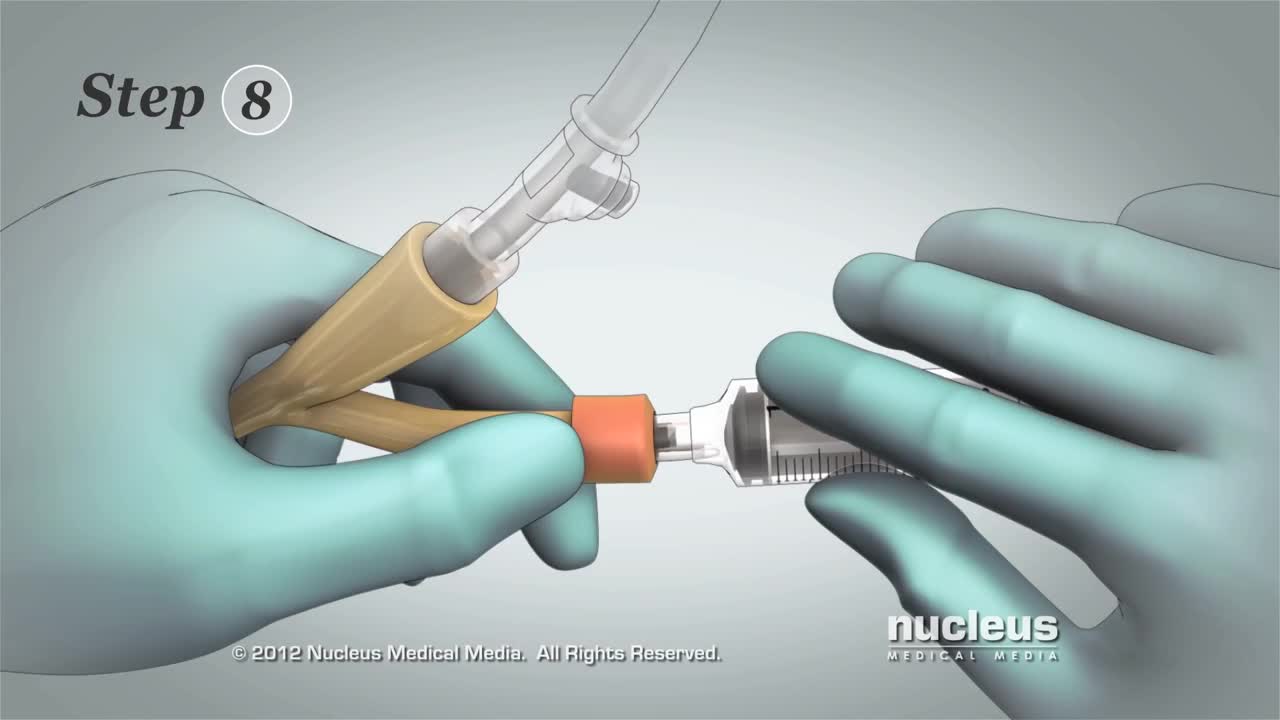
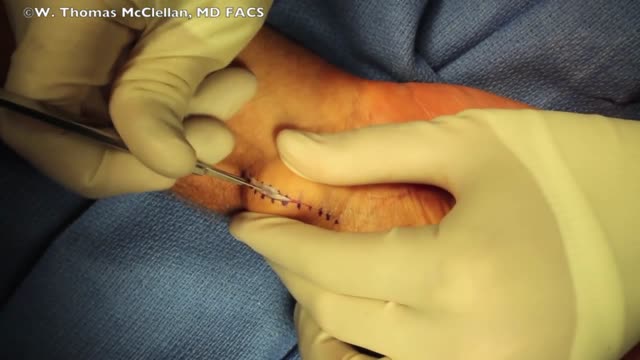
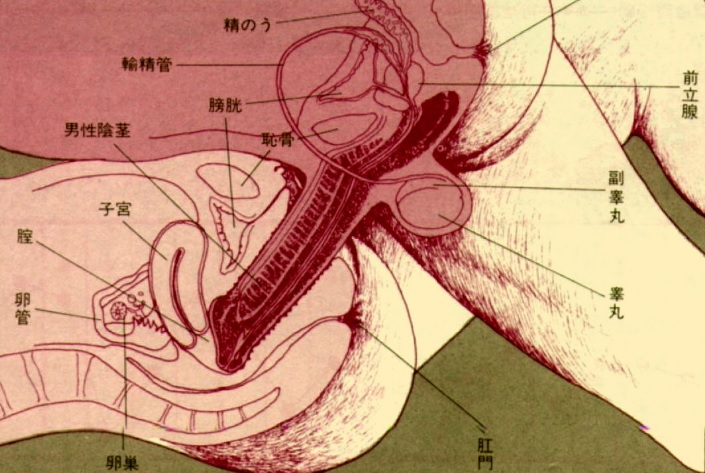
This 3D medical animation contains the discharge instructions for removal of a Foley catheter from a man. The step-by-step procedures for emptying the Foley bag and removing the Foley catheter are shown. Symptoms requiring a follow-up call to the surgeon are listed.